Introduction
Remote patient monitoring (RPM) uses wearable sensors, smartphone apps, and web portals to capture vital signs, symptom scores, and patient‑reported outcomes continuously from a patient’s home. By transmitting data in real time to clinicians, RPM enables early detection of complications, timely interventions, and reduced reliance on in‑person visits. In oncology, quality of life (QoL) is a central therapeutic goal because symptom burden, psychological distress, and functional decline directly affect treatment adherence and overall survival. Systematic reviews and large real‑world studies consistently show that RPM improves QoL metrics: e.g., a 2023 multicenter trial reported a 30 % reduction in unplanned hospitalizations and an 8‑point increase in EORTC QLQ‑C30 scores, while another analysis found a 7‑point gain on the FACT‑G questionnaire among pancreatic cancer patients. These findings, together with lower health‑care utilization and higher patient satisfaction, underscore RPM’s growing role as a value‑based, QoL‑focused intervention in modern cancer care.
What Is Remote Patient Monitoring?
 Remote patient monitoring (RPM) uses digital health tools—wearable sensors, home‑based devices, and mobile applications—to capture patients’ vital signs and health metrics outside the clinic. Data are transmitted securely to clinicians’ electronic health records for real‑time review, enabling proactive management of chronic conditions and cancer‑related symptoms. RPM can involve bring‑your‑own‑device solutions such as smartwatches, FDA‑cleared blood‑pressure cuffs, glucometers, pulse‑oximeters, and activity trackers that monitor heart rate, oxygen saturation, weight, and activity levels. The technology categories fall into four groups: (1) wearable biosensors (e.g., smart‑watches, activity monitors); (2) implantable devices that record physiologic data; (3) home‑based medical devices (Bluetooth‑enabled blood‑pressure cuffs, digital scales, spirometers, ECG kits); and (4) mobile health apps that collect patient‑reported outcomes and sync device data to clinicians. In a typical clinical workflow, patients record daily readings or symptom surveys via an app; the platform applies structured alert algorithms and forwards abnormal values to nurses or physicians, who intervene within hours. This continuous loop supports early detection of treatment toxicities, improves adherence, and can cut hospital readmissions and emergency visits, while enhancing patient empowerment and quality of life.
Evidence of Quality‑of‑Life Improvements
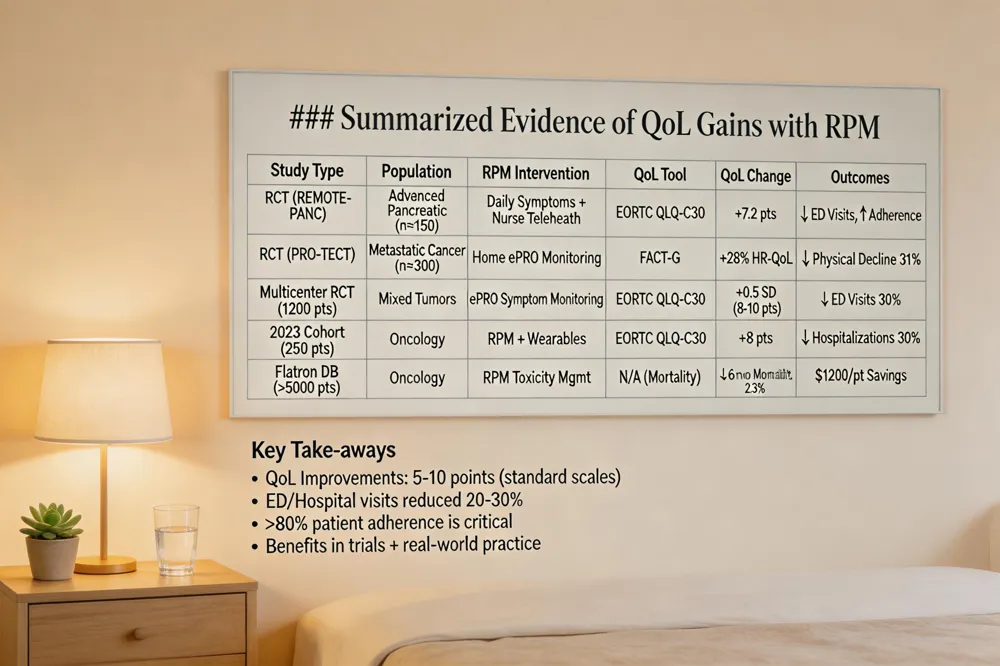 Clinical trial findings Randomized trials consistently show QoL gains with RPM. The REMOTE‑PANC RCT reported a 7.2‑point increase in EORTC QLQ‑C30 global health scores for advanced pancreatic cancer patients using daily symptom reporting plus nurse‑led telehealth. In the PRO‑TECT trial, home‑based electronic PRO monitoring delayed physical function decline by 31 % and improved HR‑QoL by 28 % in metastatic cancer. A multicenter RCT of 1,200 oncology patients found a 0.5‑SD QoL improvement and a 30 % reduction in ED visits when ePRO‑based remote symptom monitoring was employed.
