When you first hear the terms “CT scan” and “MRI,” it’s easy to get them confused. At their core, the difference is straightforward: a CT scan uses X-rays, while an MRI uses magnets and radio waves.
Think of a CT as a workhorse. It’s incredibly fast and gives your oncology team a fantastic big-picture view of your bones and internal organs, quickly showing a tumor’s size and general location. An MRI, in contrast, is the specialist. It takes longer but creates exceptionally detailed images of soft tissues, allowing doctors to analyze a tumor’s specific characteristics and see exactly how it’s interacting with nearby nerves, muscles, or blood vessels.
Your First Look at Cancer Imaging Options
After a cancer diagnosis, getting a handle on the tools your care team uses is a huge step toward feeling more in control. CT and MRI scans are the foundations of cancer imaging, but they aren't interchangeable. They’re more like two different kinds of flashlights for exploring a dark room—each one reveals something the other can't.
A CT scan is like a powerful, wide-beam flashlight. It illuminates the whole room in a flash, showing you the major objects and where they are. In cancer care, that speed and broad view are invaluable for things like:
- Initial Staging: Getting a quick, reliable measurement of a primary tumor.
- Detecting Metastasis: Checking to see if cancer has spread to other areas, like the lungs or liver.
- Guiding Biopsies: Creating a clear, real-time map for precise needle placement.
An MRI is more like a focused, high-intensity laser pointer. It meticulously traces the fine details of a single object, revealing its texture, composition, and edges that the wide-beam flashlight would miss. This level of precision is absolutely critical when we need to look closely at soft tissues.
The use of these scans has skyrocketed for a reason. Between 2000 and 2016, CT scan rates in U.S. healthcare systems jumped by 152%, and MRI use surged by over 300%. This just shows how central they’ve become to providing effective cancer care.
CT Scan vs MRI at a Glance for Oncology Patients
Having this basic knowledge can make your conversations with the oncologist much easier. Your doctor will always recommend the right test for your unique situation, but understanding the "why" behind their choice is empowering. It helps you connect the dots on your diagnostic journey, which is a big part of knowing what to expect at your first oncology appointment.
To help you see the differences clearly, here’s a simple table breaking down the key aspects of each scan from a patient’s point of view.
Ultimately, both CT and MRI are powerful allies in your fight against cancer. They give your medical team the detailed information needed to craft the most effective treatment plan for you.
How Each Imaging Technology Actually Works
To really get a feel for why your oncologist might order one scan over the other, it helps to understand what’s happening inside the machine. While both CT and MRI give us an incredibly detailed look inside your body, they get there using completely different physics. This core difference is precisely what makes each one suited for very specific jobs in cancer care.
A Computed Tomography (CT) scan is, at its heart, a souped-up X-ray. Instead of a single, flat image, the CT scanner’s X-ray beam rotates around you as you move through the donut-shaped machine, capturing hundreds of pictures from every conceivable angle.
Imagine trying to see what’s inside a loaf of bread. A regular X-ray is like looking at the loaf from the side—you see the outline but not the details within. A CT, on the other hand, gives you a clear picture of every single slice. A computer then digitally stacks these cross-sectional images to build a detailed 3D model of your organs, bones, and blood vessels. It’s an impressively fast process, often taking just a few minutes.
The Physics of an MRI Scan
A Magnetic Resonance Imaging (MRI) scan is a different beast altogether. It uses no X-rays or ionizing radiation. Instead, it taps into the magnetic properties of the water molecules in your body. Since our bodies are about 60% water, and water is full of hydrogen atoms, we have a lot to work with. These hydrogen atoms act like tiny, spinning magnets.
When you slide into the powerful magnetic tube of an MRI, the machine’s field aligns all of those tiny hydrogen “magnets” in one direction. The scanner then sends out radio wave pulses, which briefly knock the atoms out of alignment. As the atoms snap back into place, they release energy signals that the MRI scanner picks up.
Different types of tissue—like healthy muscle, fat, or a cancerous tumor—have different amounts of water and unique chemical environments. This causes their hydrogen atoms to realign at slightly different rates, producing different signals. The MRI's computer is brilliant at translating these tiny variations into a remarkably detailed picture.
The key takeaway is simple: CT scans use X-rays to see differences in density, making them fantastic for bone and solid organs. MRIs use magnets and radio waves to map water content, which gives them an edge in showing the subtle details of soft tissues, all without radiation.
