Why Fatigue Happens
Chemotherapy‑induced fatigue (CIF) affects more than 80 % of patients receiving chemo or radiation and is distinct from ordinary tiredness because rest or sleep does not fully relieve it. The fatigue is driven by several physiological mechanisms. Cytokine release during treatment triggers inflammation that alters brain signaling, while anemia and reduced oxygen delivery, as well as cancer‑related cachexia, lower tissue energy supply. Muscle loss and metabolic disturbances further deplete stamina. These changes translate into everyday challenges: patients often feel exhausted after minimal activity, struggle to concentrate, and may need frequent naps that still leave them drained. Simple tasks such as dressing, cooking, or walking short distances can feel overwhelming, leading to a loss of independence and increased reliance on caregivers. Recognizing these effects is the first step toward targeted interventions. The constant tiredness also amplifies anxiety and depression, creating a cycle where mental strain worsens physical exhaustion and improve overall mood.
1. Move to Gain Energy
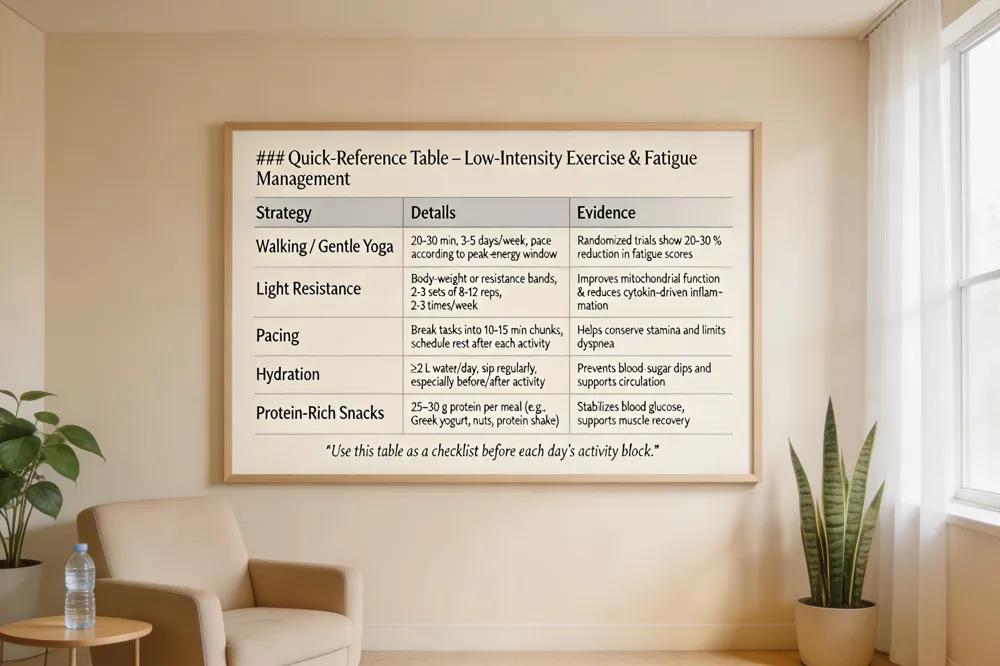 Low‑intensity aerobic exercise is a cornerstone of cancer‑related fatigue management. Walking, gentle yoga, or light resistance training for 20‑30 minutes most days (about 3‑5 hours per week) has been shown in randomized trials to cut fatigue scores by 20‑30% and improve mood. The benefit comes from enhanced circulation, better mitochondrial function, and reduced cytokine‑driven inflammation.
Cancer‑related fatigue management – Begin with a thorough assessment to identify treatable factors such as anemia, pain, sleep disruption, or nutritional gaps. Incorporate pacing strategies and a regular activity schedule that includes low‑impact exercise, consistent sleep hygiene, balanced nutrition, hydration, and psychosocial support.
What can help with chemo fatigue? – Short, regular walks or gentle yoga boost energy and mood; staying hydrated and eating protein‑rich, frequent meals prevent blood‑sugar dips; treating anemia with iron or erythropoietin when indicated; practicing good sleep hygiene (cool, dark room, short daytime naps) and addressing emotional distress through counseling or mindfulness.
Chemo fatigue and breathlessness – Often linked to anemia or lung inflammation. Medical evaluation (CBC, imaging) guides targeted treatments (iron, bronchodilators, fluid drainage). Complementary measures include paced walking, diaphragmatic breathing, stretching, and adequate hydration to rebuild stamina while minimizing dyspnea.
How to get rid of chemo fatigue? – Hydrate well, eat small protein‑dense meals, engage in gentle activity, conserve energy by planning tasks during peak alertness, take brief naps, and discuss persistent fatigue with the oncology team for possible medical interventions.
