Yes, a CT scan can detect cancer. In fact, it's one of the most important tools we have for creating a detailed, 3D picture of what’s happening inside your body, allowing our doctors to spot abnormalities like tumors.
But there’s a crucial distinction to make. While a CT scan is excellent at finding a suspicious mass and telling us its size, shape, and location, it can't tell us what that mass is made of on a cellular level. It provides the "where," but not the definitive "what."
The Role of CT Scans in Finding Cancer
Think of a CT scanner as a sophisticated mapping tool. It takes hundreds of X-ray images from various angles and then uses a powerful computer to stack them into cross-sectional "slices." This gives us an incredibly detailed view, revealing things like masses or swollen lymph nodes that would otherwise go unseen.
For an oncologist, this 3D map is the first step in answering some of the most critical questions:
- Is there a suspicious growth? A CT scan can often spot tumors just a few millimeters in size.
- Where is it? The scan pinpoints the mass’s exact location and its relationship to nearby organs and blood vessels.
- How big is it? Getting accurate measurements is essential for cancer staging and for planning the right course of treatment.
- Has the cancer spread? Scans help us see if a tumor has moved into adjacent lymph nodes or traveled to distant organs.
A CT scan gives us the anatomical blueprint—the "what" and "where" of a suspicious mass. The next steps, like a biopsy, provide the biological proof we need to confirm if it’s truly cancer.
To give you a clearer picture, here's a quick summary of what CT scans bring to the table in cancer detection.
CT Scans for Cancer Detection At a Glance
This table shows why the CT scan is such a trusted workhorse in oncology—it gives us a wealth of information quickly, guiding our next steps.
More Than Just a Cancer Detective
While we rely on CT scans heavily in oncology, their diagnostic power is much broader. In emergency rooms, they are the go-to tool for quickly evaluating injuries from accidents. They are also vital for diagnosing urgent conditions like a blood clot in the brain, showcasing just how versatile this technology is.
Ultimately, a CT scan is a pivotal part of the diagnostic puzzle, but it’s rarely the final piece. The findings from a scan are what guide specialists, like our team at Hirschfeld Oncology, to recommend the right follow-up tests. Depending on the results, that might mean an MRI, a PET scan, or a biopsy to get the complete picture. This methodical approach is the only way to ensure a precise diagnosis before we design your personalized treatment plan.
How a CT Scan Creates a Picture of Your Body
Before we dive into how a CT scan spots cancer, it’s helpful to get a feel for how the machine actually works. Think of it like this: if you wanted to inspect every single layer of a loaf of bread without slicing it open, how would you do it? A CT scanner essentially does that for the human body.
As you lie on a table that slides through a large, doughnut-shaped machine, a very narrow X-ray beam rotates around you. It’s not taking one or two pictures, but hundreds of them from every possible angle. Each image is a razor-thin digital ‘slice’ of your body. A powerful computer then stacks these individual slices together to build a detailed 3D model of your bones, organs, and soft tissues.
This gives your doctor a comprehensive, cross-sectional view of your internal anatomy—something a standard X-ray could never provide.
From Slices to a Diagnosis
An experienced radiologist or oncologist then meticulously reviews these digital images. They're looking for abnormalities with a highly trained eye, searching for the tell-tale signs that point toward a potential malignancy. It's about much more than just finding a "lump."
The analysis focuses on specific characteristics, including:
- Irregular Shapes: Benign cysts and growths are often smooth and round. Cancerous tumors, on the other hand, frequently have jagged, poorly defined borders that infiltrate the surrounding tissue.
- Abnormal Density: Radiologists analyze the density of the tissues shown on the scan. A tumor might appear as a spot that is denser (brighter) or less dense (darker) than the healthy organ tissue around it.
- Swollen Lymph Nodes: Enlarged lymph nodes can be a red flag that cancer is on the move. This is a critical piece of information for staging the disease and planning the right course of action.
