When you're facing chemotherapy, the thought of hair loss can be incredibly daunting. It's one of the most visible side effects of treatment, and for many, it's a constant, public reminder of their fight with cancer. But what if you could do something to protect your hair? Cold cap chemo is a therapy designed to do just that, giving many patients a way to keep their hair throughout their treatment journey.
Understanding Cold Cap Chemo and How It Works
The official term is scalp cooling, and it's a process that has helped countless people feel more like themselves during a challenging time. It’s not about vanity; it’s about maintaining a sense of identity and privacy.
The science behind it is surprisingly straightforward but very clever.
The Protective Helmet Analogy
Think of it like putting a protective helmet on your hair follicles before a battle. Chemotherapy drugs are powerful—they have to be to destroy fast-growing cancer cells. The problem is, they can't tell the difference between cancer cells and other healthy, fast-growing cells in your body, like your hair follicles.
A cold cap cools your scalp down to a very low, consistent temperature. You'll wear it before, during, and for a little while after your chemo infusion. This intense cold creates a protective shield for your hair in two key ways.
How Cooling Shields Your Hair
First, the cold dramatically narrows the blood vessels in your scalp. This process is called vasoconstriction. Imagine the chemotherapy drugs traveling through your bloodstream like cars on a highway. By chilling the scalp, we effectively create a traffic jam, severely limiting how much of that powerful medicine can actually reach your hair follicles.
Second, the cold puts the cells in your hair follicles into a sort of temporary hibernation. It slows down their metabolic activity so much that they become dormant. Since chemo is designed to attack cells that are actively dividing, these "sleeping" follicles are no longer an attractive target.
Here is a high-level overview of the most important aspects of cold cap therapy to give you a quick summary at a glance.
Quick Facts About Cold Cap Therapy
This combination of reduced blood flow and cellular hibernation is a powerful defense.
The results can be remarkable. One major study demonstrated an impressive 92.1% overall success rate in preventing major hair loss (which they defined as keeping more than 50% of your hair) for patients who followed the protocol precisely. You can read the full findings about cold cap effectiveness to learn more.
Ultimately, cold cap therapy is about minimizing collateral damage. By creating this cold, protected zone on your head, the chemotherapy can get to work fighting cancer everywhere else, all while giving your hair a fighting chance to stay right where it is.
The Science Behind Preventing Chemo Hair Loss
It’s pretty incredible to think that something as simple as cold can protect your hair during chemotherapy. The way it works is by triggering two key biological responses that work together to shield your hair follicles from the powerful drugs moving through your system.
It’s a smart approach that uses the body’s own natural reaction to cold to create a protective bubble right on your scalp.
Limiting Drug Exposure Through Vasoconstriction
First, let's talk about blood flow. Think of your blood vessels as a massive highway system, delivering chemotherapy drugs to every corner of your body. Your hair follicles are like busy little towns right off the main road, with a rich blood supply that normally keeps them healthy and growing.
When a cold cap is applied, that intense cold immediately causes the tiny blood vessels in your scalp to shrink down. This process is called vasoconstriction. It’s like temporarily closing the off-ramps on the highway leading to your hair. By constricting these vessels, blood flow to the scalp can be reduced by as much as 20-40%.
Less blood flow means far less of the chemotherapy medicine can actually reach and harm your hair follicles. This is the first, and most important, line of defense. The principle of using cold to restrict flow is a core concept in medicine, though it's quite different from the warming effects seen in other treatments like Heat Therapy vs Cold Therapy. For scalp cooling, this restriction is exactly what we want.
Slowing Down Follicle Activity
The other piece of the puzzle is how the cold affects the hair follicles themselves. Chemotherapy drugs are designed to hunt down and attack rapidly dividing cells—which is what makes them so effective against cancer. Unfortunately, the cells in your hair follicles are some of the fastest-dividing cells in your entire body, making them an unintentional target.
The cold essentially puts your hair follicle cells into a temporary state of hibernation.