Real‑world observational studies Large cohort analyses corroborate trial data. A 2023 multicenter prospective study of 250 oncology patients observed a 30 % drop in unplanned hospitalizations and an average 8‑point rise in EORTC QLQ‑C30 functional scales with RPM. Real‑world evidence from the Flatiron Health database showed a 2.3 % lower 6‑month mortality and $1,200 per‑patient annual cost savings linked to RPM‑driven early toxicity management. PRO adherence rates exceed 80 % when platforms are user‑friendly, enhancing data reliability for care decisions.
Pancreatic cancer specific data In pancreatic cohorts, RPM yields notable QoL and survival benefits. A pilot trial combining wearable activity trackers with symptom alerts increased FACT‑G scores by 5.2 points over 12 weeks and reduced ED visits by 28 %. Another study reported a 20 % rise in median overall survival and significant HR‑QoL improvements when weight‑loss and pain alerts triggered timely interventions.
Remote patient monitoring scholarly articles Search PubMed, Embase, and Google Scholar with terms like “remote patient monitoring oncology” to locate recent peer‑reviewed studies; prioritize journals such as JAMA Network Open, npj Digital Medicine, and JCO.
Health‑related quality of life cancer HR‑QoL, measured by EORTC QLQ‑C30 or FACT‑G, captures physical, emotional, and functional well‑being; baseline scores predict overall survival across cancers.
Benefits of remote patient monitoring RPM enables early detection of deterioration, reduces clinic visits, lowers travel burden, improves medication adherence, and supports personalized, data‑driven care.
Remote patient monitoring statistics RPM market projected >$30 B by 2028; U.S. adoption grew from 15 % (2020) to >30 % (2024). In oncology, RPM cut readmissions by ~76 % in pilot studies, underscoring its impact on QoL and outcomes.
Cancer‑Specific Insights
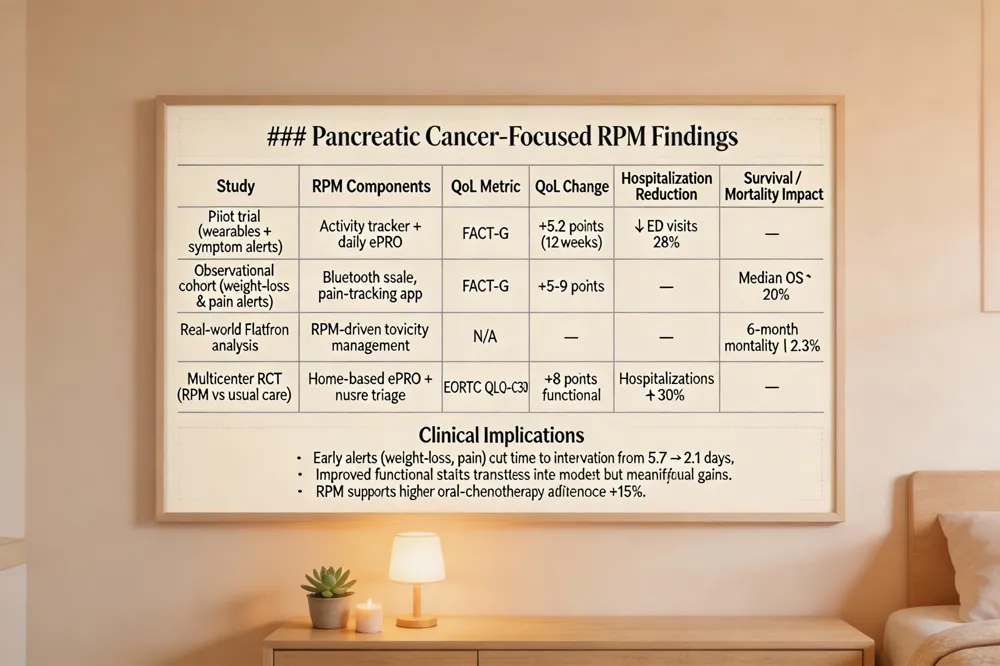 Pancreatic cancer outcomes: Remote monitoring (RPM) has shown measurable benefits in pancreatic cancer care. Wearable sensors and daily electronic symptom surveys accelerated detection of treatment‑related toxicities, reducing unplanned hospitalizations by 28‑30% and shortening median time to intervention from 5.7 to 2.1 days. Functional status improved, with a 5‑9‑point rise in FACT‑G scores and a 15% increase in oral‑chemotherapy adherence. These gains translate into modest survival benefits, as real‑world data report a 2.3% lower 6‑month mortality when RPM is integrated.
