When you’re navigating a prostate cancer diagnosis, your doctor might mention a bone scan. It's a key imaging test, but the recommendation alone can be unsettling. Let's clear up what it is and, more importantly, why it's used.
A bone scan is essentially a skeletal map used to see if cancer has spread, or metastasized, from the prostate to your bones. This is a critical piece of the puzzle for figuring out the cancer's stage and charting the best course for treatment.
Why Your Doctor Recommended a Bone Scan
First, it's important to know that a bone scan isn't a test for primary bone cancer. Its job is to answer one very specific question: has the prostate cancer traveled beyond the prostate gland and taken up residence in the bones?
When aggressive prostate cancer cells break away from the main tumor, they can journey through the bloodstream or lymphatic system. The bones are, unfortunately, a common landing spot. If cancer is found in the bones—a condition called bone metastasis—it completely changes the game, affecting the cancer's stage and the entire treatment strategy.
It's Like a Smoke Detector for Your Skeleton
Here’s a helpful way to think about it: a bone scan acts like a highly sensitive smoke detector for your skeleton.
It doesn't see the "fire" (the cancer cells themselves). Instead, it detects the "smoke"—the bone's reaction to the cancer's presence. When cancer cells invade bone, they disrupt the normal, balanced process of bone breakdown and rebuilding. This disruption kicks the bone-rebuilding cells into overdrive as they try to repair the damage. The bone scan is designed to pinpoint these areas of frantic activity, which show up as "hot spots" on the final image.
Triggers for Ordering a Scan
Doctors don't order a bone scan for every man diagnosed with prostate cancer. It’s typically reserved for situations where there's a reason to suspect the cancer might have spread.
The decision is usually based on a few key risk factors:
- Elevated PSA Levels: A high or rapidly climbing Prostate-Specific Antigen (PSA) level often signals a more aggressive cancer.
- High Gleason Score: This score comes from the biopsy and grades how abnormal the cancer cells look. A higher score (usually 7 or more) raises the concern for spread.
- Advanced Clinical Stage: If a digital rectal exam or other imaging suggests the tumor has grown outside the prostate capsule, a bone scan is a logical next step.
- Symptoms: This is a big one. Any new or persistent bone pain—especially in the back, hips, or ribs—is a major red flag for bone metastases and will almost certainly trigger a scan.
We often get asked how likely it is for the cancer to have already spread at diagnosis. The data backs up these clinical triggers. A 2022 study, for instance, showed that 23% of newly diagnosed prostate cancer patients already had bone metastases, and the risk was strongly linked to higher PSA levels and Gleason scores.
At Hirschfeld Oncology, we look at this complete picture before recommending any specific imaging. It’s a crucial part of how we approach staging for the various cancers we treat.
To make it clearer, here’s a quick summary of when and why a scan is usually ordered.
When and Why a Bone Scan Is Recommended
This table breaks down the most common clinical situations that lead to a bone scan recommendation and what we're looking for.
Ultimately, a bone scan gives your oncology team a vital piece of information to ensure your treatment plan is built on a complete and accurate understanding of your cancer.
What to Expect During Your Bone Scan
Knowing what happens during a bone scan can make the whole experience feel much less intimidating. It's a pretty straightforward process that breaks down into three simple parts: the injection, a bit of a wait, and then the scan itself. Let's walk through it step-by-step so you know exactly what’s coming.
