Some people notice it after a short walk to the bathroom. Others feel it when climbing stairs, folding laundry, or trying to hold a conversation without needing to sit down. You may be sleeping more than usual and still waking up worn out. Your family may say, “You just need to rest,” while you're thinking, “This feels different.”
That feeling often does have a name. One common reason is anemia from chemo.
As an oncology nurse, I want you to know two things right away. First, this is a real medical issue, not a personal weakness. Second, it's something your cancer team watches closely because there are ways to manage it. The more clearly you understand what's happening in your body, the easier it becomes to ask the right questions, notice important symptoms, and get help sooner.
Understanding Your Fatigue During Chemotherapy
Chemo fatigue isn't the same as ordinary tiredness. Ordinary tiredness usually improves after sleep or a quiet day. Fatigue related to treatment can feel heavy, slow, and frustrating. You may rest and still feel like your body has no reserve.
One common reason for that deep exhaustion is chemotherapy-induced anemia. Anemia means you don't have enough healthy red blood cells, or you don't have enough hemoglobin inside those cells. Hemoglobin is the part that carries oxygen. When oxygen delivery drops, your muscles and organs have to work harder for everyday tasks.
What this can feel like
You might notice:
- Walking feels harder: A trip across the room may leave you winded.
- Simple tasks take more effort: Showering, getting dressed, or making breakfast can feel like a project.
- Your brain feels foggy: Reading, focusing, or following a conversation may take more energy.
- Recovery is slow: Even after resting, you may not feel refreshed.
That's why patients often say, “I'm not sleepy. I'm drained.” That's an important difference, and it helps your team figure out what may be causing the problem.
Practical rule: If fatigue changes what you can safely do in a normal day, it's worth reporting. Don't wait until your next visit if it's getting worse.
There are also supportive tools outside the clinic that some people find helpful while they talk with their care team. If you're exploring gentle ways of managing fatigue with personalized supplement plans, keep in mind that supplements should fit your treatment plan and your lab results.
For practical daily habits, this guide on reducing chemotherapy-induced fatigue and boosting daily energy can help you think through pacing, rest, and small adjustments at home.
Why naming it matters
When patients understand that anemia can be part of treatment, they often feel less frightened and less alone. Instead of wondering whether they're “falling apart,” they can start tracking symptoms in a more useful way.
Try telling your team exactly what has changed. “I need to stop halfway up the stairs” is more helpful than “I'm tired.” “I feel lightheaded when I stand up” tells us something important. Clear details lead to better care.
Why Chemotherapy Can Cause Anemia
Chemotherapy is designed to attack fast-growing cancer cells. The problem is that some healthy cells also grow quickly, and chemo can affect them too. One of the main places this happens is the bone marrow.