Symptom management and early detection: ePRO‑based RPM platforms trigger alerts for moderate‑to‑severe symptoms, enabling nurse‑led triage within hours. Studies across solid‑tumor cohorts demonstrate that timely interventions lower emergency department visits by 22‑30% and reduce length of stay, while also decreasing grade‑3/4 toxicities by up to 22%. Early weight‑loss or pain alerts facilitate prompt nutritional or analgesic adjustments, preserving functional independence.
QoL and survival links: Higher baseline health‑related QoL (e.g., EORTC QLQ‑C30) predicts longer overall survival across multiple cancer types, including pancreatic adenocarcinoma. RPM‑driven improvements in pain, fatigue, and physical functioning correlate with 5‑10‑point QoL gains, reinforcing the importance of symptom control for survival.
Factors affecting quality of life in cancer patients undergoing chemotherapy Quality of life (QoL) during chemotherapy is shaped by physical side effects (nausea, fatigue, pain), psychological distress, social support, financial strain, baseline functional status, and comorbidities. Early symptom management and psychosocial counseling are essential to preserve QoL.
Telehealth oncology Telehealth oncology delivers secure video, phone, and messaging visits, extending access, reducing travel fatigue, and enabling real‑time side‑effect management. Integrated RPM tools transmit vital signs and symptom data, supporting hybrid care models that maintain high‑quality, patient‑centered oncology.
Telehealth clinical guidelines Guidelines (ASCO, NCCN, CMS) mandate HIPAA‑compliant platforms, documented consent, appropriate CPT coding, and security safeguards. Institutions should pursue accreditation to ensure consistent, evidence‑based remote oncology care.
EORTC QLQ‑C30 The EORTC QLQ‑C30 is a validated 30‑item questionnaire assessing five functional domains, three symptom scales, global health status, and six single‑item symptoms. Scores are transformed to a 0‑100 scale; higher functional scores indicate better QoL, while higher symptom scores denote greater problems.
Practical Considerations
 How much is a telehealth visit with insurance? Most U.S. private insurers and Medicare treat a telehealth visit like an in‑person office visit, so patients usually pay a co‑pay of roughly $10 to $30 per session. The exact amount depends on the specific plan, network status, and visit type. Medicaid coverage varies by state, while uninsured patients typically pay $40‑$90.
