Introducing Patient‑Centric Digital Oncology
Real‑time side‑effect data is critical for pancreatic cancer because chemotherapy toxicities such as nausea, fatigue and neuropathy can progress rapidly, and early detection allows dose adjustments and supportive care that keep patients on schedule and reduce emergency visits. A growing suite of FDA‑backed digital platforms—mobile PRO apps, wearable sensors and interoperable dashboards—captures symptoms, vital signs and medication adherence, encrypts the information, and feeds it directly into EHRs for alerts. Hirschfeld Oncology embraces these tools, integrating AI‑driven analytics and storage to personalize treatment, improve quality of life and meet regulatory standards.
Patient Engagement Tools and Digital Communication
 Patient engagement tools are digital solutions—patient portals, mobile apps, secure messaging, and self‑scheduling platforms—that let individuals access test results, log side‑effects, receive medication reminders, and communicate directly with clinicians. In oncology, platforms such as Mobile health apps such as Cancer.Net Mobile and MyChart and AI‑driven apps (e.g., Kaiku Health) enable real‑time symptom reporting, trigger automated alerts, and integrate data into EHRs, improving adherence to complex regimens. Studies show digital intake and reminder systems cut no‑show rates by up to 30 % and raise medication adherence by 6–12 %. Patients report higher satisfaction, greater empowerment, and reduced anxiety when they can track toxicities and receive personalized feedback. Usability hinges on intuitive design, multilingual support, and seamless workflow integration, while privacy concerns demand HIPAA‑compliant encryption and clear consent. Overall, digital communication is viewed positively for cancer care because it facilitates timely interventions and collaborative decision‑making, outweighing workflow challenges when security and training are addressed.
Artificial Intelligence: Assistant, Not Replacement
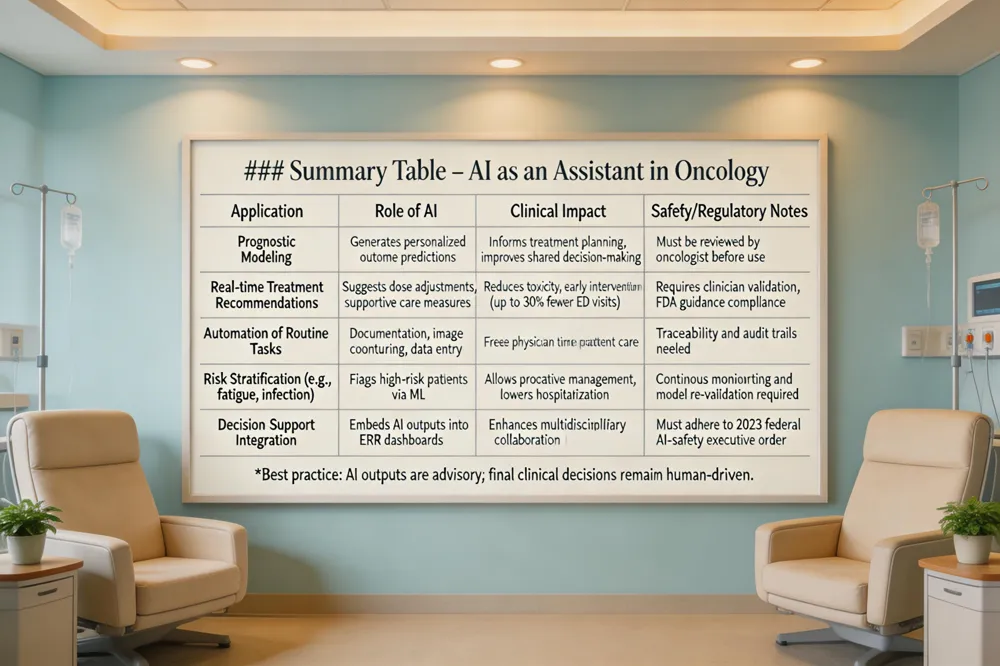 AI will not take over oncology; it will act as a powerful assistant that amplifies oncologists’ expertise. By delivering personalized prognostic insights, real‑time treatment recommendations, and automating routine tasks such as documentation and image contouring, AI frees physicians to focus on direct patient care. Every AI‑driven output must still be reviewed and validated by a human clinician to ensure safety and accuracy, preventing over‑reliance on algorithms.
Patient safety is enhanced when AI rapidly identifies high‑risk conditions—e.g., chemotherapy‑induced fatigue, neuropathy, or early signs of infection—allowing earlier interventions that can reduce emergency department visits by up to 30 % (2021 systematic review). However, without rigorous design, validation, and continuous monitoring, AI tools can miss critical cases. Health‑care organizations must adopt clear safety guidelines, maintain traceability of AI decisions, and establish reporting mechanisms for AI‑related errors, as mandated by recent FDA guidance and the 2023 federal AI‑safety executive order.