Think of bone marrow as a factory inside your bones. That factory makes red blood cells, white blood cells, and platelets. Red blood cells are the oxygen delivery trucks. If chemo slows the factory, fewer trucks leave the building. Then less oxygen reaches the rest of the body.
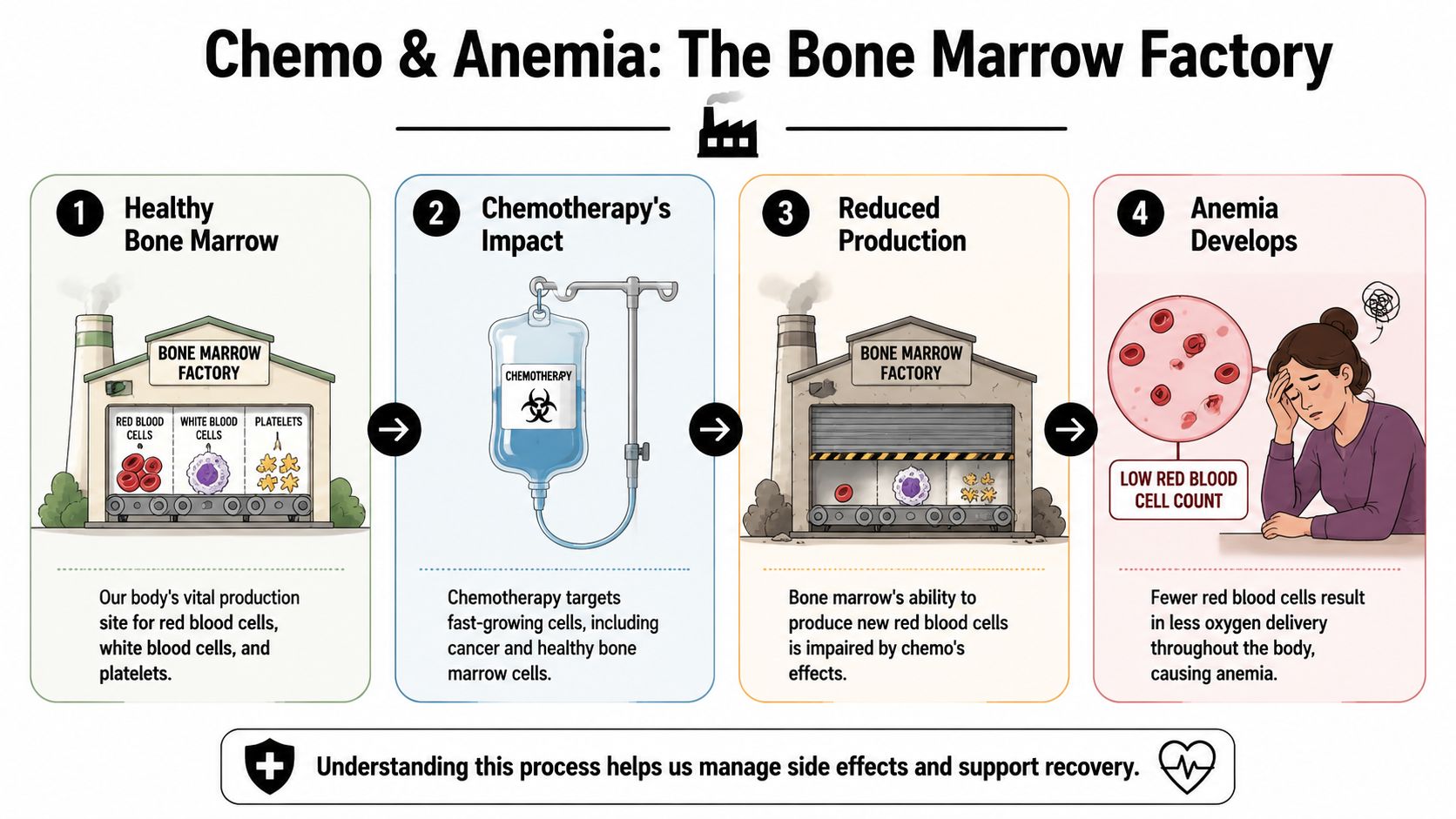
The bone marrow factory idea
Here's the simple version:
- Healthy marrow makes blood cells every day.
- Chemotherapy reaches cancer cells and marrow cells.
- Red blood cell production slows down.
- Oxygen delivery drops, and symptoms begin.
Some chemotherapy drugs are more myelosuppressive than others. Platinum-based drugs are often discussed in this context because they can strongly affect the marrow's ability to keep up with red blood cell production.
Why symptoms may build over time
Anemia from chemo often feels cumulative. Many families get confused here because a patient may feel “mostly okay” after one treatment, then much more drained after later cycles. That pattern makes sense. If the marrow is repeatedly stressed, it may not fully catch up between treatments.
A 2024 Frontiers in Medicine study found that chemotherapy-induced anemia developed in 75.3% of patients, with risk factors including older age, multiple chemotherapy cycles, and certain cancer types. That tells us something important. This isn't rare, and it's one reason oncology teams keep checking blood counts throughout treatment.
It's often easier to cope when you understand the logic. Chemo isn't “causing weakness” in a vague way. It may be lowering the blood's ability to deliver oxygen.
What families should know
Families sometimes encourage patients to “push through it.” Gentle activity can help some people, but anemia-related fatigue has a physical cause. If a patient says their legs feel heavy, their heart seems to race, or they need to stop and rest after a small task, believe them.
A helpful way to think about it is this: when oxygen delivery is reduced, the body starts spending extra effort on basic tasks. The patient isn't failing to keep up. Their body is working with less fuel.
Recognizing the Symptoms of Anemia
A lot of people expect anemia to mean “feeling a bit tired.” In real life, it can show up in several ways, and some are easier to miss than others.
You might wake up, walk to the kitchen, and feel strangely short of breath. You may stand up from the couch and need a second to steady yourself. You might notice that your hands feel cold even when the room seems warm. These are all clues that your body may not be getting the oxygen supply it needs.

Common symptoms patients describe
Here are symptoms I hear most often in clinic:
- Bone-deep fatigue: Not sleepy. Not lazy. Just depleted.
- Shortness of breath with activity: Especially when walking, showering, or climbing stairs.
- Dizziness or lightheadedness: Often worse when standing up quickly.
- Fast heartbeat or pounding heartbeat: Your body may try to compensate by moving blood faster.
- Pale skin or looking washed out: Sometimes noticed first by family.
- Cold hands and feet: Less oxygen delivery can make the body feel chilly.
- Headaches or trouble concentrating: The brain notices low oxygen too.
Why these symptoms happen
Every symptom circles back to the same issue. Red blood cells carry oxygen. When the supply drops, the body starts making adjustments.
