A biliary stent is a tiny, hollow tube that a specialist places inside a blocked bile duct. It’s a bit like a miniature scaffold or a spring used to prop open a clogged pipe, ensuring bile can flow freely from your liver to your intestine again. This procedure is a cornerstone of care for many patients, especially those whose bile ducts are blocked by conditions like pancreatic or bile duct cancer.
To give you a quick overview, here’s a simple breakdown of what this procedure is all about.
Quick Guide to Biliary Stent Placement
| Concept | Simple Explanation |
|---|---|
| What It Is | A small, expandable tube inserted into a bile duct. |
| The Goal | To hold a blocked bile duct open and restore normal bile flow. |
| Main Benefit | Rapid relief from symptoms like jaundice, itching, and nausea. |
| Role in Cancer Care | Often makes it possible to start or continue treatments like chemotherapy. |
This simple intervention can make a world of difference in your daily life and overall treatment plan.
Restoring Flow, Restoring Quality of Life

When a tumor—often from pancreatic cancer or cholangiocarcinoma—presses on a bile duct, it acts like a dam. The resulting backup of bile triggers a cascade of debilitating symptoms that can severely diminish your well-being. A biliary stent placement is designed to directly address that blockage, often bringing immediate and profound relief.
Most patients feel the benefits within days, and the change can be truly transformative. Key improvements we see include:
- Relief from Jaundice: As bile drains properly, the yellowing of the skin and eyes begins to fade.
- An End to Persistent Itching: That maddening, constant itch (called pruritus), which is caused by bile salts accumulating in the skin, finally subsides.
- Less Nausea and Discomfort: With bile aiding digestion as it should, nausea and abdominal pain often ease up.
- A Return to Normal: You’ll notice your urine color lightening and stool color returning to normal—clear signs your digestive system is getting back on track.
A Critical Bridge to Further Cancer Treatment
Beyond just managing symptoms, biliary stenting plays a crucial strategic role. It often serves as a necessary bridge, clearing the way for you to begin or resume essential cancer treatments. Many chemotherapy and immunotherapy drugs simply cannot be administered safely unless your liver is functioning properly.
By opening the bile duct and allowing the liver to recover, a biliary stent often gives patients the green light to move forward with their life-extending therapies. It turns a major roadblock into a manageable hurdle in the larger treatment journey.
The procedure's value is clear from its widespread use in modern oncology. The global market for these devices was valued at around USD 455.3 million in 2026, with steady growth projected. This reflects the increasing need for effective, minimally invasive options for patients facing malignant biliary obstructions. At practices like Hirschfeld Oncology, which specializes in complex cancers, this procedure is fundamental to both palliative care and enabling further treatment.
Successfully clearing a blockage is often one of the first big wins in fighting cancers that affect the biliary system. To learn more about the disease itself, you can explore our comprehensive guide on bile duct cancer treatment and its challenges. This procedure is more than a quick fix; it’s a strategic step that opens the door to better health and renewed hope.
Understanding Your Biliary Stent Options
When you’re dealing with a biliary obstruction, one of the most important conversations you'll have with your care team is about choosing the right stent. It’s a decision that has to balance your immediate need for relief with your longer-term treatment plan.
Think of it this way: if a tunnel is starting to collapse, you have a couple of options. You could install temporary wooden beams that are easy to put in and adjust, knowing you’ll have to replace them. Or, you could put in a permanent steel arch designed to hold everything open for the long haul. The right choice depends entirely on the situation inside that tunnel.
It’s much the same with biliary stents. We primarily work with two different kinds—plastic and metal—and knowing the difference will help you and your doctors decide on the best path forward.
Plastic Stents: The Temporary, Flexible Solution
Plastic biliary stents are often our go-to for situations that are temporary or uncertain. Made from a flexible material like polyethylene, they are inexpensive and, critically, they're designed to be easily removed and replaced.
We typically turn to plastic stents in a few key scenarios:
- When a diagnosis isn't clear: If we know there's a blockage but need to do more tests to understand why, a plastic stent can buy us time while keeping you comfortable.
- For benign (non-cancerous) strictures: Sometimes a duct narrows for reasons other than cancer. We can use a series of progressively larger plastic stents to gently stretch the duct open over time.
- As a bridge to surgery: If you're a candidate for surgery but are too jaundiced to proceed safely, a plastic stent can resolve the jaundice and get you ready for the operating room.
The main trade-off with plastic stents is their durability. Because they have a narrower opening, they are more likely to get clogged with sludge. This means they usually need to be replaced every three to six months to prevent another blockage or an infection.
