When we talk about ovarian cancer, one of the first things to understand is who it affects most often. The simple answer is that it's a disease that predominantly strikes later in life. In fact, the average age for an ovarian cancer diagnosis is 63 years old.
This number is more than just a statistic; it tells a story. It confirms that ovarian cancer is most common in postmenopausal women. While it's certainly possible for a woman to be diagnosed at any age, the risk isn't spread evenly across her lifetime. It changes dramatically as the years go by.
The Age Distribution of Ovarian Cancer
You can think of a woman's lifetime risk for ovarian cancer almost like a steep hill. The climb is slow and gradual in her younger years, but it gets much steeper and more significant after menopause. A diagnosis in a woman's 20s or 30s is quite rare. The likelihood really starts to pick up after age 55.
This age-related pattern is a key part of the disease's biology. The cellular changes that eventually lead to cancer don't happen overnight. They often accumulate over many years, which helps explain why risk builds up over a lifetime.
A Closer Look at the Numbers
The statistics paint a very clear picture. Data from the National Cancer Institute shows a definite shift toward older age groups. Looking at cases from 2015 to 2019, more than two-thirds of all ovarian cancer diagnoses were in women aged 55 or older. Drilling down even further, nearly half of all new cases occurred in women 65 and above.
This bar chart gives a great visual breakdown of how new cases are distributed across different age groups.
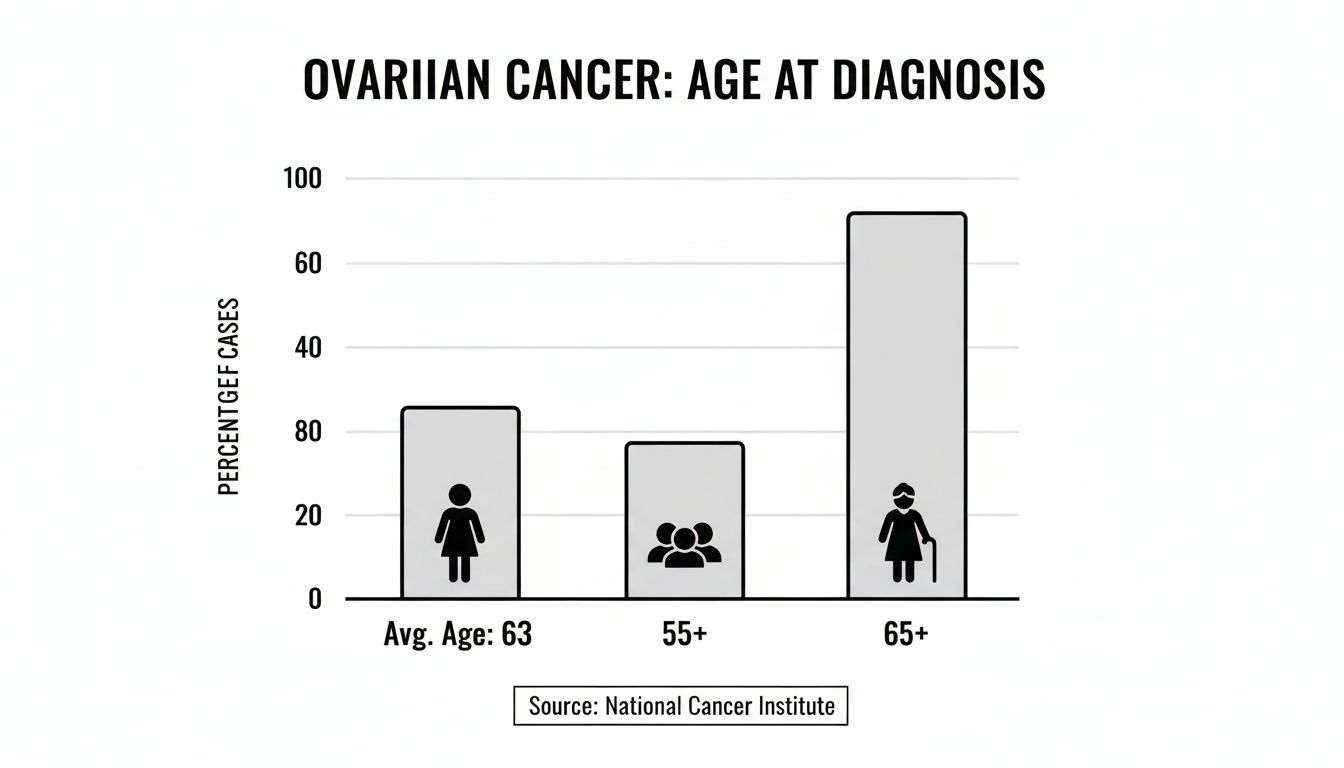
As the chart shows, while 63 is the average age, the risk is heavily weighted toward the postmenopausal years. For more in-depth information, the Ovarian Cancer Research Alliance is an excellent resource for statistics and their implications.