This is exactly why an MRI can so clearly distinguish a tumor from healthy brain tissue or precisely map a cancer's borders within the soft tissues of the pelvis.
Practical Implications of the Technology
The "how" behind CT vs. MRI directly impacts their "why" in your cancer journey.
CT's Speed and Structure: Because it’s so fast, a CT scan is the go-to for getting a quick, comprehensive survey of the chest, abdomen, and pelvis to look for any signs of cancer spread (metastasis). It’s excellent at spotting solid masses and abnormalities in dense structures.
MRI's Detail and Safety: The magnet-based technology gives us unparalleled soft-tissue contrast. This level of detail is absolutely critical for evaluating tumors in the brain, liver, or reproductive organs, where a surgeon needs to know the exact relationship between the cancer and surrounding healthy tissue. The fact that it’s radiation-free also makes it a better choice for people who may need many scans over a long period.
When you’re facing cancer, the clinical details of a scan are important, but so is the human side of the experience. What will it actually feel like? How long will it take? Is it safe? Knowing the answers to these questions can make a world of difference.
While both CT and MRI are standard, safe procedures, they feel very different from a patient's perspective.
A CT scan is incredibly fast. Most of the time, the scan itself is over in less than a minute. The whole appointment, from check-in to finish, usually takes about 10-15 minutes. You’ll lie down on a table that glides through a wide, open ring—it looks a bit like a giant donut. For most people, it's a straightforward and comfortable process.
The MRI experience is a different story. The machine is a longer, more enclosed tunnel, and you'll need to stay inside it for a while—typically anywhere from 30 to 60 minutes, sometimes longer. Staying completely still is crucial for getting clear images. The machine is also quite loud, making a series of intense knocking and banging noises. Don't worry, though; you'll be given earplugs or headphones to block out the sound.
Understanding Radiation and Magnetic Fields
It's completely normal to have questions about radiation, especially with CT scans. Yes, CT scans do use a very low dose of ionizing radiation to create their images. But in the context of cancer care, this is a carefully managed and necessary tool. The amount of radiation is minimal, and the benefit of getting a precise roadmap of the cancer to guide your treatment is immense. Your oncology team will always ensure the benefits far outweigh the very small risks.
The most significant safety distinction between CT and MRI is that an MRI uses no ionizing radiation. It relies on a powerful magnetic field and radio waves, making it an exceptionally safe option, especially for patients who may require frequent imaging over time.
Because an MRI uses such a powerful magnet, the biggest safety concern is metal. Before your scan, the staff will screen you carefully for any metal on or inside your body. This is a critical step.
They’ll ask about:
- Medical Implants: Things like pacemakers, defibrillators, cochlear implants, or certain older types of aneurysm clips can be a major issue.
- Metal Fragments: If you've ever had an injury involving shrapnel or worked with metal grinding, it's vital to let them know.
- Personal Items: You'll need to remove all jewelry, watches, hearing aids, and even credit cards before you go into the scanner room.
The Role of Contrast Agents
Sometimes, to make certain parts of your body show up more clearly, your scan will be ordered "with contrast." This just means you'll receive a special dye, usually through an IV, that helps highlight blood vessels, organs, or tumors on the final images. The type of dye used depends on the scan.
- CT Scans: Use an iodine-based contrast.
- MRI Scans: Use a gadolinium-based contrast.
Both are considered very safe, and serious reactions are quite rare. You’ll be asked about any allergies and your kidney health beforehand to make sure the contrast is safe for you. It's common to feel a brief warm sensation or a metallic taste in your mouth as the dye goes in—that’s perfectly normal and passes quickly.
To see how imaging fits into the larger diagnostic process, you can learn more about related procedures, like in our guide to the bone marrow biopsy procedure. Understanding the full journey can help put each step into perspective.
Which Scan Is Used for Specific Cancers?
When you're dealing with a cancer diagnosis, choosing between a CT scan and an MRI isn't a toss-up. It's a very specific decision your oncologist makes based on what they need to see and where. Think of it like a detective choosing between a wide-angle lens to get the whole scene and a magnifying glass to inspect a single clue.
