For most people, the first thought that comes to mind with chemotherapy is the dread of severe nausea and vomiting. It’s a fear we hear every day. But the reality of modern cancer care is that anti-nausea drugs, what we call antiemetics, have truly changed the game.
Think of it less like a battle against sickness and more like having a dedicated security detail that works around the clock to keep you feeling well. This guide will show you how we can manage this common side effect, allowing you to approach your treatment with a sense of control and confidence.
Taking Control of Chemotherapy-Induced Nausea

Chemotherapy-Induced Nausea and Vomiting (CINV) used to be an almost guaranteed part of treatment. Thankfully, those days are largely behind us. With today’s medical advances, severe nausea is something we can often prevent entirely, not just treat after it starts.
At Hirschfeld Oncology, our entire philosophy is built on being proactive. We don't wait for nausea to become a problem. Instead, we start by figuring out your personal risk level and then design a plan to head off symptoms before your first infusion even begins. We believe that protecting your quality of life is fundamental to your cancer treatment.
Your Partners in Comfort
Your oncology team is your greatest ally in staying comfortable. We see it as our job to make sure you understand exactly which anti-nausea medications you’re getting, why you’re getting them, and what to do if you feel even a little bit off. This teamwork puts you in the driver’s seat.
Feeling well enough to eat a meal, enjoy time with your family, and go about your day is not a luxury—it's a crucial part of the healing process. Our mission is to make your treatment journey as smooth as possible so you can focus on getting better. For more great advice, you can also check out this practical resource on What Helps With Chemo Nausea?.
The modern approach to CINV is one of prevention, not just reaction. By anticipating and blocking the body’s nausea signals, we can help patients maintain their strength and well-being throughout their treatment course.
In this guide, we'll pull back the curtain on how we make that happen. We will walk you through the different types of anti-nausea drugs, explain how they work, and show you how we create a regimen just for you. Specifically, we'll cover:
- The main classes of antiemetic medications.
- How we plan for acute, delayed, and even anticipatory nausea.
- Simple, non-drug tips that can make a big difference.
Getting a handle on these basics will help you work closely with your care team. It ensures your path forward is defined by resilience and healing, not by manageable side effects.
How Anti-Nausea Drugs Protect Your Body

Think of nausea as a series of biological dominos. Chemotherapy can tip the first one over, starting a chain reaction that ultimately tells your brain to feel sick. The job of modern anti-nausea medications, or antiemetics, is to strategically remove a few of those key dominos so the chain reaction never completes.
These drugs are so foundational to cancer care that they've spurred a massive field of research. In fact, the global antiemetics market is expected to grow from USD 9.38 billion in 2025 to over USD 15.76 billion by 2035. This makes sense when you consider that Chemotherapy-Induced Nausea and Vomiting (CINV) can affect up to 70-80% of patients, depending on their treatment. If you're interested in the forces driving this innovation, you can explore more about these market trends and what they mean for patients.
At Hirschfeld Oncology, we don't just rely on one medication. We build a personalized defense for you by combining different classes of drugs, each one blocking a different part of the nausea pathway. It's about creating a comprehensive shield.
To give you a clearer picture, here's a quick breakdown of the main categories of anti-nausea drugs we use.
A Quick Look at Anti-Nausea Drug Classes
| Drug Class | How It Works (Mechanism of Action) | Common Examples |
|---|---|---|
| Serotonin (5-HT3) Antagonists | Blocks serotonin signals sent from the gut to the brain's vomiting center. Excellent for acute nausea. | Ondansetron (Zofran), Palonosetron (Aloxi) |
| NK-1 Receptor Antagonists | Blocks Substance P in the brain's trigger zone. Crucial for preventing delayed nausea. | Aprepitant (Emend), Rolapitant (Varubi) |
| Corticosteroids | Provides broad anti-inflammatory effects that calm nausea pathways. Often used in combination. | Dexamethasone |
| Dopamine Antagonists | Calms the brain's chemoreceptor trigger zone by blocking dopamine. | Prochlorperazine (Compazine), Metoclopramide (Reglan) |
As you can see, each class has a specific job. Now let's dig a little deeper into how the two main players work to protect you.