Muscles tire faster. The heart may beat faster. The brain may feel foggy. Even small tasks can feel bigger than they should.
A foundational study in the Journal of the National Cancer Institute found a significant independent link between anemia and fatigue, with r=0.38, P≤0.02, and showed that quality-of-life declines worsened from 30% after the first cycle to 59% by the fourth. That matches what many patients describe. Symptoms can build gradually, then suddenly interfere with daily life in a very noticeable way.
If you're saying, “I don't feel sick exactly, I just can't do what I could do last week,” that's useful information. Tell your team that exact sentence.
When to speak up
Don't wait for symptoms to become dramatic. Call if:
- Breathlessness is new or getting worse
- You feel faint when you stand
- Your heart feels like it's racing
- You can't do normal self-care without stopping
- Family members notice a clear change in your color, stamina, or alertness
Patients sometimes underreport symptoms because they don't want treatment delayed. But early reporting gives your team more options, not fewer.
How Doctors Diagnose and Monitor Anemia
Most patients already know they're getting frequent blood tests during treatment, but many aren't told exactly what the team is looking for. Once you understand that, the process feels less mysterious.
A big part of monitoring anemia from chemo is the complete blood count, often called a CBC. This test gives your team a snapshot of how your bone marrow is doing.

The lab values you'll hear about
Two terms come up often:
- Hemoglobin, or Hgb: This tells us about the oxygen-carrying protein in red blood cells.
- Hematocrit, or Hct: This reflects how much of your blood is made up of red blood cells.
You don't need to memorize every detail. What matters is that your oncology team watches trends, not just one isolated number. A value that's acceptable for one person may be concerning in another person who has new symptoms, heart strain, or rapid changes between visits.
Why doctors may order more than a CBC
Not every low blood count is caused by the exact same problem. Chemo can suppress the marrow, but doctors also look for treatable contributors.
According to ASCO/ASH guidance summarized here, chemotherapy-induced anemia primarily results from myelosuppressive effects on the bone marrow, particularly with platinum-based agents, and management starts with screening for iron, folate, and B12 deficiencies to help choose the most effective intervention.
That's why your team may add tests beyond a CBC. They may be asking:
- Is iron available, or is there a functional iron deficiency?
- Is there a B12 or folate issue that needs correction?
- Is the pattern typical for chemo, or does it need a closer look?
If your doctors ever mention a marrow evaluation, this overview of the bone marrow biopsy procedure can help make the process less intimidating.
Sometimes it also helps to hear a visual explanation of how blood counts are measured and interpreted:
What to ask when reviewing labs
Bring a notebook, or ask a family member to write things down. Useful questions include:
- What is my hemoglobin today?
- Has it been trending down, stable, or improving?
- Do my symptoms match the lab result?
- Are you checking iron, B12, or folate?
- What change would make you recommend treatment?
Numbers matter, but symptoms matter too. A lab result always means more when it's paired with how you're actually feeling.
Exploring Your Treatment Options for Anemia
Treatment depends on why the anemia is happening, how severe your symptoms are, how quickly the count has changed, and what your overall cancer plan looks like. This is why two patients can both have anemia and still get different recommendations.
Some people need quick symptom relief. Others need support for red blood cell production over time. Others benefit most from correcting iron problems that are limiting recovery.
The main treatment paths
Red blood cell transfusion is often the fastest way to improve symptoms when anemia is causing significant shortness of breath, weakness, or other urgent problems. It doesn't fix the underlying reason the anemia developed, but it can raise oxygen-carrying capacity quickly.
Erythropoiesis-stimulating agents, often called ESAs, work differently. They signal the body to make more red blood cells. These medicines are used selectively, and the decision depends on treatment goals and safety considerations.
Iron treatment may sound simple, but the details matter. Some patients have iron on paper yet still can't use it well because of inflammation and the way cancer treatment affects iron handling. In those situations, IV iron may help more than oral iron.
Chemotherapy adjustments are also part of the conversation. If blood counts keep dropping, the oncology team may adjust timing or dosing so treatment remains tolerable and safe.
Comparing Anemia Treatment Options
| Treatment | How It Works | Best For | How It's Given |
|---|---|---|---|
| Transfusion | Replaces red blood cells directly | People with significant symptoms or a need for quicker relief | Through an IV |
| ESA | Encourages the body to produce more red blood cells | Selected patients whose care team feels it fits their treatment goals | Usually by injection |
| Iron therapy | Replaces iron needed for red blood cell production | People with iron deficiency or functional iron problems | By mouth or through an IV |
| Chemo adjustment | Reduces marrow stress so recovery can happen | People whose blood counts are repeatedly limiting treatment | Changes to schedule or dose |
When IV iron becomes part of the plan
This is an area where patients often get confused. They hear “eat more iron” or “take an iron pill,” and sometimes that helps, but not always. During active cancer treatment, the body may not absorb or use oral iron effectively enough.