The right scan depends entirely on the cancer's location and the kind of detail needed to build the most effective treatment plan. For some cancers, a CT gives the essential big picture, while for others, the granular view from an MRI is absolutely necessary.
Pancreatic and Colorectal Cancers
For cancers buried deep in the abdomen, like pancreatic and colorectal cancer, a CT scan is almost always the first and most important imaging tool. It's incredibly fast and can capture a comprehensive view of the chest, abdomen, and pelvis in one go, which is priceless for initial staging.
A CT scan is brilliant at answering the big questions quickly:
- How large is the primary tumor?
- Has the cancer spread to nearby lymph nodes?
- Are there any suspicious spots (metastases) in the liver or lungs?
This broad survey gives your oncologist a clear roadmap. In pancreatic cancer, for example, a CT can clearly show if a tumor is wrapped around major blood vessels—critical information for a surgeon.
But if that CT scan flags a potential area of concern, especially a suspicious lesion in the liver, your doctor might order an MRI. The MRI’s superior soft-tissue contrast can then definitively tell if the spot is a harmless cyst or a cancerous metastasis with far more certainty than a CT can offer.
Liver and Gynecologic Cancers
When it comes to the liver and pelvic organs, the MRI often takes the lead. The liver is a complex soft-tissue organ, and an MRI's ability to tell different tissue types apart is second to none. It can precisely distinguish a cancerous tumor from a benign growth or a cyst, a difference that can sometimes be hazy on a CT.
This level of detail is just as crucial for gynecologic cancers, like ovarian or uterine cancer. While a CT scan can certainly show a large pelvic mass, it’s the MRI that provides the detailed anatomy needed for precise treatment planning.
An MRI of the pelvis can map out the exact extent of a tumor, showing if it has invaded the bladder or rectum. This detailed information is essential for guiding surgical approaches and planning radiation therapy to target the cancer while sparing healthy surrounding tissue.
Getting a handle on these details can be empowering. You can learn more about how this works in our guide on whether a CT scan can detect ovarian cancer.
Of course, the decision-making process also takes into account practical concerns, like how long a scan takes or whether a patient feels claustrophobic.
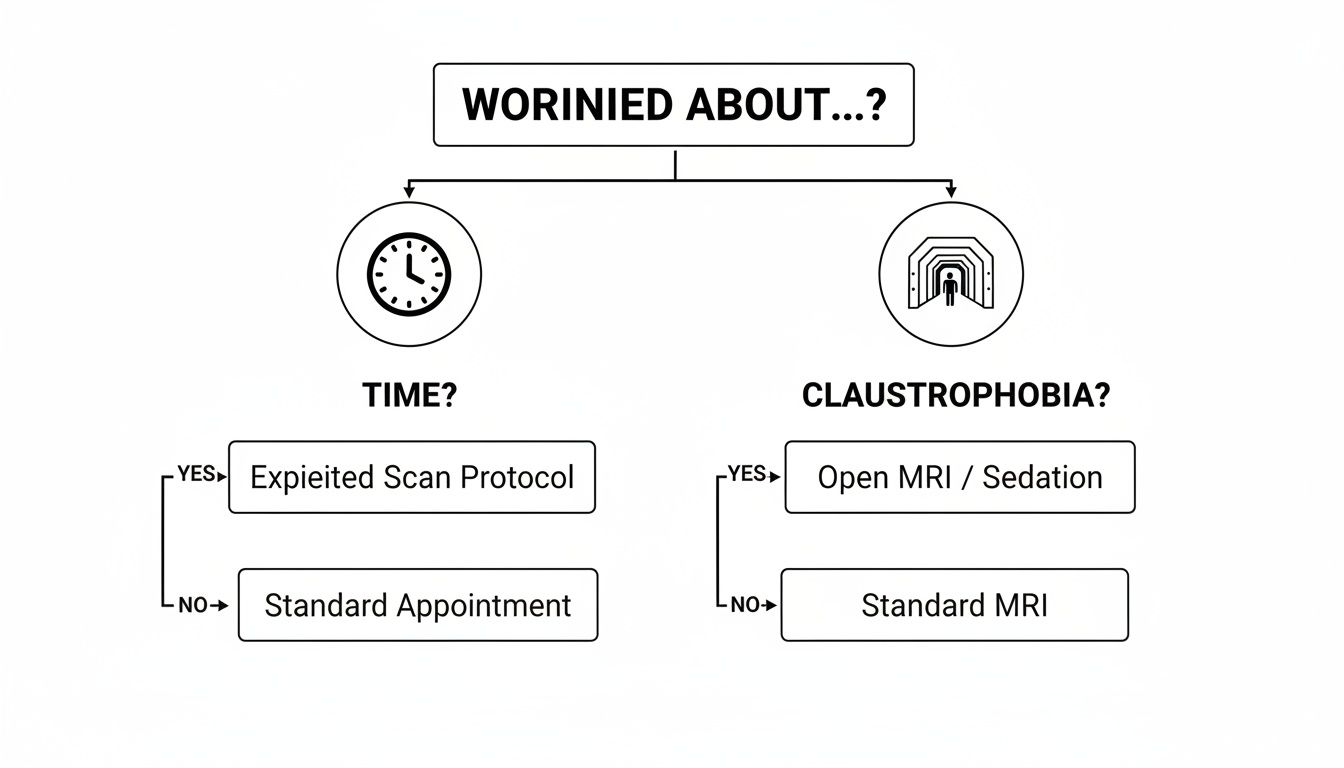
This flowchart shows how we can address patient-specific worries about time or confinement with different imaging choices or supportive measures. For every concern, there's a solution to help you get the imaging you need comfortably.
Brain and Neurological Involvement
When it comes to the brain, there’s no contest: MRI is the undisputed gold standard in oncology. A CT scan might be used in an emergency to quickly rule out major problems like bleeding, but it just doesn't have the sensitivity to pick up the subtle changes that come with cancer.
The brain is the most complex soft tissue in the body, and an MRI’s ability to create high-resolution images of its intricate structures is vital. It can spot both primary brain tumors and tiny metastatic spots that have spread from elsewhere, often long before a CT could.