Blocking the Initial Gut-to-Brain Signal
One of the body's first reactions to certain chemotherapies is irritation in the stomach and intestines. When this happens, the cells lining your gut release a flood of a chemical messenger called serotonin. This serotonin then latches onto nerve endings that fire off a direct "I feel sick!" signal to the brain.
This is where the most common class of antiemetics, the Serotonin (5-HT3) Antagonists, steps in.
- Their Job: They act like signal blockers, physically attaching to the serotonin receptors on those nerve endings. The message is sent, but it never gets delivered.
- Who They Are: You'll probably recognize names like ondansetron (Zofran) and palonosetron (Aloxi).
- When They're Used: These are our go-to drugs for preventing acute nausea—the kind that can pop up in the first 24 hours after your infusion.
By shutting down this very first signal, we can often stop nausea before it even has a chance to start.
Quieting the Brain's Nausea Control Center
There's another, more persistent pathway that involves a different part of your brain. This "command center" is highly sensitive to a potent chemical called Substance P. When Substance P docks with its target, the neurokinin-1 (NK1) receptor, it triggers a strong and often lasting wave of nausea.
This particular pathway is notorious for causing delayed nausea, the kind that can sneak up on you a day or two after your treatment. That's why we bring in the NK1 Receptor Antagonists.
These drugs essentially jam the lock. They fit perfectly into the NK1 receptor, blocking Substance P from ever binding to it. It’s a highly effective way to shut down one of the brain’s most powerful nausea-inducing pathways.
This mechanism is what gives you multi-day protection, helping you feel well long after you've left the clinic. Drugs like aprepitant (Emend) are designed specifically for this purpose.
Finally, we round out your regimen with supporting players. Corticosteroids like dexamethasone reduce overall inflammation, which helps quiet down nausea signaling, while others like dopamine antagonists calm different trigger points in the brain. By understanding how these all work together, you can see how the team at Hirschfeld Oncology layers these medications to build a protective shield that's made just for you.
Understanding the Timeline of Chemo Nausea
Nausea from chemotherapy isn't a one-size-fits-all problem. It actually follows a predictable timeline, with different types of nausea showing up at different points. As your oncology team, understanding this rhythm is key. It allows us to be one step ahead, using specific anti-nausea medications to protect you during each phase of your treatment cycle.
We think of it as building a layered defense. We know when nausea is most likely to hit, so we make sure the right protection is already in place before it starts. The three main patterns we plan for are acute, delayed, and anticipatory nausea.
The First 24 Hours: Acute CINV
The first wave we prepare for is called acute CINV (Chemotherapy-Induced Nausea and Vomiting). This is the nausea that can pop up within the first 24 hours after your infusion. It’s your body's immediate reaction to the chemotherapy, driven largely by a flood of serotonin released from cells in your gut.
To head this off, we give you powerful, fast-acting anti-nausea drugs right through your IV before the chemotherapy even starts. These are usually a combination of a serotonin (5-HT3) antagonist and sometimes an NK-1 receptor antagonist.
This pre-treatment IV medication is your front-line defense. The goal is simple: block the "I feel sick" signals from ever reaching your brain, stopping acute nausea in its tracks.
By giving you these meds at the infusion center, we're providing immediate coverage when you're most vulnerable. It’s why many people feel surprisingly good on their actual treatment day—the heavy-duty protection is already on board and working hard.
Days Two Through Five: Delayed CINV
Just when the risk of immediate nausea starts to fade, a different kind can creep in. We call this delayed CINV. It typically shows up anywhere from 24 to 72 hours after treatment and can linger for a few days.
This delayed nausea is triggered by a completely different set of signals in the brain, mainly involving a chemical called Substance P. Since the cause is different, the solution has to be different, too. This is exactly why we send you home with a pouch of pills and a very specific schedule for taking them.
Your take-home prescription plan is designed to fight delayed nausea and often includes:
- NK-1 Receptor Antagonists: Drugs like aprepitant (Emend) are the workhorses here. They are specifically designed to block Substance P.
- Corticosteroids: You'll likely have a short course of a steroid like dexamethasone to help reduce inflammation and quiet down the nausea pathways.
- “As-Needed” Medications: We also give you a backup, like ondansetron (Zofran) or prochlorperazine (Compazine), to take if you feel any "breakthrough" nausea despite your scheduled meds.