The real power of a CT scan isn't just in finding a mass. It's in showing that mass in context—revealing its relationship to the rest of the body. Is it pressing on a vital organ? Is it tangled up with major blood vessels? Has it spread? This anatomical detail is absolutely crucial for planning treatment.
The Role of Contrast Dye
Sometimes, to make the picture even clearer, we need to add a highlighter. This is where contrast dye comes in. If your doctor orders a CT "with contrast," a special iodine-based dye will be introduced into your bloodstream, usually through an IV.
As this contrast agent circulates, it makes blood vessels and organs with a rich blood supply light up brightly on the scan. Many tumors build their own network of blood vessels to feed their growth, so the dye helps them stand out dramatically from nearby healthy tissue.
This technique is especially valuable for defining the precise edges of tumors in organs like the liver or pancreas, giving surgeons a clear map to work from. To better understand how different imaging tools are used, you can explore our detailed comparison of a CT scan vs an MRI scan.
Weighing the Benefits Against the Risks
Let's talk about the elephant in the room: radiation. It’s completely understandable to be concerned about the safety of a CT scan. After all, this powerful imaging tool works by using ionizing radiation, a type of energy that, over time and with repeated exposure, can carry a small risk of damaging cells.
This presents a genuine paradox. The very technology that gives us a clear window into the body to find cancer also has a tiny, statistical chance of causing it down the road. For any patient, though, the immediate benefit of a definitive diagnosis almost always outweighs the theoretical, long-term risk. A single scan can provide life-saving information, catching a tumor early when it’s most treatable.
Minimizing Radiation Exposure
At experienced cancer centers like Hirschfeld Oncology, managing this balance is a core part of our responsibility. We operate under a guiding principle known as ALARA, which stands for As Low As Reasonably Achievable. It’s not just a guideline; it’s a commitment to ensuring every scan is as safe as possible.
So, how do we put ALARA into practice?
- Tailored Dosing: We never use a one-size-fits-all approach. The scanner's radiation dose is carefully calibrated based on a patient’s size, weight, and the specific part of the body we need to see.
- Necessary Scans Only: A CT scan is only ordered when it is absolutely essential for diagnosing, planning treatment for, or monitoring a potential cancer. If there's a better way, we'll use it.