Metal Stents: The Durable, Long-Lasting Option
Now, for blockages caused by a tumor that likely can't be removed with surgery, we often lean on self-expanding metal stents (SEMS). These are the "steel arches" in our analogy. They are delivered through an endoscope in a tightly compressed form and, once in place, expand on their own with a steady outward force.
Imagine a tiny, pre-loaded spring. When we release it inside the bile duct, it pushes the tumor back and props the duct open, creating a much wider and more resilient channel for bile to flow. This design provides much longer-lasting relief than a plastic stent.
The biggest advantage of metal stents is how long they last. Their wide internal diameter dramatically lowers the risk of clogging, and they can often stay open and functional for a year or even longer. For patients needing palliative relief, this is a huge benefit because it means fewer repeat procedures and more time focused on quality of life.
Here in the United States, we have excellent access to these advanced technologies. In fact, North America accounts for about 38% of the global biliary stent market, partly because we have so many specialized centers performing ERCP for complex cancers. This leadership ensures that skilled specialists can offer the latest innovations in stent technology. You can read more about these market insights and what they mean for patient care.
To help you see the differences at a glance, here’s a breakdown of how plastic and metal stents compare.
Plastic vs Metal Biliary Stents: A Comparison
This table highlights the key differences between the two main types of stents, which should help clarify the discussion you'll have with your physician.
| Feature | Plastic Stents | Metal Stents (SEMS) |
|---|---|---|
| Material | Polyethylene or Teflon | Medical-grade metal alloy (e.g., Nitinol) |
| Primary Use Case | Temporary drainage, benign strictures, pre-surgical use | Long-term palliative relief for malignant obstructions |
| Durability | Lower; patency of 3-6 months | Higher; patency often exceeds 12 months |
| Internal Diameter | Smaller, more prone to clogging | Larger, less prone to clogging |
| Removability | Easily removable and replaceable | Typically permanent (though some covered types can be removed) |
| Cost | Less expensive | More expensive |
| Key Advantage | Flexible, removable, and low initial cost | Long-lasting relief, reducing the need for repeat procedures |
| Main Drawback | Short lifespan requires frequent replacements | Higher initial cost and usually a permanent implant |
Ultimately, the choice isn't just about the stent itself, but about how it fits into your overall health picture and treatment goals.
A Deeper Dive: Covered vs. Uncovered Metal Stents
To add another layer of nuance, metal stents also come in a few different styles: uncovered, partially covered, and fully covered. This choice comes down to a careful trade-off between keeping the stent in place and preventing the tumor from growing through it.
An uncovered stent is made of a bare metal mesh. This design allows the stent to embed itself firmly into the duct wall, making it very unlikely to move or migrate. The downside is that tumor tissue can eventually grow through the openings in the mesh, causing a new blockage.
A fully covered stent has a thin silicone or polymer coating that acts as a barrier, preventing the tumor from growing through it. This keeps the channel open longer, but the smooth surface makes it more likely to slip out of position.
Finally, partially covered stents are a hybrid, with bare metal ends to grip the duct wall and a covered mid-section to block tumor growth. They try to offer a balance of stability and durability—the best of both worlds.
Your specialist will weigh all these factors—the location of your tumor, its specific characteristics, and your overall health—to recommend the ideal type of stent. This is a crucial part of personalizing your biliary stent placement to ensure the best possible outcome for you.
What to Expect: From Procedure to Recovery
It’s completely normal to feel some apprehension before a medical procedure. Knowing exactly what to expect before, during, and after your biliary stent placement can go a long way in calming those nerves and helping you feel more in control. Let's walk through the entire process together, from the moment you arrive to your recovery at home.
Before the procedure, your care team will give you specific instructions. The most important one is to avoid eating or drinking for at least six to eight hours beforehand. This ensures your stomach is empty, which is crucial for a safe procedure. If you’re coming from abroad or your medical files are in another language, using professional medical records translation services can be incredibly helpful to make sure your entire care team has a complete picture of your health history.
The Day of Your Biliary Stent Procedure
When you arrive, we'll get you settled in and place a small IV in your arm. This is for fluids and medication to keep you comfortable. For most biliary stent procedures, we use a form of sedation often called "twilight sleep."
This isn't general anesthesia. You'll be very relaxed and sleepy, breathing on your own, and you won't feel any pain or remember the procedure afterward. While you're resting comfortably, the specialist—an interventional gastroenterologist or radiologist—will use sophisticated imaging to guide the stent into its exact position. The whole thing is usually over in about 30 to 60 minutes.
Deciding which stent is right for you depends on your specific situation—whether the blockage is temporary or if you need a more permanent solution.