Imagine your follicles are tiny, high-energy factories working 24/7. The cold sends a signal to power down, dramatically slowing their metabolism. They stop dividing and just go dormant for a while.
Because the chemo is looking for that high-activity signature, these "sleeping" follicles are much less likely to be noticed. They effectively fly under the radar. This is a very different mechanism from hair loss caused by other treatments; for example, you can learn more about why radiation can cause hair loss in a separate article.
So, to put it all together, scalp cooling provides a powerful two-pronged defense. It reduces the amount of chemotherapy that reaches the scalp and makes the hair follicles less vulnerable to the drugs that do get through. This is how it gives your hair a real fighting chance to survive treatment, all without interfering with the chemotherapy's work in the rest of your body.
Understanding Your Chances of Success with Cold Caps
If you're thinking about using a cold cap, your biggest question is probably pretty simple: "Will this actually work for me?" It's a fair question, and while there are no absolute guarantees in medicine, we have a lot of solid research to help you set realistic expectations for your own journey.
The effectiveness of scalp cooling isn't a single, fixed number. It's tied directly to the specific chemotherapy drugs you'll be receiving. Your unique chemo regimen—the combination of drugs, the dosage, and your infusion schedule—is the single biggest factor in determining how well a cold cap can protect your hair.
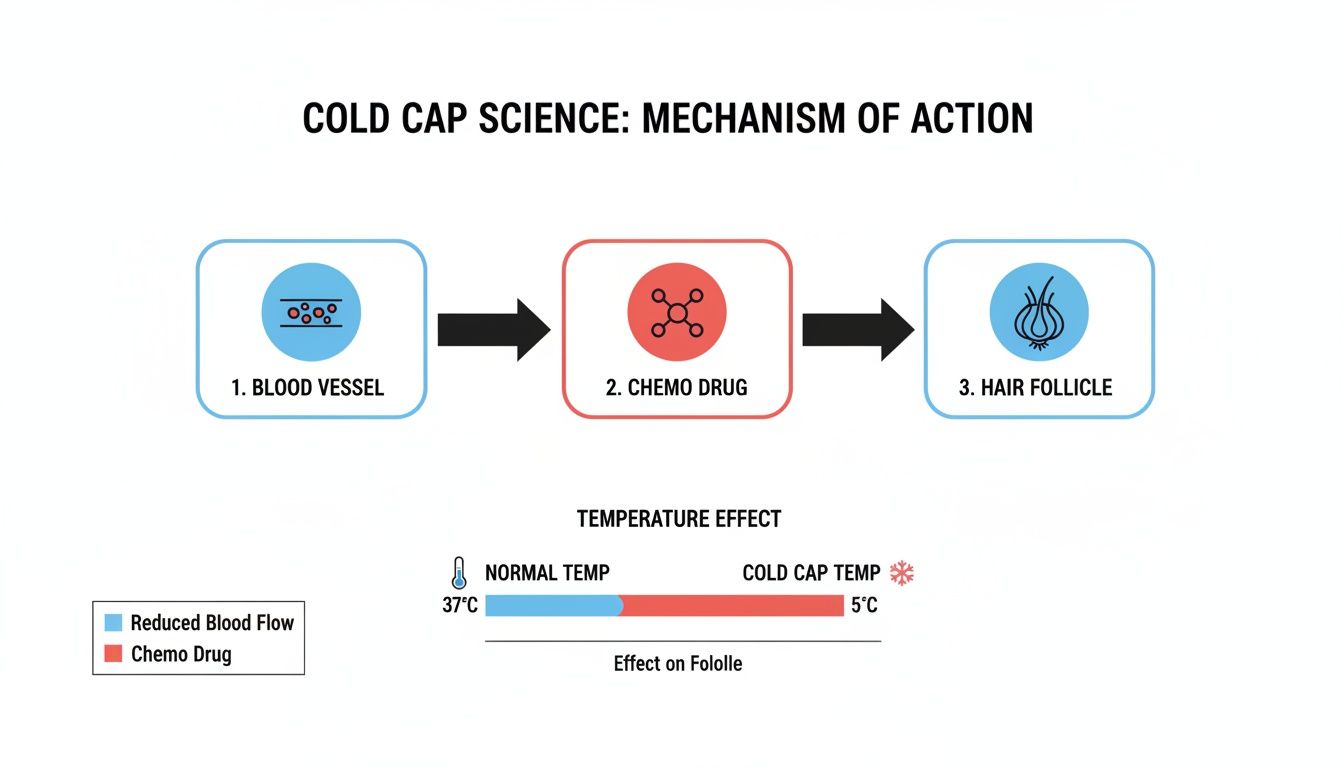
The Science Behind How It Works
So, how does making your scalp cold actually prevent hair loss? It's a fascinating two-part process that creates a protective shield for your hair follicles.