- Modern Equipment: Today’s CT scanners are marvels of engineering. They are far more sensitive than older models, allowing us to capture incredibly detailed images with significantly less radiation.
This process transforms hundreds of thin X-ray "slices" into a comprehensive 3D model that a radiologist can analyze for any signs of disease.
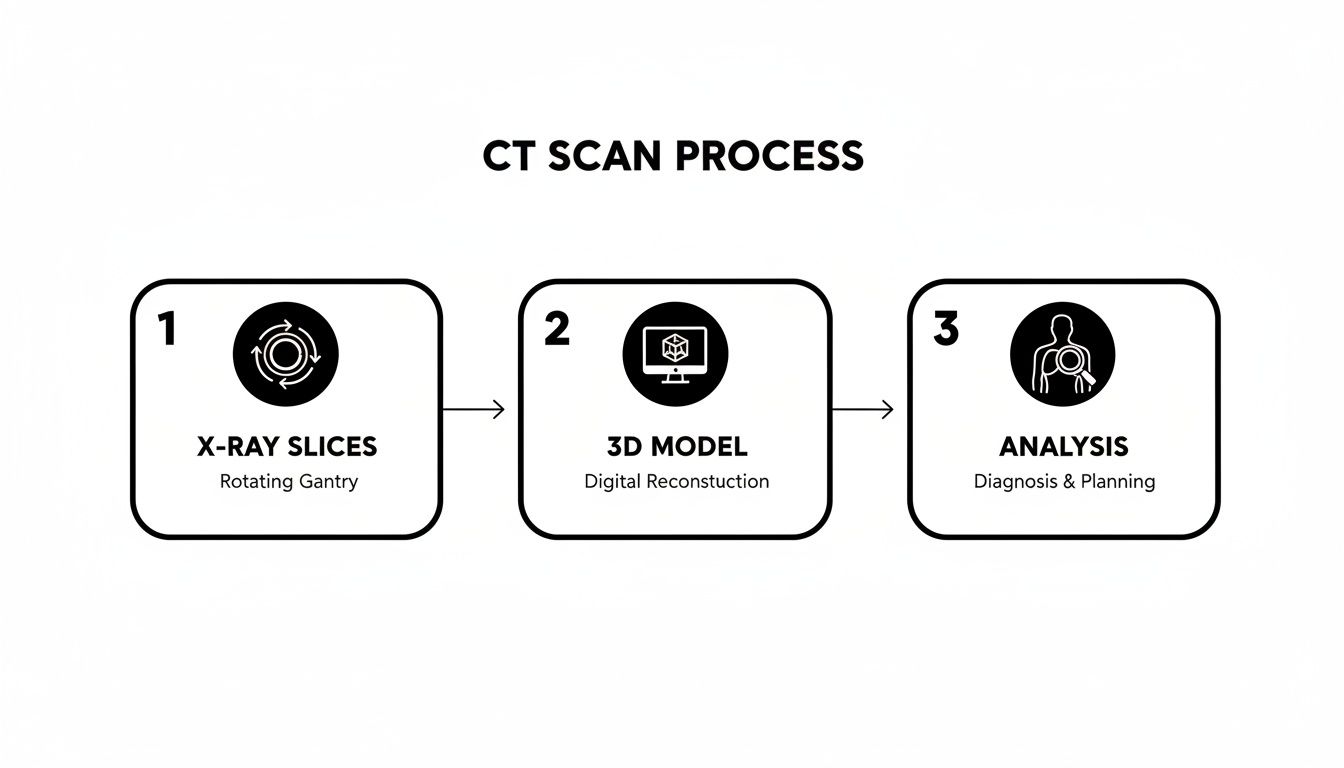
Think of it like assembling a detailed map of your internal anatomy, which we can then examine for anything out of place.
The Bigger Picture on Risk
The conversation about radiation risk becomes more relevant for patients who need multiple scans over many months or years to see how well a treatment is working. Even then, the immediate, critical need to know if a therapy is shrinking a tumor has to be balanced against the cumulative radiation exposure.
CT scans remain an indispensable tool in oncology because they can often spot problems much earlier than you might feel them. Their widespread use, however, has rightly sparked important discussions. One study published in JAMA Internal Medicine estimated that the 93 million CT scans performed in the U.S. in a single year could contribute to approximately 103,000 future cancers over patients’ lifetimes.
These numbers underscore the dual nature of this technology. While it's a powerful ally in the fight against cancer, it's one we must use wisely and judiciously.
Which Cancers Are Most Visible on a CT Scan?

So, can a CT scan find cancer? Absolutely, but it’s not a one-size-fits-all solution. Think of it as a specialist. A CT scan’s real power is in detecting solid tumors, especially those hidden deep inside the body where they can’t be seen or felt during a physical exam.
This makes it an indispensable tool for investigating potential cancers in the chest, abdomen, and pelvis. It gives us an incredibly clear and detailed look inside these complex areas.
The technology is particularly well-suited for a few key areas:
- Lung Cancer: CT scans can pick up on tiny, early-stage lung nodules that a standard chest X-ray would almost certainly miss.
- Abdominal Cancers: It’s one of our go-to methods for identifying tumors in organs like the pancreas, liver, kidneys, and adrenal glands.
- Colorectal Cancer: For staging colorectal cancer, a CT scan is essential. It helps us see if the cancer has spread to nearby lymph nodes or traveled to the liver, which is critical information for treatment planning.
Finding Cancers in the Abdomen and Pelvis
When we’re dealing with potential cancers in the abdomen and pelvis, a CT scan provides what is essentially a detailed anatomical map. This map shows us the tumor’s precise size and shape, but just as importantly, it reveals its relationship to surrounding organs and critical blood vessels.