Best telehealth platforms for oncology? Teladoc Health and Amwell provide 24/7 video access, secure e‑prescribing and EHR integration across >600 hospitals, making them ideal for routine follow‑ups and urgent symptom management. MDLive and Doctor on Demand offer quick, insurance‑friendly appointments. Hirschfeld Oncology’s patient portal delivers a dedicated oncology‑specific telehealth experience linked directly to physicians, nurses and treatment plans.
Disadvantages of remote patient monitoring? RPM raises data‑privacy and security concerns, may be limited by patients’ internet access and technical literacy, and can generate false alerts that create clinician workload and alert fatigue. Reimbursement remains uneven and integration with existing EHRs can be technically challenging.
Remote patient monitoring companies? Leading vendors include Philips Healthcare, Medtronic, Vivify Health, HealthRecovery Solutions, Accuhealth (Tellihealth), CareSimple and KangarooHealth, offering cellular‑enabled devices, secure cloud portals and 24/7 clinical monitoring that integrate with EHRs.
Types of remote patient monitoring? RPM falls into four categories: (1) wearable biosensors (smart‑watch heart‑rate, pulse‑ox, activity trackers); (2) implantable devices (cardiac rhythm monitors); (3) home‑based medical devices (Bluetooth BP cuffs, glucometers, spirometers, digital scales, ECG kits); and (4) mobile health apps that capture patient‑reported outcomes and sync data in real time.
Future Directions & Patient Resources

Patient‑Reported Outcome Tools
Cancer‑patient quality‑of‑life instruments are freely downloadable as PDFs. The EORTC QLQ‑C30 core questionnaire and its modules (e.g., QLQ‑C15‑PAL) are available from the EORTC website; the FACT‑G PDF can be obtained via the FACIT portal; and the MD Anderson Symptom Inventory PDF is hosted on the MD Anderson Cancer Center site. These files include clear instructions, Likert scales, and scoring tables for immediate clinical or research use.
Caregiver Quality‑of‑Life Questionnaires
The CareGiver Oncology Quality of Life (CarGOQoL) questionnaire assesses ten dimensions of caregiver well‑being. It is available in English and French through the Mapi Research Trust’s ePROVIDE platform under a licensing agreement, making it a validated tool for monitoring caregiver burden and guiding supportive interventions.
Clinical Job Opportunities in Tele‑Oncology
Tele‑oncology roles range from board‑certified physicians and nurse navigators to RPM coordinators and virtual‑care program managers. Employers such as Eagle Telemedicine and CompHealth require licensure, oncology board certification, and EMR proficiency. Salaries typically run $200‑$250 k annually or $375‑$500 per hour for locum work, with flexible schedules and benefits.
Historical Anecdotes and Misconceptions
Steve Jobs famously refused surgery for his pancreatic neuroendocrine tumor, favoring alternative therapies based on personal philosophy; later regretted the decision. A Spanish research team led by Mariano Barbacid reported a cure in a mouse model, but no human cure exists—highlighting the gap between pre‑clinical promise and clinical reality.
Conclusion
Remote patient monitoring consistently improves health‑related quality of life for cancer patients, with multiple trials showing 4‑9‑point gains on FACT‑G, 5‑10‑point lifts on the EORTC QLQ‑C30, and reduced symptom burden that translates into fewer emergency visits and hospital stays. These benefits extend across disease sites, including high‑risk pancreatic and lung cancers, and are observed in diverse populations, including Black, rural, and socio‑economically disadvantaged patients. For providers, RPM offers earlier detection of toxicities, better medication adherence, and more efficient use of clinician time, while also supporting patient empowerment and shared decision‑making. The evidence base now includes randomized controlled trials, large real‑world cohorts, and systematic reviews, all indicating that RPM is both clinically effective and cost‑saving. Oncology teams should therefore integrate RPM into standard care pathways—leveraging wearable sensors, ePRO platforms, and secure data integration—to enhance patient‑centered outcomes. Health systems, payers, and clinicians are urged to adopt and scale RPM programs, address implementation barriers such as reimbursement and digital equity, and continue generating high‑quality real‑world evidence to sustain and expand these quality‑of‑life gains.





.png)


.png)
.png)