To give you an even more precise view, this table breaks down the percentage of new cases diagnosed within specific age brackets.
Ovarian Cancer Incidence by Age Group (2015-2019)
This data really drives home the main point: the average age for ovarian cancer reflects a risk that climbs steadily through a woman's 40s and 50s, peaking in her 60s and early 70s.
Understanding this age distribution is the first step in being proactive about your health. It helps you know when to be most vigilant about potential symptoms. Of course, this is just the general timeline. As we'll discuss next, specific cancer subtypes and personal risk factors can significantly alter this picture.
How Different Ovarian Cancer Types Affect Age

While 63 is the number you'll often hear cited as the average age for an ovarian cancer diagnosis, it’s just that—an average. The reality is far more nuanced. Thinking of ovarian cancer as a single disease is a common misconception; it’s actually an umbrella term for a group of distinct cancers, each with its own story, behavior, and typical age of onset.
The most common type, by a long shot, is epithelial ovarian cancer. This group accounts for about 90% of all cases and develops from the cells on the outer surface of the ovary or fallopian tube. This is the cancer that aligns most closely with the "average age" statistic, as it primarily affects postmenopausal women. The risk for this specific type tends to grow as a woman gets older.
But what about the other 10%? This is where the story diverges significantly, particularly for younger women.
Younger Onset Cancers: Germ Cell and Stromal Tumors
Some of the rarer forms of ovarian cancer start in completely different types of ovarian cells, and as a result, they follow a much different timeline. This is why a diagnosis in a 25-year-old can look vastly different from one in a 65-year-old.
Two important examples to know are:
- Germ Cell Tumors: These cancers grow from the very cells that produce eggs (the ova). While they are rare—making up less than 5% of all ovarian cancers—they are the most common type we see in teenagers and women in their 20s.
- Stromal Tumors: These tumors develop from the connective tissue cells that hold the ovary together and produce hormones like estrogen and progesterone. They can technically appear at any age, but they are often diagnosed in younger women compared to epithelial cancers.
This distinction is absolutely critical. It shifts the conversation from a single average age for ovarian cancer to a more precise, type-specific understanding. In fact, a patient’s age at diagnosis is often one of the first and most powerful clues we have about which subtype of cancer we might be dealing with. You can dive deeper into the specifics of diagnosis and the various forms this disease can take in our comprehensive guide to understanding ovarian cancer.
The key takeaway is that ovarian cancer is not one disease. The type of cell where the cancer begins—epithelial, germ, or stromal—is a major factor in determining the typical age of diagnosis, treatment approach, and prognosis.
To make this easier to visualize, here's a breakdown of the main ovarian cancer subtypes and the age ranges they most commonly affect.
Ovarian Cancer Subtypes and Typical Age of Onset
Understanding these differences is the first step toward appreciating why a personalized diagnosis and treatment plan is so essential in managing this complex disease.
