When we talk about the breast cancer survival rate by age, a general trend often appears. Younger women diagnosed with early-stage cancer tend to have higher survival rates, but the picture gets more complex for older adults. It's not a simple straight line, though—factors like how aggressive the tumor is and a person's overall health play a huge part at every age.
What Statistics Show About Age and Breast Cancer Survival
Trying to make sense of cancer statistics can feel overwhelming, but the main idea is actually pretty straightforward. Oncologists frequently refer to a measure called the 5-year relative survival rate.
This number compares people with the same type and stage of cancer to the overall population. Essentially, it tells us the percentage of patients who are likely to be alive five years after their diagnosis, helping to isolate the cancer's impact.
It's so important to remember that these are just averages based on data from thousands of people in the past. They offer a valuable big-picture perspective, but they can't predict what will happen for any one person. Your journey is entirely your own, influenced by your health, the specific details of your cancer, and how you respond to treatment.
For a broader look at the disease, you can find more information in our comprehensive guide on breast cancer care and treatment.
A Closer Look at the Numbers
Drilling down into the data, we see how age can influence survival statistics, sometimes in unexpected ways. For instance, younger women often have better outcomes when their cancer is caught at the earliest stages.
To put some concrete numbers to this, let's look at the 5-year relative survival rates for breast cancer (all stages combined) across different age groups.
5-Year Relative Breast Cancer Survival Rates by Age Group
Source: SEER 22, 2014-2020 data
As you can see, the rates are highest for women in their 40s, 50s, and 60s before declining slightly for older age groups.
When we focus on a very specific scenario, like stage 0 breast cancer, the differences become even more pronounced. A major study found that women aged 40 to 49 had a 100.0% 5-year overall survival rate, while women aged 50 to 59 had a rate of 95.0%. It’s a small but significant difference that underscores how age can be a factor.
This chart helps visualize that specific finding for stage 0 breast cancer.
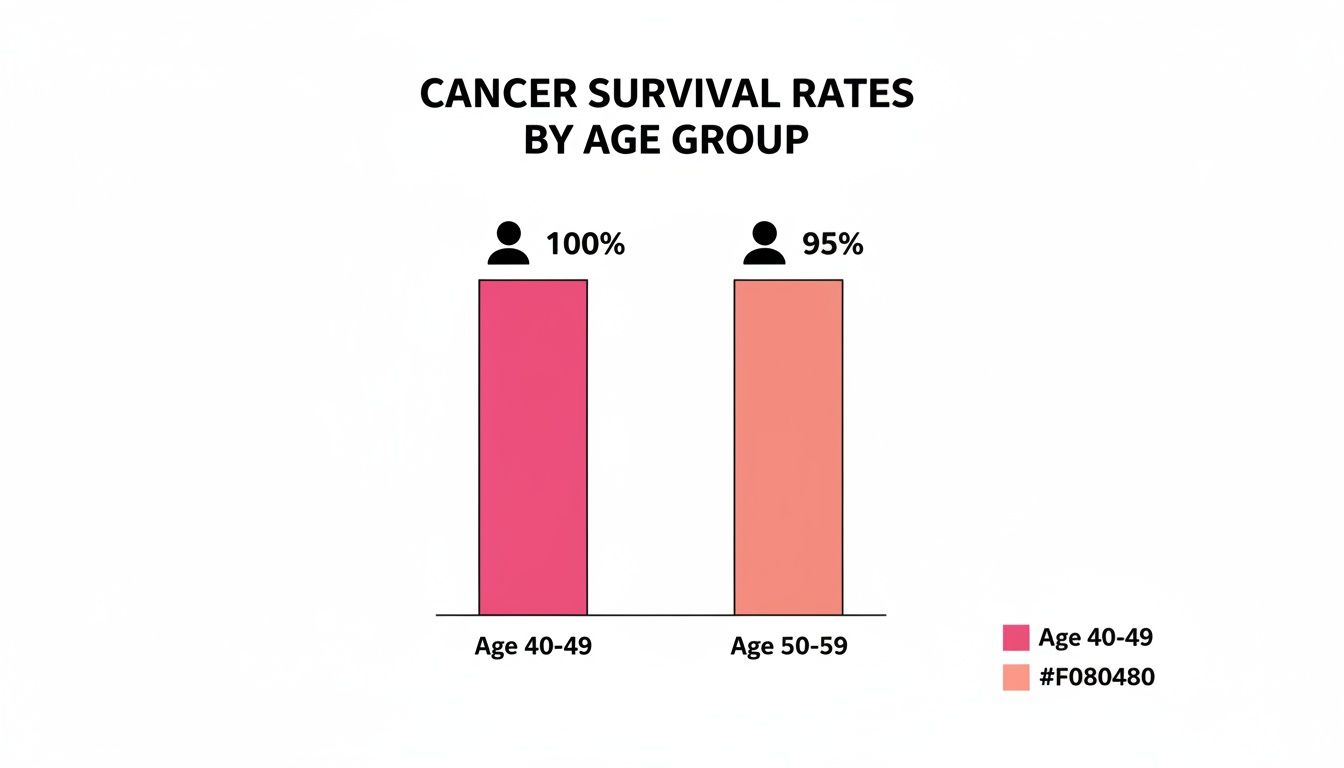
It’s clear from the chart that the younger group had a higher survival rate in this very early-stage scenario. This really sets the stage for a deeper question: why do these differences exist?