2. Nutrition & Hydration Power‑Ups
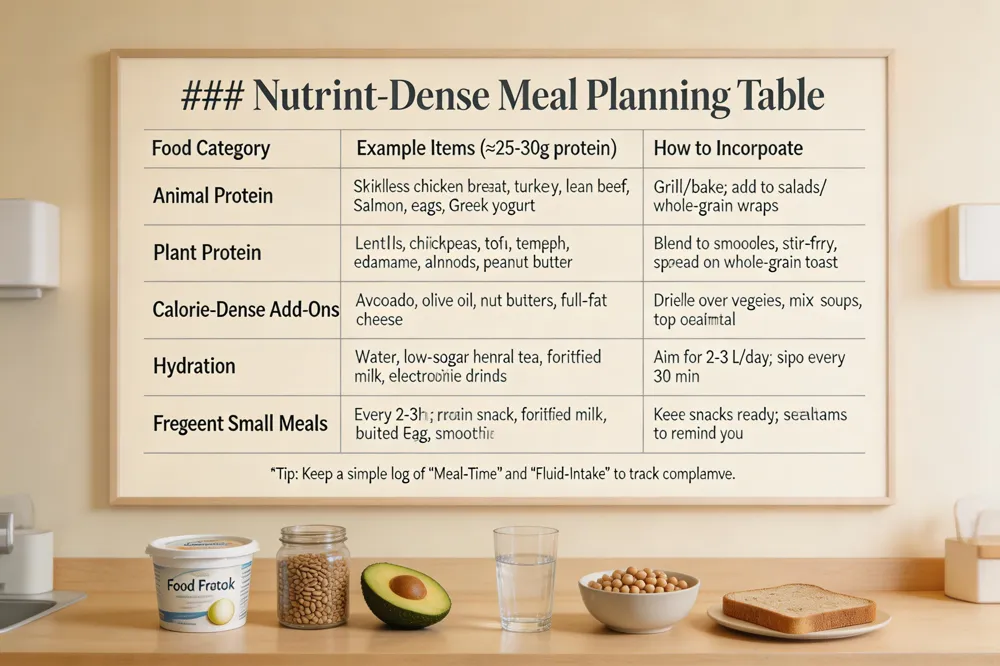 Protein‑rich foods – Cancer patients benefit from high‑quality animal proteins such as skinless chicken, turkey, lean beef, pork, lamb, salmon, shrimp, eggs and dairy (Greek yogurt, cottage cheese, milk, hard cheese). Plant‑based sources include beans, lentils, chickpeas, tofu, tempeh, soy milk, edamame, almonds, peanuts, nut butters, seeds (pumpkin, sunflower, chia, hemp) and grain‑based additions like wheat germ or fortified cereals. When whole foods fall short, protein powders or ready‑to‑drink shakes can boost intake to the recommended 25–30 g per meal.
Frequent small meals – Eating every 2–3 hours stabilizes blood‑sugar and prevents energy crashes. Easy, nutrient‑dense options—fortified milk, nut‑butter toast, boiled eggs, pureed soups, smoothies with protein powder—are ideal when appetite is low.
Calorie‑dense options – Adding healthy fats (avocado, olive oil, butter, nut butters) and calorie‑rich foods (full‑fat dairy, fortified milk, cheese) provides extra energy without large volumes.
Hydration importance – Aim for at least 2–3 L of fluid daily (water, low‑sugar teas, nutrient‑rich drinks). Dehydration worsens fatigue and cognitive fog.
Q&A
- High protein foods: See list above; include animal and plant sources plus protein powders if needed.
- Energy boost: Small, frequent protein‑fat meals, stay hydrated, nap ≤1 hour, maintain regular light activity.
- 5 P’s: Plan, Prioritise, Pace, Position, Permission – a framework for scheduling rest and activity.
- Gain energy during chemo: Align tasks with peak alertness, hydrate, eat balanced snacks, limit alcohol/caffeine, do gentle exercise, seek support, and discuss treatable causes (anemia, depression) with the care team.