First, the intense cold constricts the blood vessels in your scalp. Think of it like a gatekeeper significantly reducing the amount of traffic on a road. This means far less of the chemotherapy drug can reach your hair follicles in the first place.
Second, the cold temperature slows down the metabolic rate of the hair follicle cells themselves. When these cells are less active, they don't absorb the chemotherapy drugs that do manage to get through as readily. It’s a powerful combination that limits the follicles’ exposure to the damaging effects of the drugs.
Why Your Chemo Regimen Matters Most
Some chemotherapy drugs are simply harder on hair follicles than others. Because of this, success rates with cold capping can vary quite a bit. It helps to think of it like this: the same rain jacket that keeps you dry in a drizzle won't hold up in a hurricane. Similarly, your hair's ability to withstand chemo depends entirely on the strength of the drugs it’s up against.
For instance, two common classes of drugs show very different outcomes:
- Taxane-Based Chemotherapy: Drugs like paclitaxel (Taxol) and docetaxel (Taxotere) are staples in treating breast, ovarian, and lung cancers. Patients receiving only taxane-based drugs tend to see the highest rates of success with scalp cooling.
- Anthracycline-Based Chemotherapy: Drugs like doxorubicin (Adriamycin) and epirubicin are also widely used, especially for breast cancer. These drugs are known to be more aggressive on hair follicles, which often leads to more mixed and sometimes lower success rates.
When a patient’s treatment involves a combination of drugs—like the common "AC-T" regimen that includes both an anthracycline and a taxane—the success rate usually lands somewhere in the middle. The drug that is more toxic to hair tends to have the biggest say in the final outcome.
A Look at the Data
To help put this into perspective, we can look at the real-world success rates for different chemotherapy types. The table below gathers data from several studies to give you a general idea of what to expect based on your specific regimen.
Cold Cap Success Rates by Chemotherapy Type
It’s important to remember these are averages. Your personal results can be influenced by your dosage, overall health, and how well you tolerate the cold cap itself.
One of the largest studies, the Dutch Scalp Cooling Registry, followed 7,424 chemotherapy patients and provided some incredible real-world insights. The study found that 56% of people using scalp cooling did not need a wig or head covering by the end of their treatment.
Success was highest for those on taxane regimens, reaching an impressive 78%. This was significantly higher than the results for anthracyclines (40%) and combination therapies (45%). These numbers line up closely with major FDA studies and give us a reliable picture of what’s possible. You can discover more insights on cold cap efficacy from Paxman to see the detailed data for yourself.
Defining What "Success" Means to You
It's also crucial to understand what "success" looks like when you're scalp cooling. The goal isn't to save every single strand of hair—some shedding is normal and expected. Instead, success is generally defined as retaining more than 50% of your hair. This is typically enough that you don't feel the need for a wig or full head covering.
For many, success is about more than just numbers. It's deeply personal. It’s about looking in the mirror and still seeing yourself. It's about maintaining a sense of privacy and normalcy during a time that is anything but normal.
The decision to use a cold cap is yours alone, but it’s one best made with good information and a clear conversation with your oncology team. By understanding the data and your specific treatment plan, you can decide if this path feels right for you.