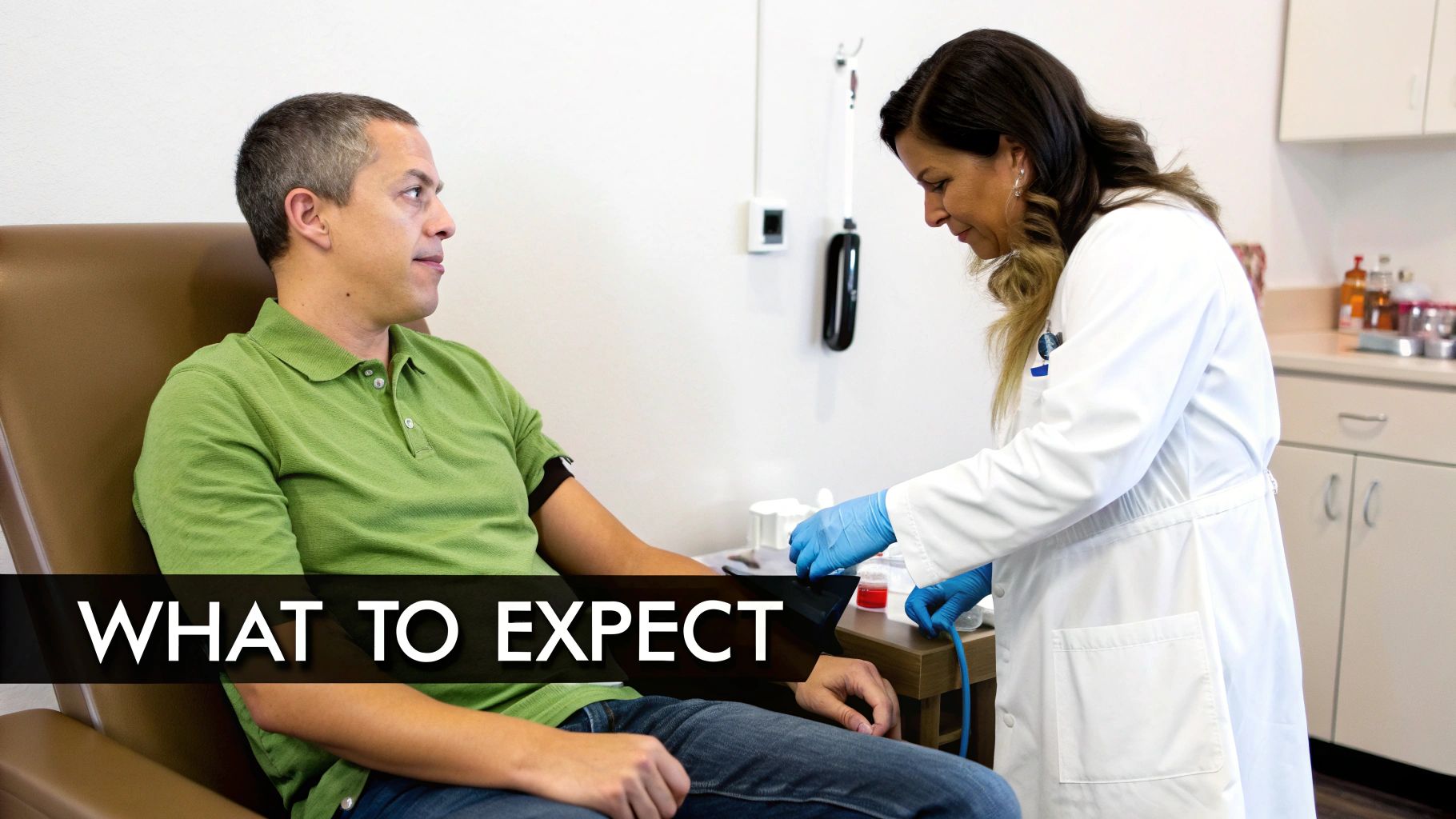
The good news is, there's not much you need to do to get ready. You can usually eat and drink normally beforehand and take your medications as scheduled. Just double-check with your doctor’s office in case they have any specific instructions for you.
Phase 1: The Injection
First things first, you'll get a quick injection of a radioactive substance, which we call a tracer. It goes into a vein in your arm, just like getting a blood test. The dose of radiation is tiny—about the same as a standard X-ray—so it's considered very safe.
This tracer is the magic ingredient. You can think of it like a special dye that’s drawn to areas where your bones are more active. Once it's in your bloodstream, it needs some time to make its way to your skeleton, which brings us to the next step.
Phase 2: The Waiting Period
After the shot, there's a waiting period of about two to four hours. This is a crucial pause. It gives the tracer enough time to travel through your body and settle into your bones, especially in spots where bone cells are busy repairing damage. That activity could be from something harmless like arthritis or an old injury, but it can also be a sign of cancer.