3. Sleep Hygiene & Energy‑Conservation
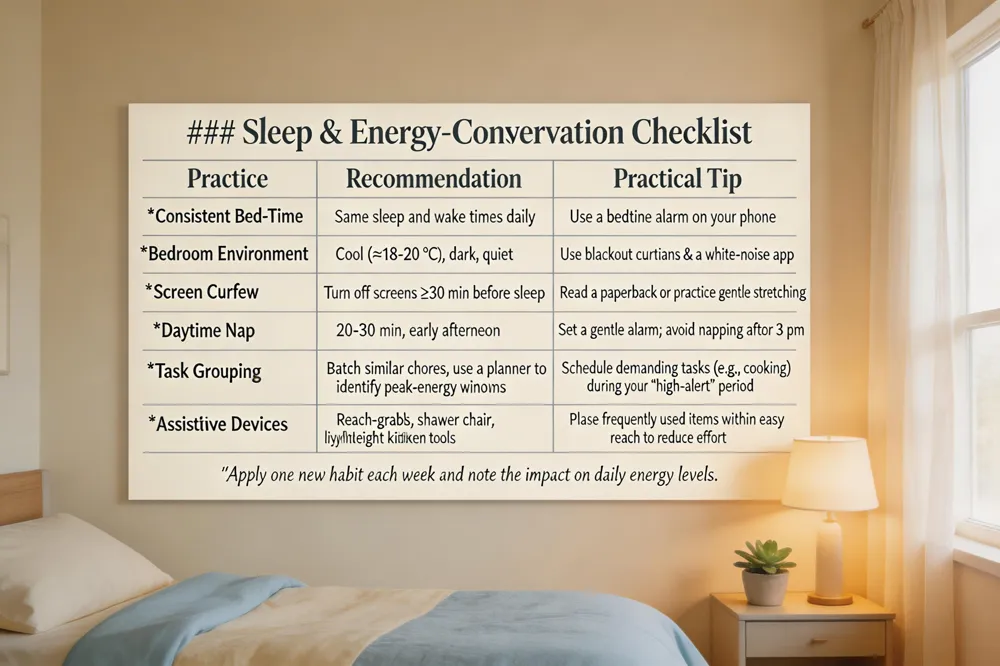 A regular sleep‑wake routine is the cornerstone of fatigue management. Go to bed and rise at the same time each day, keep the bedroom cool, dark and quiet, and turn off screens at least 30 minutes before sleep. Short daytime naps are helpful, but limit them to 20‑30 minutes and schedule them early in the afternoon to avoid disrupting night‑time rest.
Pace your day by grouping similar tasks, using a planner to identify peak‑energy windows, and taking a 5‑10 minute break after each activity. Energy‑conservation strategies such as delegating chores, using adaptive devices (e.g., reachers, shower chairs), and sitting while cooking or dressing reduce expendable effort.
Cancer fatigue vs normal fatigue – Cancer‑related fatigue is far more intense, persistent, and unrelieved by ordinary rest; it often includes brain‑fog, anxiety, and emotional exhaustion, whereas normal fatigue resolves with sleep or reduced activity.
Cancer fatigue after treatment – It can linger for months, worsened by anemia, poor nutrition, or sleep disturbances. Gentle aerobic activity, balanced meals, hydration, and pacing improve stamina; discuss persistent fatigue with your oncology team for possible medical interventions.
Stage 4 cancer sleeping all the time – Continuous drowsiness may signal disease progression, anemia, pain, or depression. A thorough evaluation (blood work, medication review, mood screening) is essential; management includes scheduled naps, energy‑conserving techniques, nutrition, and targeted therapies for underlying causes.
The 5 P’s of fatigue management – Plan, Prioritise, Pace, Position, and Permission: schedule rest, rank tasks, move gradually, adopt comfortable postures, and allow yourself permission to rest when needed.
4. Managing Emotional & Cognitive Load
 Does breast cancer make you tired before treatment? Yes. Fatigue often precedes any therapy because the tumor releases cytokines, can cause anemia, and disrupts metabolism. The emotional stress of a new diagnosis adds anxiety and depression, deepening the sense of exhaustion that is not relieved by rest.
Does cancer make you tired before treatment? The cancer itself can trigger systemic inflammation, hormonal changes, and pain, all of which drain energy. Psychological distress and sleep disturbances further amplify tiredness. Early discussion with the oncology team is essential.
Cancer fatigue symptoms Patients describe a pervasive, heavy tiredness that persists despite sleep, muscle sluggishness, short‑of‑breath on minimal activity, and “brain fog” (difficulty concentrating, remembering). Emotional signs include low motivation, sadness, and anxiety.
Cancer fatigue treatment Identify reversible causes (anemia, pain, sleep issues). Implement low‑intensity aerobic activity (walking, gentle yoga) timed to energy peaks. Use stress‑reduction techniques—deep breathing, progressive muscle relaxation, and mindfulness meditation to lower cortisol. Cognitive‑behavioral therapy (CBT) addresses maladaptive thoughts and improves sleep hygiene. Psychosocial support (counseling, support groups) combats depression and anxiety. When needed, clinicians may consider modest agents or treat anemia.
Things I wish I had during chemo A clear treatment roadmap, a dedicated supportive‑care nurse, easy‑to‑digest nutrition, pre‑planned hair‑loss strategies, and readily available emotional‑support resources (therapist, peer group, mindfulness apps) would have eased both physical fatigue and the mental load.