Recent research underscores just how critical this is. For cancer patients who suddenly develop neurological symptoms, an MRI is far more effective at finding the cause. One analysis of over 1,900 patients found that MRI detected critical brain abnormalities in 12.6% of cases, while CT scans only found them 5.2% of the time. This data strongly supports making MRI the priority for any cancer patient with new neurological signs.
Cost, Availability, and Speed: The Practical Side of Imaging
When we're deciding between a CT and an MRI, the conversation isn't just about the science. We also have to look at the practical side of things—how much it costs, how easy it is to get an appointment, and how long you'll actually be in the scanner. These real-world factors are a big part of your care journey and can influence how quickly we can move forward with your treatment plan.
Scan Time: A Noticeable Difference
One of the first things patients notice is the speed. A CT scan is incredibly fast; the imaging itself often takes less than a minute. This is a huge plus if you're in pain, have trouble staying still, or if we need answers right away.
An MRI is a different story. It's a much longer process, typically lasting anywhere from 30 to 60 minutes. That extended time is what allows the machine to capture such rich, detailed images, but it does require you to lie perfectly still in a fairly confined space.
Finding an Appointment: Availability Matters
You’ll find CT scanners in almost every hospital and most outpatient imaging centers. They are far more common than MRI machines, which usually means more appointment slots and shorter wait times. When your oncologist needs information quickly, the sheer accessibility of a CT can be a game-changer.
Because MRI machines are more complex and costly, there are simply fewer of them around. This can sometimes mean waiting a bit longer for a scan, a factor your care team will definitely weigh when creating your diagnostic timeline.
The key logistical trade-off is often speed and availability versus image detail. A CT can give us answers quickly, but sometimes the superior soft-tissue detail from an MRI is absolutely worth the wait, especially when planning a precise surgery or radiation treatment.
Understanding the Cost of Imaging
Navigating the cost of medical imaging involves understanding the prior authorization process, which can affect both your out-of-pocket expense and how quickly you can get scheduled. In general, an MRI is more expensive, with costs ranging from $1,200 to $4,000, while a CT scan typically falls between $500 and $3,000.
However, these numbers don't tell the whole story. For cancer patients, these scans are medically necessary, and insurance usually covers the vast majority of the cost. Most patients are only responsible for a copay or a small percentage of the total. At a dedicated practice like Hirschfeld Oncology, we always choose the test that will give us the clearest clinical answers, not the one that costs less.
You can find more details about imaging costs and insurance coverage at DocPanel.com.