They’ll ask you to drink a few glasses of water during this time. Why? It helps flush out any extra tracer that your bones don't absorb, leading to a much sharper and clearer final image. You can often leave the clinic during this wait; just be sure you know exactly when they need you back.
Key Takeaway: That two-to-four-hour wait isn't just empty time. It's what allows the tracer to highlight the precise areas your oncologist needs to examine, making the whole scan as effective as possible.
Phase 3: The Imaging Process
When it's time for the scan, you'll lie on a padded table that moves through a large, open scanner. A special device called a gamma camera will pass slowly over and under you.
This camera isn't giving off any radiation. Instead, it's detecting the faint energy signals from the tracer that has collected in your bones. It uses those signals to build a detailed picture of your entire skeleton.
The most important thing you have to do is lie as still as possible to make sure the images aren't blurry. The scan is completely painless and usually takes about 30 to 60 minutes. After that, you're all done. You can head home and get back to your day, and the tracer will naturally pass out of your system over the next 24 to 48 hours.
How to Understand Your Bone Scan Results
Once the scan is done, the images go to a radiologist—a doctor who specializes in medical imaging. They’ll carefully analyze everything and send a detailed report to your oncologist. Sitting down to go over that report is the next big step, and it usually points to one of two main outcomes.

A negative result is what everyone hopes for. This means the scan shows the radioactive tracer spread evenly throughout your skeleton, with no unusual areas lighting up. It’s a good sign that, as far as this test can see, there’s no evidence of prostate cancer in your bones.
A positive result, on the other hand, means the scan found one or more "hot spots." These are areas where the tracer has gathered, signaling a flurry of bone-rebuilding activity.
Decoding Hot Spots
Now, this is the crucial part: a hot spot does not automatically mean cancer. A bone scan is great at detecting activity—it's very sensitive—but it can't always tell you why the activity is happening. Think of it like a smoke detector; it tells you there's smoke, but it doesn't know if it's from burnt toast or a real fire.
Plenty of benign (non-cancerous) conditions can cause a bone to light up on a scan, including:
- Arthritis: Joint inflammation is one of the most common culprits behind hot spots.
- Old Injuries: A bone that was fractured years ago can still show signs of healing and repair.
- Infections: Though less common, a bone infection will also trigger increased cellular activity.
- Other Bone Diseases: Conditions like Paget's disease can also show up as hot spots.
This is where your oncologist puts on their detective hat. They’ll look at the location of the hot spots and cross-reference them with your symptoms, a physical exam, and often other imaging like X-rays or CT scans to figure out the most likely cause.
If your report mentions hot spots, try not to assume the worst. Your doctor sees this as one clue in a much larger puzzle. More often than not, they’ll need to do more investigating to confirm what these spots really are.
Measuring the Big Picture with the Bone Scan Index
When bone metastases are confirmed, doctors need a way to measure the overall extent of the cancer's spread. Simply counting spots can be misleading. That’s where a tool called the Bone Scan Index (BSI) comes in.
The BSI is a percentage that estimates how much of your total skeleton is affected by cancer. It’s a much more objective and reliable way to quantify the "tumor burden" in your bones.
Specialized software calculates this number, giving your care team powerful information for planning your treatment and understanding your prognosis. For example, studies have shown that a higher BSI often points to a more aggressive disease. One major study found that a BSI greater than 3.5% was linked to a higher mortality risk, showing just how important it is to have a clear, quantified picture of skeletal involvement. You can read more about the prognostic value of BSI in prostate cancer.
In the end, your bone scan gives your medical team a critical snapshot of your bone health. Your oncologist will walk you through the report, explain what it means for you personally, and map out the next steps in your treatment plan.
The Strengths and Limitations of Bone Scans
No medical test is perfect, and that definitely includes bone scans. To really grasp its role in prostate cancer care, you have to understand what it does exceptionally well—and where it falls short. It's just one piece of a much larger diagnostic puzzle, and knowing its pros and cons is key.