Sticking to your pill schedule is non-negotiable. Missing even one dose can open the door for nausea to gain a foothold, and once it does, it's much tougher to get back under control. If you're wondering how long other side effects might stick around, you can learn more about the general timeline of chemo side effects in our detailed guide.
Before Treatment Even Starts: Anticipatory CINV
The third type is a bit of a curveball because it’s driven by the mind. Anticipatory CINV is a learned response where your brain starts connecting the cancer center itself—the smells, the sights, the sounds—with feeling sick. It can make you feel queasy before a nurse has even touched your port.
This usually only happens when nausea wasn't well-managed during earlier treatments. Your brain, trying to protect you, creates a powerful mental shortcut. Suddenly, the scent of an alcohol wipe or the look of the infusion chair can become a trigger for nausea.
Managing this requires a different set of tools:
- Anxiolytics: Anti-anxiety medications like lorazepam (Ativan) are excellent for calming the nervous system and short-circuiting this learned response.
- Behavioral Techniques: Things like guided imagery, deep breathing exercises, or mindfulness can help your brain break the negative connection.
Honestly, the best way to deal with anticipatory nausea is to prevent it from ever developing. By controlling acute and delayed nausea effectively from your very first infusion, we can keep your brain from learning that unhelpful association. It's all part of a comprehensive plan to protect your quality of life at every step.
Building Your Personalized Anti-Nausea Plan
When it comes to preventing Chemotherapy-Induced Nausea and Vomiting (CINV), a one-size-fits-all approach just doesn't work. Think of it like a custom-tailored suit versus one bought off the rack—the fit makes all the difference. At Hirschfeld Oncology, we don't just hand you a standard prescription. Instead, we work with you to design a personalized anti-nausea strategy built around your specific situation.
This process is a partnership. We begin by looking at a few key factors to map out a plan with the highest chance of success, starting from your very first treatment. Our primary goals are always your comfort and quality of life.
The Blueprint of Your Regimen
Your personalized plan is built on a foundation of three critical pieces of information. Each one gives us vital clues about how to best protect you from nausea and vomiting.
- Your Chemotherapy Drugs: This is the most important starting point. Different chemo agents carry different levels of emetogenic (nausea-causing) risk. A plan for a low-risk drug will look very different from one designed for a high-risk agent.
- Your Personal History: We also need to understand your individual risk factors. Have you had nausea with past surgeries? Do you get motion sickness? Are you female? These details help us gauge your natural sensitivity.
