Setting the Stage: Patient‑Centric Oncology and Lifestyle Coaching
Lifestyle coaching is a process that guides cancer patients and caregivers through nutrition, physical activity, stress management, sleep hygiene and health‑literacy improvement, using motivational interviewing, goal‑setting and resource navigation. It dovetails with care models such as the IOM’s eight dimensions and NCCN supportive‑care domains, delivering emotional support, communication, shared decision‑making and multidisciplinary teamwork. Systematic reviews and meta‑analyses demonstrate that coaching reduces anxiety and depression, improves physical activity, diet and weight control, and lowers fatigue, thereby decreasing recurrence risk and mortality. Economic analyses in chronic disease and oncology pilot studies further show reduced utilization, cost savings and patient satisfaction, supporting integration.
Integrating Lifestyle Coaching into Patient‑Centric Oncology

Evidence that health coaching improves mental health and survival
Systematic reviews show health coaching reduces anxiety and depression—risk factors that increase cancer recurrence by 24 % and mortality by up to 76 % (Wang et al., 2020). Meta‑analyses of >282,000 breast‑cancer patients link improved mental health to lower all‑cause mortality, and higher fitness levels cut mortality by up to 46 % (Bettariga et al., 2023).
Guidelines from ACS, NCCN, ASCO, ESMO
All major oncology societies endorse lifestyle interventions (nutrition, activity, stress management) across the cancer continuum, recommending their integration into survivorship care plans.
Reimbursement pathways (AMA CPT codes)
The AMA’s Category III CPT codes (99401‑99404, 99406‑99407) enable billing for Certified Health & Wellness Coaches, legitimizing coaching in U.S. oncology practice.
Five pillars of health coaching
Nutrition, movement, sleep, stress management, and social connection.
Five Ps of coaching
Purpose, Partnership, Planning, Patterns, People.
Salary expectations for cancer coaches
Average U.S. salary ≈ $85,000/yr; entry‑level ≈ $68,000, experienced up to $120,000‑$130,000 depending on location and expertise.
Lifestyle medicine and cancer
Lifestyle medicine—optimal nutrition, regular activity, restorative sleep, stress management, social connectedness, and avoidance of risky substances—addresses modifiable factors responsible for up to 45 % of cancer deaths, improving recurrence risk and overall survival.
What is the role of a lifestyle coach?
A lifestyle coach mentors patients to set SMART goals, overcome barriers, and sustain behavior change across nutrition, movement, stress, and sleep, enhancing empowerment and quality of life.
What are the 5 pillars of health coaching?
Nutrition, Movement, Sleep, Stress Management, Social Connection.
What is lifestyle oncology?
Lifestyle oncology applies lifestyle‑medicine principles to cancer care, integrating diet, exercise, sleep, and mind‑body practices with standard therapies to boost tolerance, reduce recurrence, and improve survivorship.
What are the 5 Ps of coaching?
Purpose, Partnership, Planning, Patterns, People.
Cancer Coach salary
Typical range $68,000–$130,000 /yr, averaging $85,000, reflecting demand for specialized oncology support.
Financial Navigation and Support Services for Cancer Patients

Rental assistance for cancer patients
Patients can call 2‑1‑1 for a statewide directory of emergency housing aid and rent‑relief services. The Cancer Financial Assistance Coalition and Chemo Divas list non‑medical grants that include rent support. Community Action Partnerships administer LIHEAP and Weatherization grants covering housing costs, while Family Reach’s Financial Resource Center offers one‑on‑one counseling and a searchable database of regional rent‑assistance programs. Hope Lodge and Extended Stay America provide free or reduced‑rate lodging for treatment‑related travel, offsetting overall housing expenses.
Emergency financial assistance for cancer patients
Contact the oncology social‑work team for rapid assessment and connection to emergency funds, short‑term housing, transportation vouchers, and prescription‑cost assistance. Federal programs such as Medicaid, Medicare, SSI, and SSDI can provide immediate income support. Non‑profits like CancerCare, the American Cancer Society, and the Patient Advocate Foundation offer emergency co‑pay relief, lodging grants, and food assistance searchable by diagnosis and zip code.
Free gas cards for cancer patients
Organizations such as My Cancer Resources, Mercy Medical Angels, and Tenaciously Teal issue gas‑card programs for patients meeting distance (≥50 mi one‑way) and income criteria. Applications require a physician verification letter and, sometimes, income documentation; virtual cards are delivered within days.
Free government grants for cancer patients
While no stand‑alone cash grants exist, federal and state programs act like grants: Medicaid/Medicare coverage, SSDI/SSI income, SNAP food assistance, and state‑run transportation vouchers or housing subsidies. Patients should contact their local 211 service or the Social Security Administration to determine eligibility and start the application process.