How to Read Survival Statistics Like an Expert

Cancer statistics can feel incredibly final, like a verdict has been handed down. But that’s not what they are. It’s better to think of them like a weather forecast based on past storms. They tell us what happened to large groups of people years ago, giving us a general sense of the climate—not a guarantee of rain or shine for your specific journey.
To feel in control, you first need to understand the language. The term you’ll hear most often is the 5-year relative survival rate, and it’s one of the most misunderstood concepts in oncology.
This particular statistic compares people with a specific type and stage of cancer to people in the general population of the same age and sex. Its whole purpose is to try and isolate the impact of the cancer itself.
Relative vs. Overall Survival
Let’s break this down. Imagine two groups of people. Group A has been diagnosed with breast cancer, while Group B is a similar group of people without breast cancer.
Overall Survival Rate: This simply tracks how many people in Group A are still alive after five years. It doesn't care why someone may have passed away—it could be from the cancer, or it could be from something totally unrelated, like a heart attack or a car accident.
Relative Survival Rate: This is where it gets more specific. It compares the survival of Group A to what would normally be expected in Group B over those same five years. It helps answer the real question: "Putting all other life risks aside, how did the cancer itself affect this group's chances of survival?"
So, when you see a 91% 5-year relative survival rate, it doesn't mean you have a 9% chance of dying from breast cancer. It means that people diagnosed with that cancer are, on average, 91% as likely to be alive five years later as their peers who don't have cancer.
Key Takeaway: Survival rates are a snapshot of the past. They are calculated using data from patients diagnosed at least five years ago, meaning they reflect the effectiveness of older treatments—not necessarily the more advanced options available to you today.
A Starting Point, Not a Final Word
This time lag is critical to remember. The data used to calculate the breast cancer survival rates you see today is based on therapies that were standard years ago. Cancer treatment moves fast. Today's approaches are often far more targeted and effective than what's reflected in those statistics.
This is why these numbers should never be seen as your destiny. They're a valuable tool for understanding the big picture and a great starting point for a conversation with your oncologist. Use them to get your bearings, but always remember that your personal path will be carved out by your unique health, your cancer's specific biology, and the modern, personalized care plan you build with your medical team.
The Key Factors That Influence Outcomes at Every Age
Survival statistics give us a useful bird's-eye view, but they don't capture the full picture of an individual's journey. When we look at the breast cancer survival rate by age, the differences we see are rooted in a complex mix of biology, overall health, and even how people interact with the healthcare system.
These factors often intertwine, shaping why a diagnosis for a 35-year-old can look so different from one for a 75-year-old. Digging into these reasons helps us move past the raw numbers and toward a more personalized understanding of treatment and prognosis. Four areas, in particular, explain why outcomes vary so much across a lifetime.
Tumor Biology
Not all breast cancers are created equal. The specific biological "personality" of a tumor—things like its hormone receptor status or the presence of certain proteins—is a major driver of how it behaves and how we treat it.
In Younger Women: We tend to see a higher frequency of more aggressive subtypes, like triple-negative breast cancer (TNBC) and HER2-positive breast cancer. These cancers are notorious for growing and spreading faster, which often means they require more intensive treatments, including chemotherapy.
In Older Women: Hormone receptor-positive (HR-positive) breast cancers are far more common. Because these tumors use estrogen or progesterone as fuel, they often respond very well to hormone-blocking therapies. While typically less aggressive, they still present their own unique challenges.
Stage at Diagnosis Matters
When a cancer is found is just as important as what kind of cancer it is. Catching it early almost always leads to more treatment options and a better prognosis, but age can play a big role in the timing of a diagnosis.
Younger women, for instance, are usually not in the standard age range for routine mammograms. Their cancer is often discovered only after a noticeable symptom appears, which can mean the disease is already more advanced. On the other hand, an older adult might dismiss a lump or symptom as just another part of getting older, delaying a visit to the doctor and also leading to a later-stage diagnosis.