- Your Past Experiences: If you’ve had chemotherapy before, your response to previous anti-nausea drugs gives us an invaluable roadmap. We can see what worked, what didn’t, and build from there.
By combining these elements, we move from a general strategy to one that is specifically calibrated for you.
The timeline of nausea is also a critical factor. Different medications are needed at different times, as this flowchart shows.
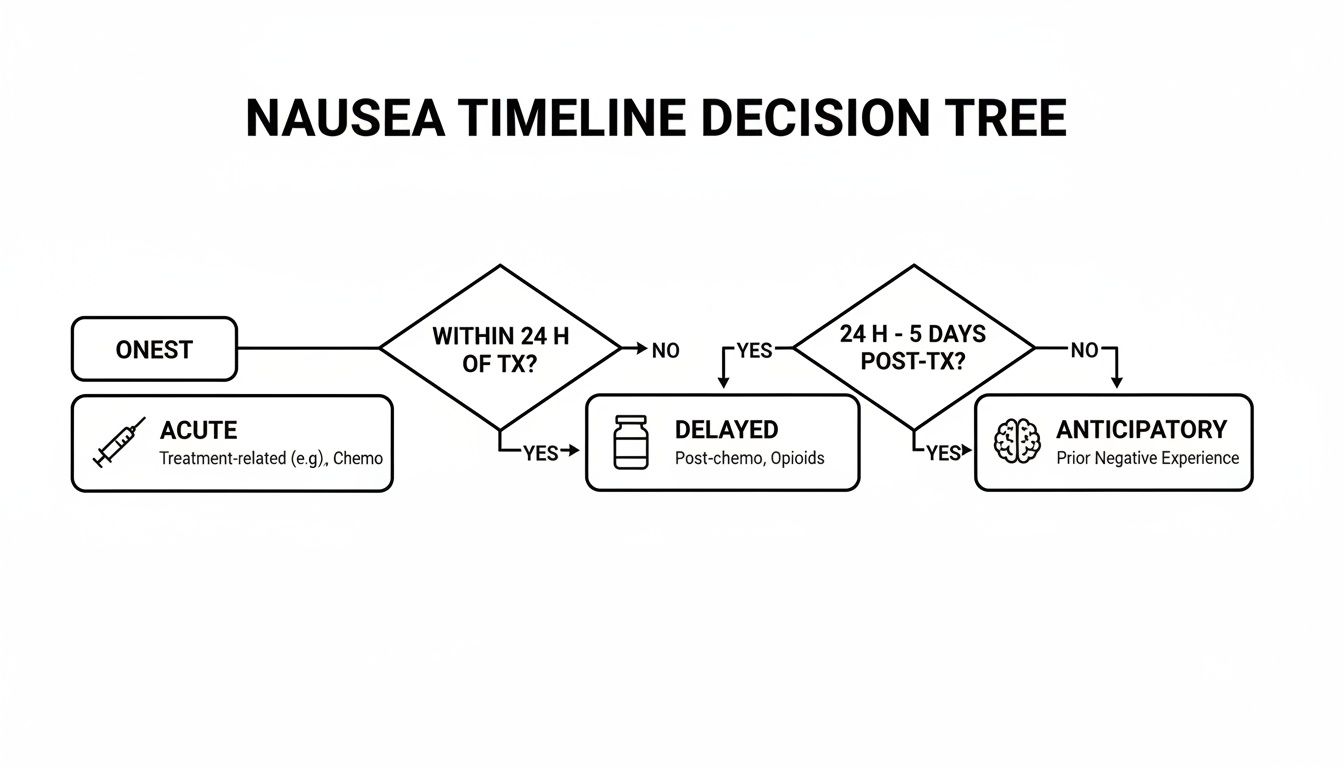
As you can see, a solid plan has to account for the acute, delayed, and even the psychological side of CINV.
How Plans Differ Based on Risk
Let's look at a couple of real-world examples to see how this works. A patient receiving a highly emetogenic chemotherapy agent often gets a powerful, three-drug combination to stay ahead of nausea.
- During Infusion: This might involve an IV cocktail of a serotonin antagonist (like palonosetron), an NK-1 antagonist (like fosaprepitant), and a corticosteroid (dexamethasone).
- At Home: You would then go home with a schedule of oral pills for the next 3-4 days. These often include an NK-1 antagonist and dexamethasone to prevent delayed nausea from setting in.
On the other hand, a patient on a low-risk regimen may only need a single dose of dexamethasone or another mild anti-nausea drug given right before their infusion. In that case, no scheduled take-home pills would be required. This tailored approach ensures you get the exact level of protection you need without being over-medicated.
This focus on personalized care is a major part of modern oncology. The global antiemetics market, valued at $8.48 billion in 2025 and set to grow in 2026, is largely driven by the need to manage CINV, which can affect up to 80% of patients. Advanced infusion centers like Hirschfeld Oncology are at the forefront, using the most effective serotonin-receptor antagonists via IV for rapid relief and embracing sophisticated combination therapies. It's a mission that aligns perfectly with our goal of providing effective, low-toxicity care. You can read more about the latest antiemetics market analysis to see how the field is evolving.
The Most Important Factor is You
Ultimately, the most critical part of your anti-nausea plan is your feedback. No plan is set in stone.
We start with the best evidence-based regimen for your situation, but your real-world experience is what allows us to perfect it. If you feel even a hint of nausea, we need to know.
Communication is absolutely essential. Are you feeling queasy an hour after your infusion? Or is it sneaking up on you two days later? Is a certain smell triggering it? This information helps us fine-tune your medications with precision.
Based on your feedback, we might adjust a dose, switch one drug for another in the same class, or add a new medication to target a specific symptom. Your comfort is our priority, and getting there is a collaborative effort. Never hesitate to call our clinic—your input is what makes your personalized plan work.