Your Partner in Cancer Imaging Decisions
Choosing between a CT or MRI scan isn't a decision you have to make alone. It’s a conversation—a critical part of building your personalized treatment strategy. Your oncologist will carefully weigh your specific cancer type, its stage, and your overall health to recommend the right path. As the most important member of your care team, understanding the "why" behind each test is your right.
At Hirschfeld Oncology, clear, patient-focused communication is our promise. We take the time to walk you through exactly why one scan might be better than another for your situation and what we hope to learn from the results. This partnership ensures you feel informed and confident every step of the way.
Navigating Your Journey with Clarity
Of course, practical matters come into play. When thinking about your imaging options, a key financial piece of the puzzle is how your health plan covers existing diagnoses. A detailed guide on insurance for pre-existing conditions can shed light on your coverage, helping you plan for the financial side of things. Having this knowledge lets you focus on what really matters: your health.
The right imaging at the right time provides more than just a picture; it provides a roadmap. It allows us to target treatment with exceptional precision, monitor your progress closely, and adjust your care plan to achieve the best possible outcomes while preserving your quality of life.
Our goal is simple: to demystify this process, replacing uncertainty with clarity and partnership. We firmly believe that precise imaging, paired with a compassionate, collaborative approach, offers the most powerful path forward.
Your journey is yours alone, and your imaging plan should reflect that. We invite you to schedule a consultation with our team. Let’s talk about how our personalized strategies, guided by advanced imaging and open communication, can offer renewed hope and a clear direction for your treatment.
Your Top Questions About CT and MRI Scans
When you're navigating a cancer diagnosis, it's completely normal to have a lot of questions about the tests you'll need. Let’s walk through some of the most common concerns patients have about CT and MRI scans to help clear up any confusion and ease your mind.
Can a CT Scan and an MRI Be Used Interchangeably?
This is a question I hear all the time. While both are powerful imaging tools, CT and MRI are not interchangeable. It’s better to think of them as complementary, each giving your care team a different, essential piece of information at various points in your journey.
One scan doesn't replace the other; they work together to build a complete diagnostic picture.
For example, your oncologist might order a CT scan right after a colorectal cancer diagnosis to get a quick, comprehensive map of your abdomen and see if the cancer has spread. If that scan flags a small, uncertain spot on your liver, an MRI is the perfect next step. Its superior ability to differentiate soft tissues can tell us exactly what that spot is, confirming whether or not it’s something to worry about.
A great way to think about it is this: The CT scan is brilliant at telling us that something is there and its size. The MRI excels at telling us what that something is with much greater certainty.
What If I’m Claustrophobic?
Feeling anxious about being in the enclosed space of an MRI machine is incredibly common and nothing to be ashamed of. Please, always let us know if this is a concern for you. Your comfort is a top priority, and we have several ways to help you get through the scan.
We’ll work together to find what’s right for you. Some options include:
- Open MRI Machines: These scanners are designed with much more open space around you, which can significantly reduce feelings of confinement. They aren't available at every facility, but we can help locate one.
- Mild Sedation: Your doctor can prescribe a mild sedative to help you feel calm and relaxed throughout the scan.
- Comfort and Distraction Techniques: Simple things can make a huge difference. Many patients find comfort in listening to music through headphones, practicing slow and steady breathing, or using other mindfulness exercises.
The most important thing is to talk to us about your fears. We are here to support you and will find a solution that makes the experience manageable.
How Often Will I Need Scans During My Treatment?
There’s no single answer to this, as your imaging schedule is tailored specifically to you. The frequency of your scans depends entirely on the type of cancer you have, your specific treatment plan, and how your body is responding to therapy.
During an active round of chemotherapy, for instance, you might have a scan every few months to check if the tumor is shrinking. Once you move into a maintenance phase or remission, the time between scans could lengthen to every six months or even once a year.
Your schedule is part of an ongoing conversation between you and your oncologist. These scans provide the critical feedback we need to see if your treatment is working and allow us to make any necessary adjustments right away.
The decisions behind your imaging plan are always a partnership. At Hirschfeld Oncology, we believe clear, open communication is key to making you feel confident and informed. To discuss a personalized cancer care strategy, please learn more about our approach at Hirschfeld Oncology Blog.





.png)


.png)
.png)