The timing of a diagnosis is everything. It’s not just about the biology of the tumor, but about when we find it. An earlier diagnosis opens up a wider range of effective, often less intensive, treatment options.
The Impact of Comorbidities
As people get older, it's common to accumulate other health conditions, which we call comorbidities. Things like heart disease, diabetes, or kidney issues can profoundly impact a person's ability to tolerate certain cancer treatments.
An older patient with a heart condition, for example, might not be a good candidate for chemotherapies known to be hard on the cardiovascular system. Oncologists have to perform a careful balancing act: fighting the cancer aggressively while also protecting the patient's overall health and quality of life. Younger patients generally have fewer comorbidities, which allows them to handle more intensive treatment plans.
Data from the National Cancer Institute's SEER program clearly shows this intersection of age and health. Breast cancer cases peak at 27.4% in the 65-74 age group, and sadly, deaths follow a similar trend, with the median age at death being 71.
Let's break down how these factors typically appear across different age groups.
How Age-Related Factors Impact Breast Cancer Prognosis
This table compares how key biological and clinical factors typically present in younger versus older patients with breast cancer, influencing their survival outcomes.
As you can see, the patient's age doesn't just change the statistics; it changes the entire clinical picture, from the cancer's biology to the available treatment strategies.
Differences in Treatment Approaches
Finally, the treatment plan itself is almost always adapted based on a person's age and overall fitness. The goal is always the same—provide the best care possible—but what "best" means can be very different at various stages of life.
A younger patient may be willing to endure significant side effects from aggressive treatment to achieve the longest possible lifespan. For an older patient, the priority might shift toward a therapy that keeps the cancer in check while maintaining their independence and minimizing harsh side effects, placing a premium on their quality of life.
Tailoring Cancer Treatment to Your Stage in Life

Effective cancer treatment is never a one-size-fits-all solution. Think of an oncologist as a master tailor, meticulously crafting a strategy that fits your specific age, overall health, and personal goals. A plan that’s right for a 35-year-old might be completely wrong for a 75-year-old, even if their cancers look identical on paper.
This highly personal approach means the conversation about treatment goals can change dramatically depending on your age. For younger patients, we’re often focused on preserving fertility before chemotherapy begins or managing long-term side effects that could impact their lives for decades. The focus is almost always on aggressive, curative therapy to give them the longest, healthiest future possible.
For older adults, that conversation often shifts. The priority becomes finding the sweet spot between powerful treatment and maintaining a high quality of life. We have to carefully consider how therapies might interact with other health conditions or affect a person's ability to live independently and comfortably.
How Modern Therapies Adapt to Any Age
Thankfully, today's oncology toolkit is filled with treatments that allow for this deep level of personalization. Many of these newer approaches pack a serious punch against cancer but with fewer of the harsh side effects we used to see with traditional chemotherapy.
This is a critical piece of the puzzle, because the breast cancer survival rate by age is often tied to how well a person can tolerate their prescribed treatment.
- Targeted Therapy: These drugs act like smart missiles, homing in on the specific proteins or mutations that fuel cancer growth. Because they largely ignore healthy cells, their side effects are often much more manageable.
- Immunotherapy: Instead of attacking the cancer directly, this approach revs up your own immune system to recognize and destroy cancer cells. It’s a completely different way of fighting the disease and a game-changer for certain aggressive cancers.
- Gentler Chemotherapy: Not all chemo is created equal. Modern regimens often use lower doses or different drug combinations to dial back the toxicity while still keeping the cancer in check.
The American Cancer Society reports a 5-year relative survival rate for breast cancer of 91%, which dips to 86% at 10 years and 81% at 15 years post-diagnosis. These long-term numbers really drive home why we need sustainable treatment plans that people can stick with for years. You can find more details in the latest breast cancer statistics from the American Cancer Society.
Figuring out which of these therapies will work best comes down to understanding the cancer's unique subtype. We get that information by digging into its biology, which you can learn more about in our guide on what molecular testing for cancer reveals. Once we identify the precise drivers of a tumor, we can select the most effective treatment for that specific cancer.
Armed with this level of detail, you can have a much more meaningful conversation with your doctor about what the "best" treatment really means for you. It’s not just about fighting cancer—it's about building a path forward that honors your health and your life priorities, no matter your age.
Finding Hope and Personalized Care Beyond the Numbers

Statistics on the breast cancer survival rate by age can give you a general lay of the land, but an experienced oncologist is the guide who knows the terrain. They can help you navigate the specifics of your own diagnosis. Averages and percentages are useful starting points, but they can't possibly tell the full story of your health, your goals, or your life.