Personal Risk Factors That Shift Your Timeline

While it’s helpful to know the average age for ovarian cancer, that number is just a starting point. Your personal risk profile is what really tells the story. Think of the average age as a general landmark; specific factors in your own life can shift your personal timeline, sometimes significantly.
The single biggest influence is genetics. Most ovarian cancers are considered sporadic, meaning they seem to happen by chance. But for a meaningful portion—up to 20% of cases—the cancer is tied directly to an inherited genetic mutation.
The Power of Your Family Health Story
Your family’s health history is one of the most powerful tools you have. It acts as a kind of roadmap, highlighting potential risks that might otherwise go completely unnoticed. A pattern of certain cancers in your family tree should be a major signal, even if no one was ever officially tested for a specific genetic mutation.
This is especially true when it comes to hereditary cancer syndromes. These conditions don't just raise your lifetime risk; they often dramatically lower the age when cancer might appear.
For individuals with a hereditary cancer syndrome, such as one involving a BRCA1 or BRCA2 mutation, the average age of an ovarian cancer diagnosis can drop by 10 to 30 years. This is a massive shift, and it’s why a diagnosis in your 40s or even 30s becomes a real possibility for some families.
The most widely recognized syndromes include:
- BRCA1 Mutations: Women carrying a BRCA1 mutation face a lifetime ovarian cancer risk of up to 44%. The risk begins to climb steeply in their late 30s and early 40s.
- BRCA2 Mutations: The lifetime risk is a bit lower, at up to 17%. While lower than BRCA1, this is still a substantial increase compared to the general population's risk of just over 1%.
- Lynch Syndrome: Linked to mutations in genes like MLH1 and MSH2, this syndrome also elevates the risk of ovarian cancer, with a lifetime risk reaching up to 12%. It's also strongly associated with colorectal and uterine cancers.
Other Conditions That Impact Your Risk
Genetics aren't the whole picture. Other aspects of your personal health can also nudge your risk profile. For instance, a diagnosis of endometriosis, a painful condition where uterine-like tissue grows elsewhere in the pelvis, has been linked to a higher risk of specific ovarian cancer subtypes, namely clear cell and endometrioid carcinomas.
Your reproductive history matters, too. Things like starting your period at a very young age, never giving birth, or going through menopause later than average can slightly increase your risk. The common thread here is thought to be the total number of times you ovulate in your lifetime. On the flip side, factors like having multiple pregnancies or using oral contraceptives for several years appear to offer some protection.
At the end of the day, your risk isn't a fixed number. It’s a dynamic picture shaped by your genes, your health, and your life story. This is exactly why a one-size-fits-all approach to the average age of ovarian cancer just doesn’t work.
Recognizing Symptoms at Every Stage of Life
Ovarian cancer is often called a “silent” disease, but this is a bit of a misnomer. The truth is, it does have symptoms. The challenge is that they're often subtle and can easily be mistaken for more common, everyday health complaints. Learning to listen to your body and understand these signals within the context of your age and life stage is crucial.
The most common signs include persistent bloating, pelvic or abdominal pain, feeling full quickly even after eating little, and needing to urinate more often. Since these are so general, context is everything. For instance, a younger, premenopausal woman might quickly dismiss persistent bloating as a normal part of her menstrual cycle or maybe a reaction to something she ate.
For a postmenopausal woman, however, that very same symptom should raise a much bigger red flag. The key things to watch for are symptoms that are new, persistent, and show up frequently.
Interpreting Symptoms Across the Lifespan
Think of your body as having a familiar, baseline rhythm. A huge part of early detection is simply noticing when that rhythm changes and, importantly, doesn’t return to normal after a week or two.
In Younger Women (20s-40s): Be on the lookout for symptoms that might seem related to your period but suddenly become worse, more frequent, or just don't go away like they used to. If your typical pre-period bloating used to last a couple of days but now hangs around for two straight weeks, that's a significant change worth discussing with your doctor.