This information is the foundation for planning any effective treatment, especially surgery. For example, with gynecological cancers, a CT scan delivers vital staging information that guides our entire approach. We cover this topic in much more detail in our guide on how a CT scan helps detect ovarian cancer.
A CT scan's ability to visualize solid masses makes it a cornerstone of modern oncology. For tumors in the chest or abdomen, it provides the detailed "lay of the land" that is essential for making an accurate diagnosis and forming a treatment plan.
Of course, with any powerful tool, there are trade-offs to consider. Scans of the abdomen and pelvis require higher radiation doses and are used frequently. Because of this, some researchers project that CT imaging could potentially contribute to 5% of all annual U.S. cancer cases. One study estimated that these procedures could be linked to 37,500 projected future cancers from a single year of scans. You can read more about these findings from UCSF.edu.
Where CT Scans Are Less Effective
It's just as important to know what a CT scan can't do well. It isn't the primary imaging choice for every situation, and for some cancers, other tools are far better.
A CT is generally less effective for:
- Blood Cancers: Cancers like leukemia or lymphoma circulate in the blood and lymphatic system and don’t typically form the kind of solid tumors a CT is designed to see.
- Surface-Level Cancers: Early-stage skin cancers, for example, are diagnosed visually by a dermatologist and confirmed with a simple skin biopsy.
- Certain Brain Tumors: While a CT can certainly detect a mass in the brain, an MRI is usually the preferred tool. It provides much better detail of the brain's soft tissues, giving neurologists and oncologists a clearer picture.
Why a CT Scan Is Part of a Larger Puzzle
A CT scan gives us an incredibly sharp, detailed picture of what’s happening inside your body. But while it's a powerful tool for finding a suspicious mass, it almost never provides the final word on its own. It's an important first step, but just one step on the path to a clear diagnosis.
The scan can tell us the size, shape, and exact location of an abnormality. The problem is, a lot of different things can look similar on a CT image. A harmless cyst, a pocket of inflammation, or even old scar tissue can show up as a "mass," leaving us with a picture that demands a closer look.
The Gold Standard: A Biopsy
This is why a biopsy remains the absolute 'gold standard' for confirming cancer. No matter how concerning a growth looks on a CT scan, the only way to be 100% sure is to get a small sample of the tissue itself.
A pathologist then examines that sample under a microscope. They're looking for the tell-tale signs of cancer cells, which have a distinct appearance.
Think of it this way: The CT scan is like a detective who finds compelling evidence at a crime scene. But the biopsy is the DNA test that provides undeniable proof, confirming the identity of the cells beyond any doubt.
A CT scan answers the question, "Is there something there?" A biopsy answers the question, "Is it cancer?" Both are essential, but only the biopsy provides the definitive diagnosis needed to start treatment.
Comparing Diagnostic Tools for Cancer
To get the most accurate diagnosis, oncologists almost always need more than one piece of information. Think of it as assembling a puzzle—each test provides a different piece, and only when they’re put together does the full picture emerge. A CT scan is a crucial piece, but it works best alongside other tools.
Here’s a quick look at how these different tests contribute.
Each of these tools gives us a unique perspective. The CT might find a mass, an MRI could clarify how it's interacting with nearby soft tissues, and a PET scan can tell us if it’s metabolically active.
A seasoned oncologist synthesizes all of these findings. By looking at the complete picture, your care team at Hirschfeld Oncology can move forward with confidence, knowing they have the detailed information needed to recommend the most precise and effective treatment plan for you.
Discussing Your Results with an Expert Oncologist

Getting your CT scan report back can feel like a moment where time stands still. Whether the results are what you feared or something entirely unexpected, the words on that page can be overwhelming. This is precisely the moment when having an experienced, compassionate guide is no longer a "nice to have"—it's everything. A diagnosis isn't an endpoint; it's the starting line for creating a plan.