If you'd like a plain-language refresher on fighting fatigue with iron and B12, it can help you understand why these nutrients matter. Just remember that supplements aren't interchangeable with medical treatment. Your labs and your symptoms determine what actually fits.
What decision-making often looks like
Your doctor may weigh questions like these:
- How severe are the symptoms right now?
- Is the anemia mainly from marrow suppression, iron problems, or both?
- Is a rapid fix needed, or is a steadier strategy better?
- Will anemia start delaying cancer treatment if we don't act?
Sometimes the best plan is one treatment. Sometimes it's a combination. The key is that you don't have to guess what the plan means. Ask your team to explain the goal of each option in one sentence. For example: “This is for quick relief,” or “This is to help your body rebuild.”
Practical Steps for Managing Anemia Symptoms
Medical treatment matters most, but what you do at home also makes a real difference. Good symptom management isn't about “toughing it out.” It's about using your energy carefully and reducing risks while your team works on the medical side.

Daily habits that help
Try to make your day easier, not fuller.
- Pace your effort: Break larger tasks into smaller ones. Shower, then rest. Fold a few clothes, then sit down.
- Sit whenever you can: Sit to brush your teeth, prep food, or get dressed if standing makes you dizzy.
- Stand up slowly: This can help if you feel lightheaded.
- Keep essentials nearby: Water, medications, snacks, a phone charger, and a blanket should be within easy reach.
- Use your best hours wisely: If mornings are easier, do the most important task then and let the rest wait.
Food and fluids matter, but they're not the whole treatment
Patients often ask if diet alone can fix anemia from chemo. Usually, no. But food and hydration still support recovery.
Aim for regular eating, even if meals are small. Include protein when you can. Drink fluids through the day, especially if treatment side effects have reduced your appetite. If eating is hard, this guide on what to eat during chemotherapy may help with practical choices.
Try this sentence with family: “I may look like I'm resting, but I'm actually managing my energy so I can do the things that matter most.”
How modern treatment fits into home care
Home strategies work best when they're paired with good medical follow-up. That's especially true when fatigue is tied to functional iron deficiency, where the body can't use iron efficiently even when iron is present.
Emerging 2024 to 2025 data summarized in this review shows that IV iron can correct functional iron deficiency in 60% to 80% of advanced solid tumor cases, with hemoglobin rising by 1 to 2 g/dL without transfusions, helping some patients stay on full-dose, low-toxicity regimens. For patients trying to keep treatment on schedule while limiting extra strain, that's a hopeful and practical development.
Safety reminders
Call your team sooner rather than later if symptoms are changing fast. At home, keep the focus on safety:
- Don't drive if you feel faint or unusually weak
- Use support when showering if balance feels off
- Ask for help with stairs, laundry, and grocery bags
- Keep a symptom log so changes are easier to describe
Small changes in routine can protect your strength while treatment decisions are being made.
Partnering with Your Oncology Team
The patients who do best with symptom management are not the ones who stay silent. They're the ones who report changes clearly, ask direct questions, and let the team know what daily life looks like.
You are not “bothering” your nurse by calling about worsening fatigue, breathlessness, dizziness, or a pounding heartbeat. Those details help your team decide whether to repeat labs, check nutrient levels, adjust treatment, or bring you in sooner.
Questions worth asking
Bring these to your next visit:
- What is my current hemoglobin, and how has it changed over time?
- Do my symptoms fit anemia, or could something else also be contributing?
- Are you checking iron, folate, and B12?
- At what point would you recommend transfusion, IV iron, an ESA, or a chemo change?
- What symptoms should trigger an immediate call?
- If my count drops again, what is our next step?
Red flags that need urgent attention
Call right away, or seek urgent care if instructed, for:
- Shortness of breath at rest
- Chest pain
- Fainting
- Confusion or sudden weakness
- A rapid worsening in fatigue that makes basic self-care unsafe
The most useful update you can give is concrete. “I had to stop twice walking from the bedroom to the kitchen” tells your team much more than “I'm more tired.”
Families can help by keeping notes, tracking symptoms between visits, and speaking up if the patient minimizes what's happening. Good cancer care works best when the patient, caregiver, nurse, and doctor are all working from the same honest picture.
If you or a loved one is dealing with anemia from chemo and needs thoughtful support during complex cancer treatment, Hirschfeld Oncology offers research-informed guidance, close monitoring, and patient-centered care for people facing advanced or treatment-resistant cancers in Brooklyn and across New York City.





.png)


.png)
.png)