5. Practical Tools & Support Resources
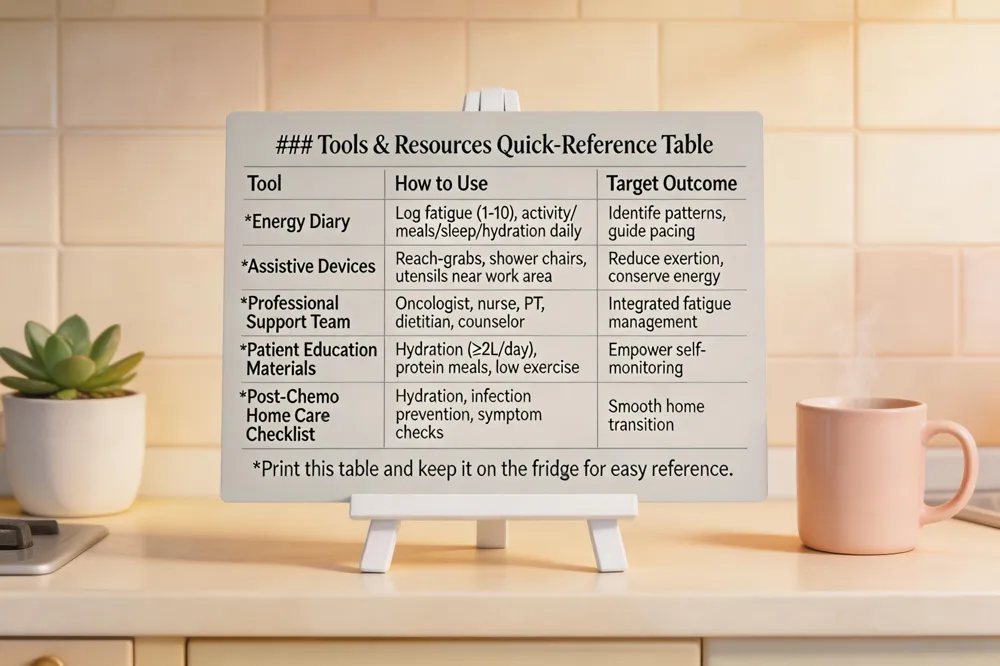 Using an energy diary helps patients track when fatigue peaks, what activities trigger low energy, and how sleep, nutrition, and hydration (≥2 L/day) affect stamina. Logging this information enables the oncology team to tailor pacing schedules and identify treatable contributors such as anemia or medication side‑effects.
Assistive devices—including reach‑grabs, shower chairs, and lightweight kitchen tools—reduce the physical effort required for daily chores, conserving precious energy for essential tasks. Simple modifications, like placing frequently used items within easy reach, further lower exertion.
The professional support team should be multidisciplinary: oncologists, oncology nurses, physical therapists, dietitians, and mental‑health counselors collaborate to address medical, nutritional, and emotional aspects of fatigue. Regular check‑ins allow timely adjustments to treatment, pain control, and psychosocial interventions such as CBT or mindfulness.
Patient education equips individuals with knowledge about hydration (≥2 L/day), protein‑rich small meals, sleep hygiene, and safe low‑intensity exercise (e.g., 10‑minute walks). Understanding how to self‑monitor symptoms and when to contact the care team empowers patients to manage fatigue proactively.
Post chemotherapy care at home – focus on infection prevention, stay hydrated, eat nutrient‑dense small meals, incorporate gentle activity, and monitor for fever, pain, or new symptoms, contacting the oncology team promptly.
How long does chemo fatigue last – acute fatigue peaks during treatment cycles and usually subsides within weeks after a cycle, but can linger for months; chronic fatigue may persist for years, especially with anemia or emotional stress.
Long‑term fatigue after chemotherapy – may persist for months or years; address reversible factors, adopt graded exercise, energy‑conservation, and multidisciplinary support to improve quality of life.
Chemo fatigue Taxol – Taxol‑induced fatigue stems from marrow suppression and inflammation; management includes dose adjustments, hydration, balanced meals, short naps, and activity pacing.
What is the hardest part of cancer treatment? – The greatest challenge is the profound uncertainty of disease response and therapy effectiveness, compounded by emotional strain and evolving treatment plans.
Putting It All Together
Creating a routine starts with mapping the day around natural energy peaks. Begin mornings with a brief stretch or 10‑minute walk, then schedule the most demanding tasks—appointments, paperwork, or chores—when you feel most alert, usually mid‑morning. Insert short, 15‑minute rest periods after meals or chemotherapy, and keep a water bottle and protein‑rich snacks such as Greek yogurt or nut butter on crackers within easy reach. Share this plan with the Hirschfeld Oncology team; ask the nurse or dietitian to review hydration goals, sleep‑hygiene tips, and any medication changes that could affect fatigue. Track energy, activity, and symptoms each day in a fatigue diary, and discuss the log with your oncologist every two weeks to adjust the strategy.





.png)


.png)
.png)