Your Step-By-Step Guide to a Cold Cap Treatment Day

Walking into your first cold cap chemo session can feel a little daunting. What will it feel like? How long will it take? Knowing the play-by-play from start to finish helps take the mystery out of the process, giving you a greater sense of calm and control.
A treatment day is more than just the infusion itself. It’s a longer commitment, but it’s a manageable one when you understand its three distinct phases. Let's walk through what a typical day of scalp cooling looks like, from the moment you arrive until you're ready to head home.
Phase 1: Pre-Cooling
The day begins with what’s called pre-cooling. This happens before your chemotherapy infusion even starts and typically lasts between 30 to 60 minutes, depending on the specific scalp cooling system being used. The entire goal here is to get your scalp’s temperature down to its target level before the medicine enters your system.
We won’t sugarcoat it: this is often the most challenging part of the day. The initial sensation is an intense, deep cold that many people compare to the "brain freeze" you get from slurping a slushy too fast. It can be a real shock to the system.
The good news? For almost everyone, this intense feeling starts to fade after the first 15 minutes or so. Your scalp goes numb, and the feeling becomes much more tolerable. Mentally preparing for that initial blast of cold makes it much easier to get through.
Phase 2: Infusion Cooling
Once your scalp is sufficiently chilled, your chemotherapy infusion will begin. This kicks off the second phase: infusion cooling. You'll keep the cold cap on for the entire duration of your treatment, which could be anywhere from one to several hours based on your specific drug regimen.
Your main job during this phase is simply to settle in and get as comfortable as you can. Now is the perfect time for those distractions you brought with you—a good book, a movie on your tablet, or your favorite playlist. Since you’ll be connected to an IV and the cooling machine, your ability to move around will be limited. You can find helpful tips on getting comfortable in our guide to finding a cancer infusion center near you.
“I didn’t realize how much having hair helped you feel like a normal person,” shared one patient who used scalp cooling. “People said, ‘Oh my gosh, you look so good.’ I thought it was superficial, but it really helped how I felt.”
This period is all about maintenance. The cap just keeps doing its job, constricting blood vessels to protect your hair follicles while the chemotherapy goes to work on cancer cells elsewhere.
Phase 3: Post-Cooling
The final and often longest part of your day is post-cooling. After your chemo infusion is finished, you still need to wear the cap for a set amount of time. This step is absolutely critical. It ensures your hair follicles stay protected as the chemotherapy drugs begin to clear out of your bloodstream.
How long you’ll need to post-cool varies quite a bit depending on the chemo drugs you received, ranging from 90 minutes to over 4 hours. Your oncology team will give you the exact timing for your specific treatment. It definitely makes for a longer day at the center, but sticking it out is essential for getting the best possible results from cold cap chemo.
During this time, it's common to feel a few things.
- Headaches: The prolonged cold can cause a mild headache for some people.
- Chills: It’s perfectly normal to feel chilled. This is why we always recommend bringing warm blankets, cozy socks, and extra layers.
- Neck or Shoulder Discomfort: The weight of the cap can sometimes cause stiffness. A good neck pillow can make a world of difference.
By the time your post-cooling is done, the most powerful chemotherapy agents have left your system, making it safe to finally remove the cap. While it's a long haul, each phase is a vital part of protecting your hair and helping you feel more like yourself throughout your cancer treatment.
Is Cold Cap Therapy a Safe Option for You?
One of the first questions on your mind is probably, "Can I use a cold cap?" It’s a great question, and the answer really comes down to a personal conversation between you and your oncology team. While scalp cooling is a fantastic tool for keeping your hair, it isn’t the right fit for every person or every type of cancer.
Let's walk through who tends to be a good candidate and who should steer clear, so you can feel confident in your decision.
Generally speaking, cold cap chemo is most effective and recommended for patients with solid tumors. This covers a lot of ground, opening up the option for many people facing some of the most common cancers.
Who Is a Good Candidate?
You are likely a strong candidate for scalp cooling if you've been diagnosed with a solid tumor and your treatment includes chemo drugs that cause hair loss.