This is where a truly individualized approach to cancer care makes all the difference. At Hirschfeld Oncology, we partner with our patients, particularly those facing complex or advanced-stage diagnoses, to build treatment plans that go far beyond standard protocols. Our entire focus is on care that is as unique as the person receiving it.
We move past the one-size-fits-all mentality. Instead, we design highly specific treatment regimens aimed at achieving the best possible outcome while fiercely protecting your quality of life. That means we actively work to minimize toxicity and manage side effects, helping you live as fully as possible through it all.
Charting Your Own Path Forward
The story of what's possible after a breast cancer diagnosis is changing by the day. Advanced therapies are completely rewriting the script for patients of all ages, offering new hope where options may have once seemed limited.
These modern treatments allow us to design strategies with remarkable precision.
- Immunotherapy works by activating your own immune system to recognize and attack cancer cells, creating a powerful—and often more tolerable—treatment path.
- Targeted Therapy zeroes in on the specific molecular signals driving your tumor, which stops it from growing and spreading while largely sparing healthy cells.
- Low-Dose Chemotherapy can be a highly effective way to control the disease, often with fewer debilitating side effects, making it a sustainable option for many who need a gentler approach.
This level of personalization is everything. We believe an effective treatment plan has to align not just with the cancer’s biology, but with your personal values and life priorities, too. To learn more about how a long-term perspective can shape your treatment decisions, you might find our article on planning for life after breast cancer helpful.
Your journey with cancer should be defined by hope, collaboration, and a care plan built around you—not just the numbers. An innovative and dedicated oncology team can help you find a path forward that reflects your unique circumstances and goals.
By looking past the broad statistics, we can focus on what really matters: finding the right combination of therapies to give you the best chance at the best outcome. This is a collaborative process that empowers you to take an active role in your care, ensuring every decision is made with your total well-being front and center.
Your future is so much more than a statistic.
Common Questions About Age and Breast Cancer Survival
When you start digging into cancer statistics, a lot of questions pop up. It’s completely normal. Let’s tackle some of the most common ones about the breast cancer survival rate by age to help you feel more prepared when you talk with your doctor.
Does a Lower Survival Rate for Older Women Mean Treatment Isn’t Worth It?
Not at all. This is a really important point to understand. The broad statistics you see for older adults are often pulled down by other health issues they might be dealing with, not just the cancer. A lower number on a chart doesn't predict what will happen for you.
Oncology today is all about personalizing treatment to get the best results while protecting your quality of life. We have incredible, less-toxic options now, like targeted therapies, that can be very effective and much easier to handle. The goal is always to help you live longer and better, and many, many older adults do just that for years after a breast cancer diagnosis.
Are Younger Women More Likely to Have Their Cancer Come Back?
It's a fair question, and it comes from a real biological pattern. Younger women are sometimes diagnosed with more aggressive types of breast cancer, like triple-negative, which can have a higher chance of returning.
But that’s only half the picture. We now have powerful treatments designed specifically for these aggressive cancers, including newer targeted therapies and immunotherapies that have made a huge difference. Managing this risk comes down to a proactive surveillance plan and staying in close contact with your oncology team.
Key Insight: Cancer treatment is always moving forward. The statistics we have today are based on outcomes from treatments used years ago. They don’t fully reflect how successful the advanced therapies we're using right now actually are. The outlook is constantly getting better for everyone.
How Much Have Survival Rates Improved Over the Years?
The improvement has been dramatic across the board, for every age group. This is a direct result of huge leaps in both early detection and treatment. The creation of targeted therapies for specific cancer markers, like those for HER2-positive breast cancer, completely changed the game.
Because of this constant progress, the numbers are always a few steps behind the reality in the clinic. The treatments being used today are often far more effective than the ones that produced the five-year survival stats you see online. There's more reason for hope now than ever before.
What Should I Ask My Oncologist About My Age and Treatment Plan?
Being your own best advocate is one of the most powerful things you can do. When you meet with your doctor, you're a partner in the decision-making process. Here are a few questions to get the conversation started:
- Treatment Goals: "Given my age and specific diagnosis, what should our main goals for treatment be?"
- Therapy Options: "What treatments do you recommend for someone my age? What are the potential long-term side effects I should know about, especially concerning things like fertility or bone health?"
- Quality of Life: "How can we make sure my treatment plan is effective but also fits with what's important to me for my quality of life?"
- Newer Options: "Are there any newer treatments or even clinical trials that might be a good fit for me?"
Asking direct questions is the best way to make sure your care plan is truly tailored to your health, your cancer, and your life.
At Hirschfeld Oncology, we create personalized cancer treatment plans that see you as a whole person, not just a statistic. To learn more about emerging therapies and how we can help you map out a path forward, visit our blog.





.png)


.png)
.png)