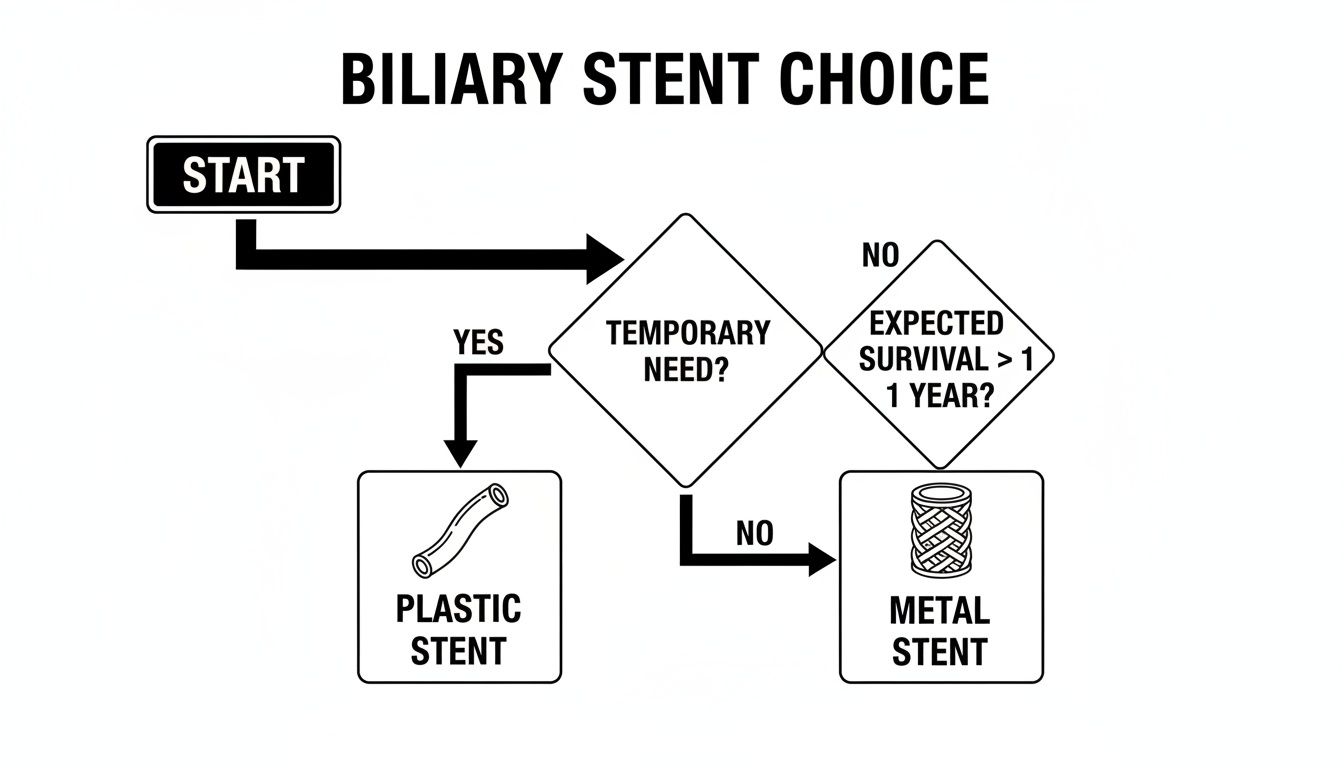
This flowchart gives you a glimpse into how your doctor might choose between a plastic stent for a short-term fix or a more durable metal stent for longer-lasting relief.
Your Immediate Recovery and Hospital Stay
After the stent is in place, you’ll spend some time in a recovery area. Our nursing staff will keep a close eye on you as the sedation starts to wear off. It's very common to feel a bit groggy, bloated, or experience some mild cramping in your abdomen. Don't worry, this is perfectly normal and typically fades within a few hours.
One known risk after an ERCP (the endoscopic method for placing a stent) is a condition called post-ERCP pancreatitis (PEP). While usually mild, it’s something we watch for very carefully, as it can occur in a notable percentage of cases. This is why that initial monitoring period is so important.
Most patients go home the same day. However, if your procedure was more involved or if we want to monitor you more closely for potential issues like pancreatitis, you might stay overnight. We’ll make sure you're feeling stable and comfortable before sending you home.
At Home: What to Do and What to Look For
Once you're back home, the focus shifts to a gentle recovery. For the first few days, it’s all about taking it easy and letting your body heal.
- Your Diet: We'll have you start with clear liquids. From there, you can slowly add soft, low-fat foods back into your diet over the next day or two. This gradual approach is gentler on your digestive system as it adjusts to the new stent.