Most patients who successfully use cold caps have one of these diagnoses:
- Breast Cancer
- Ovarian Cancer
- Prostate Cancer
- Lung Cancer
- Pancreatic Cancer
For these individuals, using a cold cap is a proactive way to hold onto a piece of their identity and privacy during a challenging time.
Who Is Generally Not Advised to Use Cold Caps?
On the flip side, scalp cooling is typically not recommended for hematological (blood) cancers. The reason for this is pretty straightforward: these cancers are systemic, meaning they move throughout the entire body via the bloodstream and lymphatic system.
This category includes cancers like:
- Leukemia
- Lymphoma
- Myeloma
The main worry here is a theoretical one. Since cold caps work by constricting blood vessels in the scalp, there's a small but serious risk that the chemotherapy might not fully reach and destroy cancer cells that could be hiding out in the scalp area. To ensure the treatment is as effective as possible everywhere in your body, oncologists almost always advise against scalp cooling for blood-related cancers.
Addressing the Biggest Safety Fear
Naturally, the first thing many people ask is, "If the cold protects my hair follicles, could it also protect cancer cells?" It’s a completely valid concern. The fear is that the scalp could become a "safe haven" for cancer cells to escape chemotherapy, potentially leading to scalp metastases later on.
This question used to be a major point of hesitation for doctors and patients alike. Thankfully, years of dedicated research have given us some very clear and reassuring answers.
A landmark long-term study followed breast cancer patients for seven years. It compared those who used scalp cooling to a control group of 186 patients who didn't. The results were definitive: the rate of scalp and brain metastases was identical in both groups.
The research confirmed there is zero increased risk of cancer returning to the scalp because of cold capping. This study, along with others, has largely put those old fears to rest, showing that for the right patient, scalp cooling is safe.
As a bonus, the same study reported hair preservation success rates between 20% to 45%, highlighting the significant psychological boost it offers alongside its strong safety record. You can read the full research about these long-term results to dig into the findings yourself.
The takeaway is this: for patients with solid tumors, all the evidence we have today shows that cold cap therapy is a safe way to manage one of chemotherapy's most difficult side effects. The next step is to take this information and have a conversation with your oncologist to decide if it’s the right choice for your journey.
How to Prepare for Your Cold Cap Chemo Journey

Once you and your doctor decide that cold cap chemo is a good option for you, it’s time to start thinking about the logistics. Getting organized now can make a huge difference in how smoothly your treatment days go. You’ll need to pick a cooling system, figure out the finances, and coordinate everything with your infusion center.
Let's walk through the key decisions you'll be making so you can feel confident and prepared for what’s ahead.
Choosing Your Scalp Cooling System
Your first big decision is which type of scalp cooling system to use. While they all work by chilling your scalp, how they get the job done can be very different. The two main categories are manual caps and automated machines.
Manual Systems: Think of these as the hands-on, DIY approach. With systems like Penguin Cold Caps, you rent a set of gel-filled caps that are frozen with dry ice in a special cooler. This method requires a helper to swap out the caps every 20-30 minutes during your treatment. The big advantage here is flexibility—you can use them at any infusion center.
Automated Systems: These are more of a "set it and forget it" solution. FDA-cleared machines like Paxman and DigniCap use a single, soft cap connected to a small refrigeration unit. The machine circulates coolant automatically, keeping the temperature perfectly consistent. The catch is that these systems are only available at infusion centers that have invested in the equipment.
Your choice often comes down to what your infusion center has available, your budget, and whether you're up for managing the cap-swapping process.
Navigating the Costs and Financial Aid
For many patients, the cost of scalp cooling can feel like a major obstacle, since it's often not covered by insurance upfront. The total expense for a full course of chemotherapy can run anywhere from $1,500 to $3,000, sometimes more.
The good news is that the financial landscape is definitely getting better. More and more patients are successfully getting reimbursed—at least partially—from their insurance companies. This usually takes persistence and detailed paperwork, but it's worth the effort. Call your provider early to ask about their policy for a "scalp cooling device" or "alopecia prevention."