The biggest strength of a bone scan is its high sensitivity. Think of it like a smoke detector with the sensitivity cranked all the way up. It’s fantastic at picking up even tiny changes in bone activity anywhere in the body, often long before a patient would ever feel something like bone pain. This makes it a great first-pass tool for surveying the entire skeleton for potential trouble.
The Challenge of Non-Specificity
But that high sensitivity comes with a major trade-off: non-specificity. This is the scan's main limitation. While it’s great at telling you that something is happening in the bone, it often can’t tell you why.
The scan simply highlights any area where bone is remodeling or turning over more quickly than usual. That could absolutely be cancer, but it also lights up for all sorts of benign, everyday reasons:
- Arthritis and joint inflammation
- A healing fracture from an old injury
- Bone infections or other metabolic bone diseases
This is where "false positives" come from. A hot spot shows up on the scan, raising alarm bells, but it turns out to be caused by a completely harmless condition. That can lead to a lot of unnecessary anxiety and more tests.
A key takeaway is that a bone scan identifies areas that need a closer look, but it rarely provides the final answer on its own. It raises the question; it doesn't always answer it.
The Risk of Overuse and False Alarms
This limitation is a big deal when you consider how often bone scans are still used. While guidelines recommend using them selectively based on a patient's risk, they’re still a very common part of the workup. Unfortunately, some studies have shown that roughly 50-60% of positive bone scans during initial prostate cancer staging can be false positives. This can trigger a cascade of unnecessary follow-up procedures, like more imaging or even biopsies, while also driving up healthcare costs. You can read more about the impact of bone scan utilization in prostate cancer care.
Ultimately, a bone scan gives a wide-angle, but somewhat blurry, picture of what's happening in the skeleton. Its findings have to be interpreted carefully, always within the context of your PSA levels, Gleason score, and overall health. This challenge is also exactly why newer, more precise imaging tests like the PSMA PET scan are becoming so important in modern prostate cancer care.
Comparing Bone Scans to Modern Imaging Tests
For decades, the bone scan was the go-to tool for oncologists looking for prostate cancer that had spread. It's a reliable workhorse, but medical imaging has taken some massive leaps forward. Today, we have several advanced tools that give us a much clearer and more specific picture of what’s happening inside your body.
Let's break down how the classic bone scan stacks up against these newer options. It helps to think of it this way: a bone scan is like a smoke detector. It's great at telling you there’s some kind of fire somewhere in the house, but it can’t tell you if it’s a tiny kitchen flare-up or a major problem. Newer scans are like thermal imaging cameras—they show you exactly where the heat is coming from and how big the source is.
The Rise of PSMA PET Scans
The most important new player on the field is the PSMA PET scan. This has been a genuine game-changer.
PSMA stands for Prostate-Specific Membrane Antigen, a protein that shows up in huge quantities on the surface of prostate cancer cells. The scan uses a special tracer designed to hunt down and attach to this specific protein. When it does, the cancer cells light up like a beacon, no matter where they are—in bones, lymph nodes, or other organs.
This targeted approach makes the PSMA PET scan incredibly sensitive and specific. It can spot tiny clusters of cancer cells that a traditional bone scan would completely miss. Because of this precision, it’s quickly becoming the new gold standard for staging men with prostate cancer.
The Roles of CT and MRI Scans
Computed Tomography (CT scans) and Magnetic Resonance Imaging (MRI scans) also have critical, distinct roles in painting the full picture. They just work very differently.
CT Scans: These use X-rays to build a detailed, 3D-like map of your body's interior. CTs are fantastic for checking for cancer spread to soft tissues and lymph nodes, but they aren't as good as a bone scan at picking up early signs of trouble in the bones. To see how these scans are applied elsewhere, you can learn more about how a CT scan is used in diagnosing other cancers in another one of our guides.
MRI Scans: Instead of X-rays, MRIs use powerful magnets and radio waves. This gives them an unmatched ability to create incredibly detailed images of soft tissues. We often use an MRI to get a close-up look at the prostate gland itself or to carefully evaluate the spine for any signs of cancer.
This is where you can see the core difference between a bone scan's broad search (sensitivity) and its main weakness—not always knowing what it found (specificity).