- Your Activity: Avoid any heavy lifting or intense exercise for a few days. Gentle activity, like short walks, is great for promoting circulation and recovery.
- Watching for Good Signs: Keep an eye on how you're feeling. The best part is seeing the positive signs that the stent is doing its job, which often appear within a few days.
You should notice the whites of your eyes and your skin becoming less yellow (if you had jaundice). Any itching you experienced should start to fade, and the color of your urine and stools should begin to normalize. These are all powerful signals that bile is finally flowing freely again, which is a huge step toward feeling better and moving forward with your treatment plan.
Living with a Biliary Stent Long Term

Once your biliary stent is in place, you'll begin to settle into a new routine. With the immediate symptoms of the blockage relieved, you can turn your focus back to your main cancer treatment and simply living your life. Getting comfortable with this new reality means knowing what to expect and how to be an active partner in your own care.
For many patients, especially those with a blockage related to their cancer, this is a long-term adjustment. It’s a lot like other forms of ongoing health management, which often involves Mastering Chronic Condition Management at Home by staying vigilant and keeping an open line of communication with your medical team. The goal is straightforward: keep the stent doing its job for as long as possible.
Watching for Signs of Stent Blockage
The most common issue we see with biliary stents over time is occlusion, which is just a medical term for a blockage. Think of the stent like a pipe in your house—over time, sediment and debris can build up and cause a clog. In a stent, this buildup comes from bile sludge, or in some cases, tumor tissue can grow through the mesh of an uncovered metal stent.
The good news is that the warning signs of a blockage are usually the same symptoms that brought you to the doctor in the first place. You are the first line of defense, so learning to recognize these signs is incredibly important.
- Return of Jaundice: You notice a yellow tinge returning to your skin or the whites of your eyes.
- Changes in Waste: Your urine becomes dark again, or your stools turn pale or clay-colored.
- Intense Itching (Pruritus): That frustrating, whole-body itch you had before the stent suddenly comes back.
- New or Worsening Pain: You feel a new or familiar ache in the upper right part of your abdomen.
- Signs of Infection: You develop a fever, start having chills, or just feel generally unwell. This could point to cholangitis, a serious infection of the bile duct.
If you spot any of these symptoms, don't wait. Call your oncology team right away. A blocked stent needs prompt medical attention, but it's a known issue that we are well-prepared to handle.
Understanding Stent Migration and Dislodgment
Another possibility, though less common, is stent migration. This is when the stent shifts out of its intended position. It's more of a risk with fully covered metal stents because their smooth coating prevents them from embedding into the duct wall. In contrast, an uncovered metal stent’s mesh-like structure anchors it more securely, making it far less likely to move.
We know that complications from biliary stent placement can occur in about 8% to 10% of cases. Stent migration specifically happens in roughly 5% to 10% of patients. The risk of a stent moving, or dislodgment, can be higher for certain types; fully covered metal stents may have rates around 20%, while plastic or partially covered stents are much lower at approximately 5%.
The key takeaway is this: while complications can happen, they are well-understood and treatable. Your medical team has a clear plan to address issues like a blockage or a moved stent, usually involving a straightforward endoscopic procedure to adjust, clean, or replace it.
Longevity and Replacement Schedules
How long your stent will last is one of the biggest factors in your long-term plan, and it depends entirely on the type you have.
- Plastic Stents: These are really meant to be temporary. Because they have a smaller diameter, they are more likely to clog. You can expect to have a plastic stent replaced every 3 to 6 months.
- Metal Stents (SEMS): These are the workhorses, built for durability. Their wider opening keeps them functioning much longer, often for a year or more, before needing any intervention.
Your specialist will set up a follow-up schedule based on your specific stent. It’s crucial to keep these appointments, even if you’re feeling great. Proactive check-ins allow us to catch a potential problem before it even starts causing symptoms. For more advice on this, take a look at our guide on managing gastrointestinal cancer symptoms during treatment.
Partnering with Hirschfeld Oncology for Your Care
Dealing with a cancer diagnosis can feel like trying to manage a dozen different things at once. When a procedure like a biliary stent is needed, it adds another layer of complexity. At Hirschfeld Oncology, we know that the best care isn't just about the right treatments—it's about having a dedicated team that works together, with your well-being as the only goal.
Led by Dr. Azriel Hirschfeld, our team sees you as a person, not just a diagnosis. We believe in building a truly coordinated care plan that feels supportive and clear.
A cancer journey is much more than just a series of treatments like chemotherapy or immunotherapy. It’s about managing your symptoms, keeping you strong, and making sure your body is in the best possible shape to fight the cancer. A biliary stent placement is a perfect example of this. We work hand-in-hand with New York City’s most respected interventional gastroenterologists and radiologists to make sure this critical procedure fits perfectly into your overall care plan.