Many patients don't realize that dedicated financial assistance is available. Non-profit organizations are a critical resource for making cold cap chemo affordable.
Groups like The Hair to Stay Foundation exist specifically to help patients afford scalp cooling. They offer grants based on financial need, which can be a lifeline for covering the costs that insurance won't. Applying for this kind of aid should be one of the first things you do after deciding to move forward.
Coordinating with Your Infusion Center
The final piece of the puzzle is getting in sync with your infusion center. If you’ve chosen an automated system, double-check that they have the machine and that a nurse is trained and available to help you. Remember to factor in the extra time needed for pre- and post-infusion cooling when you schedule your appointments. Our guide on how to prepare for chemotherapy offers more tips on what to expect during treatment.
If you're going with a manual system, clear communication is everything. Give the staff a heads-up that you'll be bringing your own equipment and will likely have a helper with you. Make sure there’s enough space for your cooler and supplies. A little bit of planning with your infusion team can make all the difference on treatment day.
Frequently Asked Questions About Cold Cap Chemo
If you're looking into cold cap therapy, you probably have a lot of practical questions running through your mind. That's completely normal. Getting straightforward answers can help you feel more in control and prepared for what’s ahead. Let's walk through some of the most common concerns we hear from patients considering scalp cooling.
The biggest question is almost always: how much hair will I actually keep? It helps to set realistic expectations from the start. The goal isn't to save every single strand of hair—some shedding is a normal part of the process. True success is defined as significant hair preservation, which for most people means keeping more than 50% of your hair.
When scalp cooling works well, you likely won't feel the need for a wig or full head covering. You’ll still notice more hair than usual in your brush or on your pillow, but you should have enough left to maintain your overall look and feel like yourself in the mirror.
Is the Cold Cap Process Painful?
Another common worry is about pain. We'll be honest with you: it can be uncomfortable, particularly right at the beginning. Most people find the first 15 minutes of cooling to be the toughest part. The sensation is often described as an intense "brain freeze," just like you’d get from eating ice cream too fast.
The good news is that this feeling is temporary. Your scalp quickly adjusts to the temperature and becomes numb, and that initial shock fades into a much more tolerable coldness. A few simple comforts can make a world of difference:
- Warm Blankets: Tucking yourself into cozy blankets from home helps counteract the chill.
- Cozy Layers: Think warm socks, a soft sweater, and maybe even a scarf to keep your body from feeling cold.
- Warm Drinks: Sipping on tea, hot chocolate, or another warm beverage provides a nice, comforting warmth from the inside out.
With a little preparation, most patients find the cold is just a background sensation they can manage for the rest of the treatment.
What Special Hair Care Is Required?
Protecting your hair follicles during chemo is a team effort. While the cold cap does the heavy lifting, a gentle hair care routine is your part of the bargain. Think of your hair as being in a fragile state; it needs to be treated with extra kindness to give it the best chance of survival.
For the duration of your chemo, and for a little while after, it’s best to make a few adjustments:
- Do switch to gentle, sulfate-free shampoos and conditioners.
- Don't wash your hair more than twice a week. This helps preserve the natural oils that protect your scalp.
- Do use a wide-tooth comb to gently detangle, always starting from the ends and working your way up to the roots.
- Don't use any heat styling—put away the blow dryers, flat irons, and curling wands for now.
- Do avoid all chemical treatments, including coloring, perms, or straightening.
Following these simple steps reduces the physical and chemical stress on your hair follicles. This not only maximizes the effectiveness of your cold cap chemo but also supports healthier, stronger regrowth once your treatment is complete.
At Hirschfeld Oncology, our commitment is to provide you with the most effective and supportive care available. If you're considering whether scalp cooling is a good fit for your treatment plan, we invite you to request a consultation with our experienced team. You can explore your options and learn more on our blog.





.png)


.png)
.png)