Digital oncology, the integration of patient‑reported outcome platforms, wearable sensors, AI‑driven analytics, telehealth, and secure data‑exchange standards, enables real‑time monitoring, personalized treatment adjustments, and improved patient experience. This ecosystem supports value‑based care, early detection of toxicities, and seamless data flow into electronic health records, aligning with the patient‑centered care model advocated by Hirschfeld Oncology.
Real‑Time Health Monitoring Systems and Data Analytics
 Wearable sensors such as smartwatches, Bluetooth patches, and Bluetooth‑enabled thermometers capture continuous vital signs—heart rate, blood pressure, oxygen saturation, temperature, and activity levels—and transmit encrypted data via HIPAA‑compliant mobile apps to secure dashboards. Real‑time analytics dashboards aggregate these streams, apply machine‑learning algorithms, and trigger automated alerts when predefined toxicity thresholds (e.g., fever > 100 °F, rapid weight loss, or sustained tachycardia) are crossed, enabling clinicians to intervene before emergency department visits—studies report up to a 30 % reduction in such visits for oncology patients.
Real‑time health monitoring system – A platform that continuously gathers physiologic data from wearables, combines it with patient‑reported outcomes (PROs) entered into apps like Cancer.Net Mobile, and delivers live alerts to the care team, supporting proactive dose adjustments and supportive care for pancreatic cancer regimens.
Real‑time data analysis in health monitoring systems: a comprehensive systematic literature review – Review of 36 studies (out of 2,822) found machine‑learning especially support‑vector machines, dominates real‑time analysis, improving early symptom detection and diagnostic accuracy across cardiovascular and oncology settings, though no single method fits all conditions.
What is real‑time patient monitoring? – Continuous, instant collection and analysis of vitals and PROs via connected devices, allowing clinicians to spot abnormal trends the moment they occur, predict emerging toxicities, and personalize treatment plans on the fly, thereby reducing hospitalizations and enhancing patient safety.
Remote Patient Monitoring Devices: Types, Approvals, and Popular Solutions
 Remote patient monitoring (RPM) devices are digital medical tools that collect health data outside traditional clinical settings and transmit it to clinicians for review. They include wearables and home‑based gadgets such as blood‑pressure cuffs, pulse oximeters, glucose meters, smart scales, inhaler trackers, and ECG‑capable smartwatches. The devices often operate continuously or on a scheduled basis, sending measurements directly to electronic health records or provider portals.
Wearable remote‑patient monitoring devices enable continuous, real‑time capture of vital signs—heart rate, respiratory rate, temperature, oxygen saturation, and blood pressure—without tethering patients to bedside monitors. Platforms like Medtronic’s BioButton® and Vivalink’s ECG/SpO² patches are integrated into oncology pathways to detect early deterioration, reduce manual charting, and free clinicians for personalized care.
The most popular RPM solution in 2026 is the CardioMEMS HF System, an FDA‑cleared implantable sensor that continuously measures pulmonary‑artery pressure and transmits daily readings via a bedside pillow. Its strong evidence base, seamless data integration, and Medicare‑approved CPT codes have driven widespread adoption, making it the benchmark RPM device across chronic‑disease programs.
Most RPM tools are Class II devices cleared through the FDA 510(k) pathway; only a few high‑risk Class III systems receive full FDA approval. Clinicians should verify each system’s clearance status before clinical integration.
Getting Started with Remote Patient Monitoring
 Defining goals, selecting platforms, and building an RPM team: Begin by setting SMART clinical objectives—e.g., cut emergency‑department visits for pancreatic‑cancer patients by 20% and boost symptom‑reporting adherence. Choose a HIPAA‑compliant platform that integrates with your EHR (e.g., Kyruus Health or Actuvi) and supports oncology‑specific devices such as wearables, Bluetooth thermometers, and smart scales. Assemble a dedicated team: an executive champion, a clinical lead, IT support, and nursing staff to train patients and monitor alerts.
Remote patient monitoring software: RPM software captures real‑time vitals, activity, and patient‑reported outcomes, feeding them into secure cloud storage. AI analytics flag abnormal trends—e.g., rising heart‑rate variability signaling fatigue—triggering automated alerts to the care team. Built‑in billing modules generate CPT codes (99453‑99458) and streamline documentation, turning continuous monitoring into a reimbursable service.