Managing Side Effects of Nausea Medication
It can feel frustrating when the medicine you take to fix one problem creates another. But with modern anti-nausea drugs, the goal is always to make a good trade—swapping severe nausea for a much smaller, more manageable side effect. Knowing what to expect is the first step in handling these issues and staying on track with your treatment.
Many of these side effects are quite mild and don't last long. For example, the powerful serotonin (5-HT3) antagonists like ondansetron (Zofran) are fantastic at stopping nausea signals, but in doing so, they can sometimes slow down your digestive system and lead to a headache or constipation.
Likewise, the NK-1 antagonists that we use to prevent delayed nausea might leave you feeling a bit tired or cause hiccups. Corticosteroids such as dexamethasone are notorious for giving a burst of energy or causing insomnia, which is exactly why your team will probably tell you to take them first thing in the morning.
Common Side Effects and Simple Tips
Most of these issues are not alarming and can be managed easily at home. Your care team will give you specific advice, but here are a few common-sense strategies that usually do the trick.
- For Headaches: A simple over-the-counter pain reliever like acetaminophen or ibuprofen often works wonders. Just be sure to check with your oncology team first to make sure it’s safe for you.
- For Constipation: Try to drink more fluids and, if you have the appetite, add high-fiber foods like prunes or whole grains to your diet. Your doctor may also suggest a gentle, over-the-counter stool softener.
- For Fatigue: This is your body telling you to slow down. Listen to it. Short naps can be incredibly restorative, but try to keep them from interfering with your nighttime sleep.
- For Insomnia or Restlessness: The best defense is a good offense—take your steroid medication early in the day. If you're still wired at bedtime, skip the caffeine and establish a calming routine to help you wind down.
Keeping track of these symptoms is incredibly helpful. When you're dealing with the side effects of anti-nausea medication, being organized allows you to communicate everything clearly and systematically to your doctor. To get a handle on this, you can master your next doctor visit with a review of systems.
When to Call Your Oncology Clinic
While many side effects are minor inconveniences, some things shouldn't wait. Your safety and comfort are our highest priorities, so we need to know immediately if something feels off.
It's crucial to report any new or worsening symptoms. Never assume a side effect is "normal" or that you just have to endure it. There are always other options we can explore to keep you comfortable.
Please call your clinic right away if you experience any of these:
- Severe constipation that lasts for more than a couple of days.
- A bad or persistent headache that isn't touched by over-the-counter medication.
- Any signs of an allergic reaction, like a rash, hives, or trouble breathing.
- Any "breakthrough" nausea or vomiting that happens even though you're taking your medication as prescribed.
This open communication is also why it's absolutely critical to tell your oncology team about every single medication you take. This includes vitamins, herbal remedies, and anything you buy over the counter. Many supplements can interfere with how both your chemotherapy and your anti-nausea drugs work, sometimes with serious results. To get more practical advice on symptom control, you can read our guide on managing side effects of cancer treatment.
The good news is that supportive care is constantly getting better. North America is projected to drive over 37% of the antiemetic drug market's growth through 2030, with the global market expanding at a 6.4% annual rate. This investment leads directly to better, more convenient options for patients. Today, outpatient drugs can successfully prevent vomiting in up to 90% of patients receiving high-risk chemo, which helps keep people out of the emergency room. You can discover more about these market insights and what they mean for patient care.
Complementary Strategies to Enhance Your Comfort

While your prescribed anti-nausea drugs are the cornerstone of your plan for CINV, they work even better when you pair them with other thoughtful comfort measures. Weaving some simple, proven habits into your day can add an extra layer of relief and help you feel more in control.
Think of these not as alternatives to your medication, but as powerful partners. At Hirschfeld Oncology, we see this as a team effort. We provide the medical strategy to manage your symptoms, and you can strengthen that plan with practical steps at home. Your comfort is always the goal.
Simple Dietary Adjustments
What you eat—and just as importantly, how you eat—can make a world of difference in how you feel. Strong smells or big, heavy meals are common triggers for nausea. Making a few changes here is one of the most impactful things you can do to support your anti-nausea medication plan.
Try these simple but effective shifts in your eating routine:
- Eat Small and Often: Instead of three large meals, aim for five or six small, snack-sized ones throughout the day. This keeps your stomach from getting too full or too empty, both of which can bring on that queasy feeling.