Your Personalized Care Coordination
This close collaboration means your care is never split between different offices or competing priorities. We take on the job of coordinating everything so you can put your energy where it belongs: on your health.
Think of Dr. Hirschfeld as the central point person for your entire care team. While a highly skilled specialist is the one performing the stent procedure, Dr. Hirschfeld's role is to ensure the timing is right and the procedure's goals align with your upcoming cancer therapy. He makes sure everyone is on the same page. This unified approach is especially critical for anyone dealing with advanced cancers like cholangiocarcinoma or pancreatic cancer, where every decision has a major impact.
Our commitment is to give you a clear, supportive path forward. We coordinate with specialists to ensure your biliary stent procedure not only relieves symptoms but also strategically paves the way for your primary cancer treatment, helping you regain control and hope.
Preparing for Your Consultation
A good conversation is the first step toward building a strong partnership with your doctor. Whether you're meeting at our Brooklyn infusion center or with one of our trusted partners, coming prepared can help you feel more in control.
We always encourage patients to bring a list of questions to their appointments. It’s the best way to make sure all your concerns are heard and that you leave with a solid understanding of the road ahead.
Here are a few essential questions to get you started:
- Why is a biliary stent the right choice for me right now?
- What kind of stent are you recommending, and why is it the best option for my specific situation?
- What are the next steps in my cancer treatment after the stent is in place?
- Who do I call if I think there’s a problem with the stent, like a blockage?
- How will this procedure affect my quality of life, both now and in the long run?
For those looking into every possible option, it’s also a good idea to ask how this procedure fits with emerging treatments. You can learn more about how we connect patients with new research by exploring our guide to bile duct cancer clinical trials.
If you or someone you love is navigating a complex cancer diagnosis in the New York City area, we invite you to schedule a consultation with Hirschfeld Oncology. Let us show you how our patient-first approach can make all the difference.
Frequently Asked Questions About Biliary Stents
Learning you need a biliary stent can bring up a lot of questions for both you and your family. We get it. Let’s walk through some of the most common concerns we hear, answering them simply and directly so you know exactly what to expect.
How Soon Will I Feel Better After a Biliary Stent Placement?
Most people are surprised by how quickly they start to feel relief. While everyone's body responds differently, many patients notice a big improvement in symptoms like severe itching (pruritus) and jaundice within just a few days to a week.
One of the most reassuring signs is seeing your urine and stool colors return to normal—that's a clear signal the stent is doing its job. Recovery from the biliary stent placement itself is usually fast, too, with most people getting back to light activities in a matter of days. For many, that rapid relief is the first truly positive turn in their treatment journey.
Will I Be Able to Feel the Stent Inside Me?
That’s a very common worry, but the answer is no, you won't be able to feel the stent at all. Your bile ducts don't have the kind of nerves that would register the stent's presence. Once the initial minor discomfort or bloating from the procedure fades, the stent will work silently in the background.
It's completely natural to feel anxious about having a device inside your body. You can rest easy knowing the stent is designed to do its job without you ever being aware it's there.
This allows you to put your focus where it belongs: on your recovery and overall health, not on the stent itself.
What Are the Warning Signs That My Stent Is Blocked?
Knowing what to look for is key to staying ahead of any issues. It's time to call your doctor right away if your original symptoms start to come back. Be on the lookout for:
- Jaundice (skin or eyes turning yellow again)
- A return to dark urine or pale, clay-colored stools
- Intense itching that doesn't go away
- New or worsening pain in your abdomen
Also, keep an eye out for signs of a possible infection, like a fever or chills. A blocked stent needs to be addressed quickly, but your medical team is prepared for this. The solution is usually straightforward—cleaning or replacing the stent. By noticing these changes early, you become the most important member of your own care team.
Can I Continue Chemotherapy After Getting a Stent?
Absolutely. In fact, getting your cancer therapy back on track is often one of the main reasons for placing a stent. By clearing the biliary blockage, the stent allows your liver function to improve, which is often a requirement for safely receiving treatments like chemotherapy or immunotherapy.
Your oncologist will keep a close eye on your liver function tests to find the best and safest time to restart your treatment, helping to keep your entire cancer care plan moving forward.
At Hirschfeld Oncology, we know that navigating a cancer diagnosis requires coordinated, compassionate care. You can learn more about our patient-centered approach and find other helpful resources on our blog at https://honcology.com/blog.





.png)


.png)
.png)