In Postmenopausal Women (50+): The appearance of any new pelvic symptoms is your cue to see a doctor right away. Without the monthly hormonal shifts of a menstrual cycle, there are fewer simple, benign explanations for issues like new-onset bloating or pelvic pressure.
Trust your intuition. If you feel that something is persistently "off," especially if the symptoms are new and occur more than 12 times a month, it’s time to speak with a doctor. This is true no matter the average age for ovarian cancer—your personal experience is what counts.
Keeping a simple log of your symptoms can be an incredibly powerful tool. Jotting down what you're feeling, how often it happens, and how intense it is creates a clear record to share with your physician. It turns vague feelings into concrete data they can act on.
Beyond symptoms, certain diagnostic tools can offer more clarity. While you can learn more about how a CT scan might detect ovarian cancer in our other guides, simpler tests are often the first step. For example, a specialized CA-125 blood test for ovarian health is designed to measure specific tumor markers in the blood.
When you finally talk to your doctor, be as specific as possible. Instead of just saying, "I feel bloated," try describing it in detail: "For the past three weeks, I've had noticeable bloating every single day that makes my pants feel tight, and it doesn't seem to be related to my diet." This direct, factual approach helps your doctor grasp the persistence and severity of the issue, ensuring you get the attention and care you deserve.
How Age Shapes Ovarian Cancer Treatment and Prognosis

When my team and I sit down to create an ovarian cancer treatment plan, a patient's age is a critical piece of the puzzle. We’re not just treating the cancer; we’re treating the person who has it. Their stage in life, overall health, and personal goals all play a huge role in the decisions we make together. The conversation we have with a 35-year-old and a 75-year-old, even with the same diagnosis, will look very different.
For instance, a younger woman with an early-stage cancer might have fertility preservation as her top priority. When it's oncologically safe, we can adapt surgical techniques to preserve an ovary and the uterus. This approach carefully balances the immediate need to treat the cancer with the deeply personal desire to protect her future family-building options.
On the other hand, for an older patient, the focus often shifts. The primary goals may be to treat the cancer as effectively as possible while carefully managing other health conditions to maintain a high quality of life.
Tailoring Treatment to the Individual
As women get older, they are more likely to have other health issues, which we call comorbidities. These can include things like heart conditions, diabetes, or kidney problems, all of which influence how well a person can tolerate standard cancer treatments like extensive surgery or high-dose chemotherapy.
An oncologist has to weigh these factors with great care. Moving ahead with a standard protocol that’s too aggressive could do more harm than good, depleting a patient's strength and their ability to fight the cancer.
A patient's biological age—how healthy they are—is often more important than their chronological age. A fit 80-year-old might tolerate a more intensive treatment plan than a 65-year-old with multiple serious health issues. The goal is always to match the treatment intensity to the patient's overall health and personal wishes.
This is exactly where personalized medicine makes such a difference. Advanced, customized strategies can offer a lifeline, especially for patients who aren't ideal candidates for a traditional, one-size-fits-all chemotherapy regimen.
Personalized Medicine and Quality of Life
At Hirschfeld Oncology, our entire philosophy is built on finding this precise balance. By using targeted therapies and refined chemotherapy regimens, we can zero in on the cancer cells while sparing healthy tissues as much as possible. This approach often results in fewer side effects and a much better quality of life during treatment.
This kind of individualized care really means:
- Focusing on the Patient’s Goals: Treatment decisions are a collaboration. We make sure the plan aligns with what matters most to the patient and their family.
- Managing Comorbidities: We coordinate care to manage every aspect of a patient’s health, not just the cancer.
- Prioritizing Well-Being: Our aim is to find the most effective treatment that also allows the patient to keep living their life as fully as possible.
Ultimately, age provides important context, but it’s the individual—their health, their goals, and the specific biology of their cancer—that truly dictates the best path forward. This patient-first approach ensures that every person, regardless of whether they fit the average age for ovarian cancer, receives care designed just for them.