- Choose Bland Foods: Stick with simple, easy-to-digest foods. Things like crackers, toast, rice, and plain baked chicken are great choices. It’s wise to steer clear of anything too greasy, spicy, or sugary while you're in treatment.
- Stay Hydrated: Sip on clear fluids like water, broth, or diluted juice all day. Dehydration is a sneaky culprit that can make nausea much worse, so keeping fluids up is key.
For a much deeper look into nutrition during cancer care, we have a helpful guide on what to eat during chemotherapy.
Natural Aids and Mind-Body Techniques
Beyond what’s on your plate, a few other non-medical tools can help soothe your system. Many of our patients find real comfort in these gentle, natural aids that work right alongside their prescriptions.
These complementary approaches empower you to take an active role in your comfort. They address the mind-body connection, which can be a powerful force in managing treatment-related symptoms.
Some people get relief from sipping on ginger or peppermint tea, as both have a reputation for calming the stomach. Another go-to tool is acupressure, often through wristbands sometimes called "sea-bands." They apply gentle, constant pressure to a point on your inner wrist (the P6 point) that’s thought to ease nausea.
Don’t underestimate the power of calming your mind, either. Techniques like guided imagery, simple deep breathing exercises, or meditation can help settle your whole nervous system. By dialing down stress and anxiety, these practices can quiet the physical sensation of nausea, helping your anti-nausea drugs do their job even better.
Common Questions About Anti-Nausea Drugs
When you're facing cancer treatment, a lot of worries can crop up, and managing side effects is usually at the top of the list. We find that getting clear answers about anti-nausea drugs can make a world of difference for our patients' peace of mind.
Let's walk through some of the most common questions we hear every day at Hirschfeld Oncology. We want you to feel prepared and in control, knowing we're focused on keeping you comfortable.
Is Nausea Guaranteed With Chemotherapy?
No, not at all. Whether you experience nausea depends entirely on the specific chemotherapy drugs you're receiving. Some have a high likelihood of causing it, while many others have a very low risk.
Your oncology team figures this out right from the start. We look at your specific treatment plan and create a proactive anti-nausea strategy just for you.
Our goal with modern antiemetic medicine is always prevention. For the vast majority of our patients, we can successfully block nausea before it ever begins, which allows them to get through treatment much more comfortably.
Can I Use Over-The-Counter Nausea Medicine?
This is a really important one: you should never take any over-the-counter (OTC) medications, supplements, or herbal remedies without talking to us first.
Even things that seem completely harmless can cause problems. Many common OTC products can interfere with how your chemotherapy works or interact poorly with your prescribed anti-nausea drugs. These interactions might make your cancer treatment less effective or trigger unexpected and serious side effects. Always call the clinic before you take anything new—we're here to guide you.
What If My Anti-Nausea Drugs Aren't Working?
Please, call the clinic right away. Don't wait for things to get worse, and never feel like you just have to "tough it out." Your comfort is our priority, and breakthrough nausea is a medical issue we need to solve together.
If you're still feeling sick after taking your medication as prescribed, your team needs to know immediately. We have many different drugs and combinations we can try. Finding the perfect regimen sometimes takes a few adjustments, and your feedback is the most important tool we have to get it right.
How Does Hirschfeld Oncology Personalize My Treatment?
At Hirschfeld Oncology, we don’t use a one-size-fits-all approach. We start by looking at several factors: the specific nausea risk of your chemo regimen, your overall health, and even your personal history with things like motion sickness or nausea from past procedures.
From there, we build a multi-layered plan. This typically includes powerful IV antiemetics given right here during your infusion to head off immediate nausea. We then send you home with a precise schedule of pills to prevent any delayed symptoms from showing up later. Most importantly, we listen. After each cycle, we check in to see how you did, and we're always ready to tweak the plan to protect your quality of life.
At Hirschfeld Oncology, we believe that outstanding symptom management is a non-negotiable part of excellent cancer care. If you have questions about your treatment or are looking for a second opinion, our team is here to help you find a clear path forward. Explore your options by visiting us at https://honcology.com/blog.





.png)


.png)
.png)