Does Medicare pay for RPM? Yes. Medicare reimburses remote physiological monitoring and remote therapeutic monitoring when data are transmitted on at least 16 of 30 days, the patient has consented, and the service is medically necessary. Billing uses CPT/HCPCS codes 99453, 99454, 99457, and 99458.
What is the latest technology used to monitor patients? The newest solutions combine IoT‑enabled wearables (continuous heart‑rate, activity, temperature) with AI‑driven analytics platforms. Data flow in real time to secure cloud servers, integrate via FHIR into the EHR, and generate predictive alerts that enable early intervention and personalized dose adjustments for oncology patients.
Home‑Based and Continuous Monitoring Devices
 Continuous health monitoring devices
health monitoring wearables and smart rings enable real‑time capture of heart rate, ECG, blood‑oxygen saturation, activity, and sleep patterns. Bluetooth‑enabled blood‑pressure cuffs, pulse‑oximetry clips, and continuous glucose monitors transmit data securely to patient portals, allowing clinicians to spot early signs of hypertension, dehydration, or metabolic imbalance. For patients undergoing pancreatic cancer therapy, these tools provide timely alerts that support proactive dose adjustments and supportive‑care interventions, aligning with Hirschfeld Oncology’s data‑driven care model.
Health monitoring devices for home
Home‑based devices empower patients to log vital signs and symptoms between visits. Key tools include Bluetooth‑enabled blood‑pressure cuffs for cardiovascular monitoring, pulse oximeters for oxygen saturation, glucometers or CGMs for glucose control, and spirometers for lung function. Wearable smartwatches and smart rings continuously record physiological trends, which are integrated via secure telehealth platforms into the electronic health record, enabling Dr. Hirschfeld’s team to personalize treatment plans promptly.
Patient monitoring devices examples
Examples include Bluetooth‑enabled cuffs, glucometers that auto‑send readings, pulse‑oximeter clips for continuous SpO₂ and heart‑rate monitoring, portable ECG units paired with digital stethoscopes, and smartwatches that track activity and sleep. These devices collectively support remote monitoring of side‑effects, facilitate early intervention, and improve patient safety in oncology care.
Digital Health Ecosystem: IoT, DHT, and Clinical Impact
 Digital health technologies are reshaping oncology care by enabling real‑time data capture, remote symptom monitoring, and AI‑driven decision support. These tools improve patient safety, reduce emergency visits, and streamline clinical workflows.
Digital health technology examples
Electronic health records store and share patient data securely. Telemedicine platforms provide virtual visits and real‑time communication. Wearable devices and mobile apps monitor vital signs, activity, and treatment adherence. AI‑driven decision‑support systems analyze imaging, genomics, and clinical notes for personalized therapy. Remote patient‑monitoring tools and digital therapeutics deliver at‑home symptom tracking and medication reminders.
What are 5 examples of IoT used in healthcare?
- Wearable sensors and smart devices (e.g., glucose monitors, activity trackers) that continuously collect and transmit vital signs.
- Implantable and external biosensors measuring heart rate, blood pressure, oxygen saturation with alerting clinicians of abnormalities.
- RPM portals where patients upload home‑device data for remote tracking and treatment adjustment.
- Machine‑learning analytics that process IoT streams to predict disease progression and flag complications.
- Blockchain‑secured EHRs that log IoT‑generated medication and device usage data for immutable, auditable records.
What is DHT in clinical trials?
Digital health technologies (DHTs) such as wearables, implantables, mobile apps, and cloud platforms capture patient‑generated data continuously, often outside the study site. They provide richer, objective endpoints, reduce patient burden, and accelerate safety and efficacy assessments. FDA guidance supports DHT integration to decentralized oncology trials.
How does RPM impact doctor visits?
Remote patient‑monitoring enables 24/7 oversight, allowing clinicians to detect problems early and intervene before they require in‑person care. Patients avoid unnecessary trips, saving time and money, while doctors see fewer emergency visits and can focus on high‑risk cases.
A Future Powered by Real‑Time, Patient‑Driven Data
Digital side‑effect tracking gives patients a voice and clinicians immediate, actionable data. Real‑time PRO platforms cut emergency visits by up to 30%, boost adherence, and personalize supportive care. Wearables and AI analytics turn daily logs into early warnings for nausea, fatigue, neuropathy, and other toxicities. Hirschfeld Oncology leads this shift, integrating encrypted, HIPAA‑compliant apps and dashboards into pancreatic‑cancer protocols, enabling rapid dose adjustments and shared decision‑making. We encourage every patient to log symptoms through approved apps and every provider to act on the alerts, creating a safer, more effective treatment journey.





.png)


.png)
.png)