Accessing Coaching and Support Resources
 Finding a cancer coach begins with your treatment team. Hirschfeld Oncology’s multidisciplinary staff includes patient‑advocates who provide personalized coaching, navigation, and emotional support throughout the pancreatic‑cancer journey. Local options such as Fort Worth’s Center for Cancer & Blood Disorders, telehealth‑enabled therapists (e.g., Melissa Lewis, LPC), and Holistic Health & Psychiatry in Arlington also act as coaches. Ask your oncologist for nurse‑navigator or survivorship referrals, and consider nearby peer groups like the monthly meeting at 800 W Magnolia Ave., Fort Worth for shared guidance.
Cancer support groups cover a spectrum of diagnoses—Breast, Lung, Pancreatic, Gynecologic, Young Adult, LGBTQ+, and Metastatic Breast Cancer—as well as caregiver and bereavement groups. The American Cancer Society’s ACS CARES™ program connects patients and caregivers with one‑on‑one support, while its Survivors Network offers an online community for peer interaction. In‑person and video‑conferenced groups are available in New York, New Jersey, and other regions, addressing survivorship, older adults, journal writing, and metastatic disease topics.
Free services for cancer patients include the ACS 24/7 helpline, ACS CARES, and non‑profits like Cancer Care® and the Patient Advocate Foundation, which provide co‑pay assistance, drug‑cost programs, and a searchable aid database. Charities also supply complimentary wigs, scarves, medical equipment, and travel‑housing vouchers. Mobile apps and online toolkits help patients track appointments, medication, and survivorship plans at no cost.
A holistic cancer coach delivers whole‑person support that blends emotional guidance, nutrition, lifestyle strategies, and mindset tools across the cancer continuum. Working alongside oncologists, the coach translates medical plans into daily habits that boost resilience, reduce side effects, and enhance quality of life. This approach aligns with Hirschfeld Oncology’s mission to pair cutting‑edge therapies with innovative, patient‑centered care, turning diagnosis into an opportunity for growth and hope.
Group Health Coaching Models and Outcomes
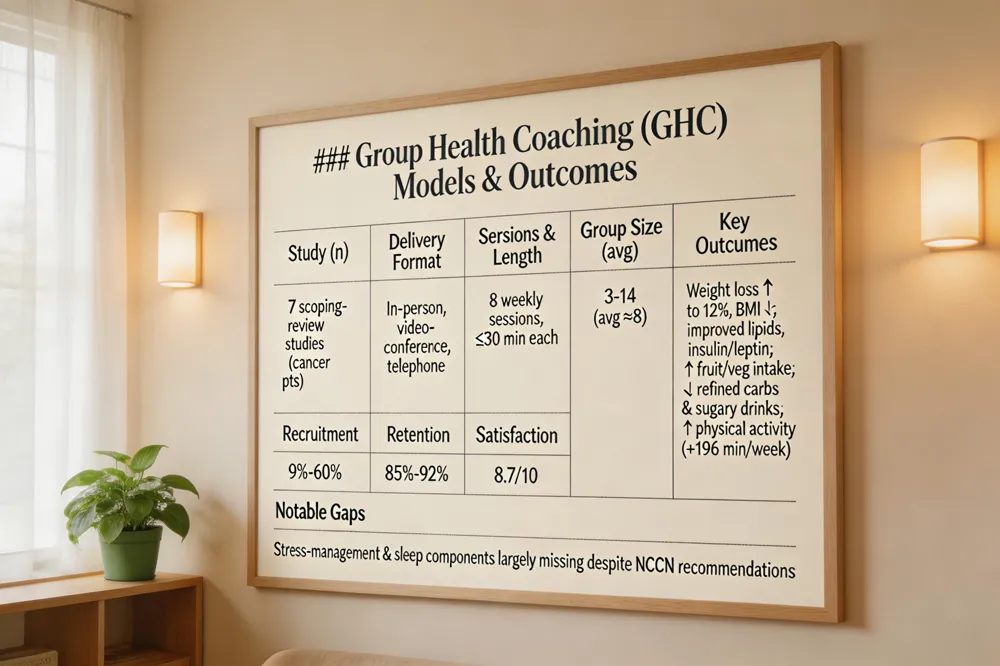 A recent scoping review identified seven group health coaching (GHC) studies that met inclusion criteria for cancer populations. Participants were mainly female, mean age 51‑69, various cancer types. The most common topics were physical activity, diet, weight loss, often combined in a single program.
Delivery formats varied: in‑person, video conferencing, telephone. Programs typically ran for eight weekly sessions most common, each lasting ≤30 minutes, with group sizes of 3‑14 participants, average about eight per group.
Feasibility and acceptability were high—recruitment 9%‑60%, retention 85%‑92%, satisfaction 8.7/10. Outcome highlights included up to 12% weight loss, BMI reduction, improved lipids, lower insulin/leptin, more fruits/vegetables, less refined carbs and sugary drinks, lower calories, and one study +196 min/week moderate‑vigorous activity. Quality‑of‑life improvements were noted in joint pain, depressive symptoms, body image; some decline in functional wellbeing/fatigue during treatment.
Despite these benefits, the review highlighted a notable gap: few GHC programs addressed stress‑management or sleep despite NCCN recommendations. Future research should standardize coach certification, expand follow‑up beyond six months, and incorporate stress‑reduction and sleep‑management.