The way a doctor communicates difficult news truly matters. A skilled oncologist knows how to turn a complex medical report into a clear, understandable path forward, which is a critical part of the process and a key factor in how to improve patient experience.
Turning a Diagnosis into a Plan
At Hirschfeld Oncology, we see the person, not just the scan. It’s our firm belief that understanding your results is the first real step toward taking back control. With over 20 years of experience in the field, Dr. Azriel Hirschfeld specializes in looking beyond the images to create a treatment strategy that is truly personalized to you.
We focus on patient-centered care, which means finding approaches that are not only effective but also fit your life. Our expertise in advanced treatments gives our patients hope, even when facing complex situations.
- Targeted Low-Dose Chemotherapy: This isn't a one-size-fits-all approach. We use this method to deliver treatment more precisely, which helps maximize its impact on cancer cells while aiming to reduce the harsh side effects of standard chemotherapy.
- Immunotherapy: Sometimes, the most powerful tool is your own body. Immunotherapy works by activating your immune system to recognize and fight cancer, which can lead to a powerful and lasting response for certain tumors.
Your CT scan results are more than just images; they are a critical piece of your story. Our goal is to listen to that story, understand your unique situation, and work with you to create a care plan that aligns with your health goals and personal values.
For patients in Brooklyn, Williamsburg, Bushwick, and throughout NYC, the next step is a conversation. We’re here to help you make sense of your scan results and explore all your options—options that put your quality of life at the forefront.
To help you prepare for that first important meeting, we’ve put together a guide with key questions to ask your oncologist.
Frequently Asked Questions About CT Scans and Cancer
When you're waiting on a CT scan for answers about cancer, it's natural to have a lot of questions. We get it. Let's walk through some of the most common concerns we hear from patients and their families.
Can a CT Scan Miss Cancer?
It's a tough question, but the honest answer is yes, sometimes a CT scan can miss cancer. This isn't a failure of the technology itself, but a reflection of its limitations.
A tumor might be too small to be picked up, often anything under 6 mm can be difficult to resolve. Other times, it might be hiding in a complex area of the body or have a tissue density so similar to its surroundings that it simply blends in.
This is exactly why a "clear" scan doesn't automatically mean you're in the clear, especially if your symptoms persist. The expertise of the radiologist reading the scan is critical, and it’s why your doctor may suggest another imaging test, like an MRI or PET scan, to get a different view of the situation.
How Long Does It Take to Get CT Scan Results for Cancer?
The technical part of the process moves pretty quickly. A radiologist will typically interpret your scans and send a comprehensive report over to your doctor within 24 to 48 hours.
But you probably won't get those results right away. Your doctor needs time to review the report thoroughly. They will then schedule an appointment with you, usually within a few days to a week, to go over the findings together. This conversation is essential—it allows them to explain what the report means in the context of your health and discuss what comes next.
A "suspicious mass" on a CT scan is a finding that needs further investigation; it is not a final diagnosis. Abnormalities like benign cysts, infections, or even scar tissue can mimic the appearance of a tumor. A biopsy is almost always required to know for sure.
Is a CT Scan with Contrast Better for Detecting Cancer?
In many cases, absolutely. Using an intravenous contrast dye is often the preferred method when looking for or evaluating cancer. Think of it like turning on the lights in a dim room—it makes everything stand out.
The dye travels through your bloodstream, highlighting blood vessels and certain types of tissue. This is incredibly useful because it can:
- Help define the exact edges of a tumor.
- Reveal its internal blood supply, which is a key sign of active growth.
- Create a sharp distinction between the mass and the healthy tissue around it.
This technique is especially powerful for spotting cancers in organs with a rich blood supply, like the liver, kidneys, and pancreas.
At Hirschfeld Oncology, we believe that understanding your results is the first step toward creating a clear, effective treatment plan. If you have questions about a recent scan or want to explore advanced, personalized cancer care options, we invite you to learn more about our approach and schedule a consultation by visiting our site.





.png)


.png)
.png)