Finding Advanced Ovarian Cancer Care in New York
Knowing your personal risk factors and understanding the statistics around the average age for ovarian cancer is an empowering first step. The next, and most crucial, is finding a medical team you can trust to build a truly personalized care plan—especially if you're navigating a complex or advanced diagnosis here in the New York City area.
It doesn’t matter if you fit the typical age profile or are one of the younger women diagnosed; you need and deserve a treatment strategy built just for you. Here at Hirschfeld Oncology, our entire philosophy is built around that idea. We focus on achieving powerful results with less toxicity, always prioritizing your quality of life.
Your Next Step Toward Hope
For patients across all of New York's boroughs, from Brooklyn to Manhattan and beyond, expert guidance is closer than you think. Our team is here to help if you're exploring options after standard treatments have failed, seeking a second opinion on a difficult case, or need a specialist in treatment-resistant disease.
Dr. Hirschfeld's expertise lies in creating highly individualized treatment regimens. He uses sophisticated therapies that are not only effective but also manageable, with the goal of restoring hope by providing clear, advanced options that align with your personal health and life goals.
We specialize in helping patients find a path forward, even when the diagnosis is complex. If you're currently gathering information, you may find our guide on how to find the best ovarian cancer doctors near me helpful.
Taking that first step to request a consultation can open the door to new possibilities and a renewed sense of control, guided by expertise and genuine compassion.
Frequently Asked Questions About Ovarian Cancer and Age
We’ve covered a lot of ground exploring the connection between age and ovarian cancer, but it's a topic that often leaves people with more questions. Let's tackle some of the most common ones head-on to clear up any lingering confusion about the average age for ovarian cancer.
Can Ovarian Cancer Affect Very Young Women?
Yes, it can, but it's exceptionally rare. The vast majority of ovarian cancers are found in women who have already gone through menopause. However, certain types of ovarian tumors are more likely to appear in younger women. For instance, germ cell tumors, which develop in the egg cells of the ovary, are most often diagnosed in teenagers and women in their 20s.
This is a critical point. A diagnosis in a younger woman almost always points to a different kind of cancer than the more common epithelial tumors affecting older women. This distinction is vital because it completely changes the treatment strategy.
Is the Average Age of Diagnosis Changing?
The average age at diagnosis has held pretty steady over the years, usually landing in the early 60s. What has changed is our understanding of the disease itself. We now know that "ovarian cancer" isn't one single disease but a collection of different cancers, each with its own typical timeline and behavior.
Another factor is the rise of genetic testing and greater awareness. Women who discover they have a high inherited risk might be diagnosed younger, either through more vigilant screening or because they've opted for risk-reducing surgery. It really underscores how important it is to know your family's health history.
The key takeaway is this: while broad statistics offer a general picture, your personal risk profile is what truly counts. Genetic factors can dramatically shift your individual timeline away from the population average.
Who Should Consider Genetic Testing for BRCA Mutations?
Genetic testing for mutations like BRCA1 and BRCA2 is an incredibly powerful tool, but it's not for everyone. It’s a conversation worth having with your doctor or a genetic counselor, especially if any of the following apply to you:
- You have a personal history of ovarian, fallopian tube, or peritoneal cancer.
- You have a personal history of breast cancer, particularly if diagnosed before age 50.
- A known BRCA mutation has already been identified in your family.
- A close relative, like your mother, sister, or daughter, has had ovarian cancer.
- Your family history includes several relatives with breast, ovarian, pancreatic, or high-grade prostate cancer.
Knowing your genetic status can transform the average age of ovarian cancer from a distant statistic into a personalized and actionable piece of information.
At Hirschfeld Oncology, we believe that an informed patient is an empowered patient. If you're facing an advanced or treatment-resistant ovarian cancer diagnosis in the New York City area, our team is here to provide personalized, low-toxicity care. You can learn more about our philosophy and find helpful resources on our blog.





.png)


.png)
.png)