Professional Training and Certification for Cancer Coaches
 Cancer Coaching Institute (CWI) is an internationally recognized leader in evidence‑based cancer coaching education. It offers a self‑paced Integrative Cancer Coaching Certification, live online and in‑person intensive programs, and specialty concentrations that are approved by NBHWC, UKIHCA, HCANZA, and the International Coaching Federation. Programs equip health professionals with trauma‑informed communication, goal‑setting, and behavior‑change skills, preparing them for roles that support patients through diagnosis, treatment, and survivorship. Certification pathways range from a 12‑week online Foundations course ($895) to a 5‑day intensive in‑person program ($3,195), all including tools, templates, and a year of community mentorship. Graduates can pursue the NBC‑HWC credential, expanding career prospects in integrative oncology support. Fees for coaching services vary: health coaches typically charge $30–$200 per hour (average $100), while life coaches command $75–$250 per hour (average $90). Many offer package discounts to lower the effective hourly rate. Certification opens rewarding career opportunities, with salaries reflecting the growing demand for certified cancer health coaches in multidisciplinary oncology teams.
Patient‑Centered Communication and Quality of Care
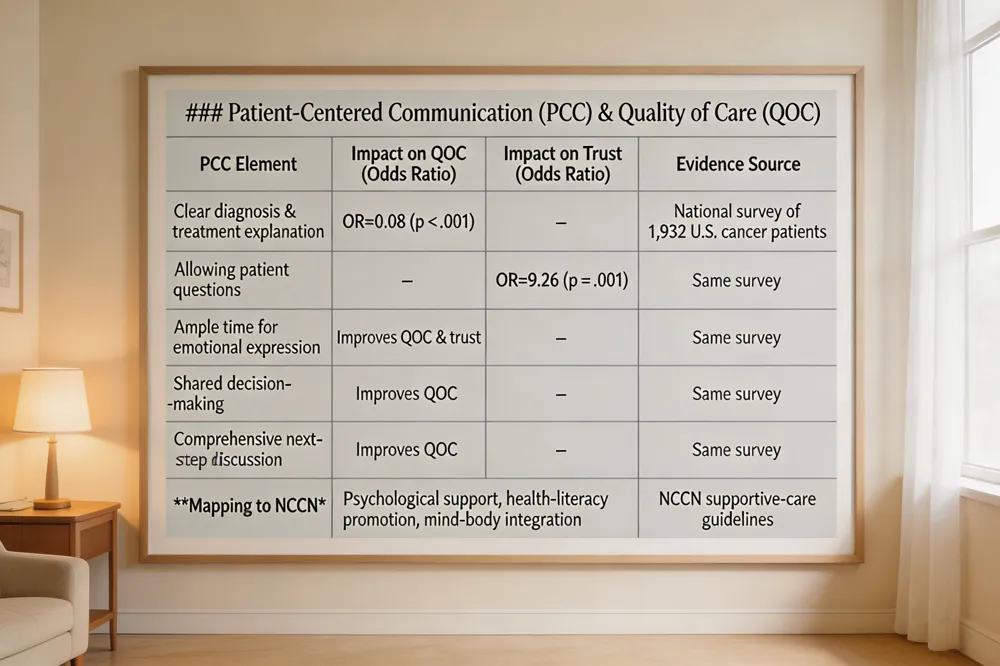 Patient‑centered communication (PCC) markedly improves cancer patients’ trust in clinicians and their perceived quality of care (QOC). In a national survey of 1,932 U.S. cancer patients, PCC was associated with higher QOC (OR = 0.08, p < .001) and a nine‑fold increase in trust when patients could ask questions (OR = 9.26, p = .001). The communication elements that drive these outcomes include clear explanations of diagnosis and treatment, ample time for patients to express feelings, thorough discussion of next steps, and shared decision‑making. Each component independently predicts better QOC and higher trust. These PCC domains map directly onto the NCCN supportive‑care guidelines, which emphasize psychological support, effective communication, empowerment, needs assessment, mind‑body integration, self‑help resources, and health‑literacy promotion. By embedding PCC into multidisciplinary oncology teams, programs can enhance patient engagement, reduce anxiety and depression, and ultimately improve adherence to lifestyle interventions—further supporting the NCCN goal of comprehensive, patient‑centric cancer care.
A Call to Action: Making Lifestyle Coaching Standard in Oncology
Health coaching reduces anxiety, depression, improves physical activity, nutrition, sleep, and weight control, which are linked to lower recurrence and mortality (e.g., 24% higher recurrence risk with depression). Integrated coaching boosts patient engagement, self‑efficacy, and adherence to evidence‑based lifestyle changes, decreasing symptom burden and health‑care utilization. Hirschfeld Oncology can embed certified coaches within its multidisciplinary team, offering virtual or group sessions that align with NCCN supportive‑care domains and CPT reimbursement pathways. Patients should ask for a coaching referral; providers should train staff, establish referral workflows, and track outcomes using PROMs to normalize coaching as standard cancer care.





.png)


.png)
.png)