As the diagram shows, a bone scan is a powerful search tool, but its findings often require another step to figure out exactly what’s going on.
Key Insight: A bone scan spots the bone's reaction to a potential problem, while a PSMA PET scan finds the prostate cancer cells themselves. That fundamental difference is why a PSMA PET gives us a much clearer, more direct map of the cancer.
Comparing Imaging for Prostate Cancer Metastases
To make it easier to see the differences at a glance, we've put together a simple comparison. Each test has its strengths, and we often use them in combination to get the most complete information possible.
Ultimately, choosing the right imaging test isn't a one-size-fits-all decision. Your oncologist will carefully consider your unique case—including your PSA level, Gleason score, and overall health—to select the right tools to build the most accurate and effective treatment plan for you.
What Happens After Your Scan Results
Getting your bone scan results is a big moment, but it's important to remember that the report itself is just one piece of the puzzle. The most critical part happens next: sitting down with your oncologist to go over what those images really mean for you and your treatment journey.

A bone scan report is never looked at in a vacuum. Your doctor will interpret the findings alongside your entire medical history—your past PSA levels, the Gleason score from your biopsy, and any symptoms you've been feeling. Only by pulling all these threads together can we get an accurate picture and map out the best path forward.
Crafting a Treatment Plan That’s Right for You
Here at Hirschfeld Oncology, we take all of that information to build a treatment plan tailored specifically to you. We believe in turning complex medical data into a clear, straightforward strategy that you can understand and feel confident about. The results of a bone scan for prostate cancer are a key factor in deciding which therapies will be most effective.
Depending on what we learn from the scan and your other tests, the next steps might involve:
- Hormone Therapy: This is a common and effective starting point if the cancer has reached the bones, as it works throughout the body to slow down cancer cell growth.
- Targeted Radiation: If you only have a few spots of cancer in the bones (what we call oligometastatic disease), we can use highly focused radiation to treat those specific areas.
- Systemic Treatments: For more widespread bone metastases, your options might expand to include advanced therapies that treat the cancer systemically.
- Continued Monitoring: If your scan is clear and other risk factors are low, the best course of action may simply be to continue with active surveillance.
We believe every decision should be a conversation. Our goal is to make sure you understand not just what we're recommending, but why we're recommending it. We're in this together.
Ultimately, your scan results are a crucial guidepost. They help us understand the extent of the cancer, which then clarifies the most effective way to manage it. This whole process is about ensuring your treatment plan is precisely aligned with your diagnosis and your own personal goals.
Your Top Questions About Bone Scans
Even with a good overview, it's completely normal to have a few more questions pop into your head. Let's walk through some of the most common things patients ask us about the bone scan process.
How Long Should I Plan to Be There?
You’ll want to set aside a good chunk of your day. The entire process, from check-in to heading home, usually takes about 3 to 5 hours.
This time includes:
- The quick injection of the tracer.
- A waiting period of 2 to 4 hours while the tracer travels through your bloodstream and settles into your bones.
- The actual scan, which itself is about 30 to 60 minutes.
Will the Scan Hurt?
The scan itself is totally painless. The only part you'll feel is the tiny prick from the IV needle when the tracer is injected—it’s just like getting a blood test.
Some people find it a little uncomfortable to lie still on the scanner table for that long, but there's no pain involved with the imaging.
What About Radiation? Am I Being Exposed to a Lot?
It’s a valid concern, but the amount of radiation you're exposed to is very small and considered quite safe. Think of it as being on par with a standard X-ray.
Your body naturally flushes the tracer out through your urine over the next day or two. Drinking plenty of water after your scan can help speed that along.
It's helpful to remember that a bone scan is strictly a diagnostic tool, not a form of treatment. Its whole purpose is to gather information safely so your care team can map out the most effective path forward for you.
For more answers to common questions, our team has put together a library of helpful resources for cancer patients and their families.
At Hirschfeld Oncology, we know that clear, straightforward information is the first step toward feeling empowered in your care. If you have more questions about your imaging plan or want to discuss what your results mean for your treatment, please reach out to us to schedule a consultation.





.png)


.png)
.png)




